Introduction
Today, composite resins are continually being developed and enhanced to meet the increasing aesthetic demand. Both the colour harmony of the composite resin and the capacity to retain this harmony for a long time are critical for achieving a natural appearance. The ability of the composite restoration to reflect the light arriving at its surface is proportional to how bright the surface is and how long it stays that way (1). Roughening the surface of restorative materials can result in irritation of the surrounding tissues and aesthetic deterioration caused by plaque accumulation. The difference of 0.3 microns on the surface can be distinguished from the tip of the human tongue and negatively affects comfort (2).
Tooth brushing is the most prevalent oral hygiene practice to prevent caries lesions. Brushing teeth with whitening toothpastes for whitening teeth is one of the preferred, easy to apply and economical methods used today. Abrasives are used in whitening toothpastes to remove stains from the tooth surface. In general, the effectiveness of cleaning the teeth is directly related to the hardness, size, shape and concentration of the particles in the toothpaste, the characteristics of the toothbrush and the pressure applied during brushing the teeth. In order to clean the teeth effectively in dentistry, the abrasiveness of the materials used should be up to a certain level (3, 4). The International Standards Organization (ISO) determined the dentin abrasiveness value (RDA) in toothpastes used should not exceed 250 (5,6). Generally, whitening toothpastes have medium (60-100 RDA) or high (RDA>100) abrasiveness (7). Toothpaste abrasives vary widely in composition, and some formulations are more abrasive than others. Sometimes, even for a good cleaning and stain removal, toothpastes can abrade the tooth structure more than it should (8). Whitening toothpastes are cosmetic products that are readily available on the market and used without the supervision of a dentist (9). In addition to chemical whiteners such as hydrogen peroxide and carbamide peroxide, these toothpastes contain abrasives such as calcium carbonate, calcium phosphate, hydrated silica, calcium pyrophosphate, alumina, perlite and sodium bicarbonate (10).
Studies have reported that the colour of restorative materials in the mouth may change over time with the oxidation of amine compounds and surface pigments. Abrasives in toothpastes can cause discolouration over time, especially by creating abrasions on the surface of resin composite materials. The colour stability of composite resins depends on a variety of intrinsic and extrinsic factors. The most important of the internal factors is the degree of monomer conversion of the resin matrix (11), while external factors are various foods and beverages such as coffee, wine, tobacco and ketchup which may cause discolouration on the surface of composite restorations (12,13).
The effects of commercially available whitening toothpastes on the surface of composite restorations are not yet completely known. As a result of long-term use of whitening toothpastes, the roughness that may occur on the surface of composite restorations and discolouration after consumption of beverages such as coffee are an important problem. The roughness that occurs on the restoration surfaces may also cause more discolouration and plaque accumulation, that results aesthetic problems and adversely affects the longivity of the restoration. The aim of this study is to evaluate the colour and the roughness changes on the surfaces of the giomer, microhybrid and nanohybrid composites after exposing to external colouration with coffee and brushing with whitening toothpastes containing silica and hydrated silica as an abrasive. The null hypothesis of this study is that with the use of different whitening toothpastes in the colouring-brushing cycle process, the degree of colour change on the surface of the restorative materials will be similar and there will be no increase in surface roughness.
Materials and methods
Preparation of samples
In the current in-vitro study, A2 colour, giomer (Beautifil II, Shofu, Japan), microhybrid composite (Arabesk, Voco, Germany) and nanohy- brid composite (Herculite, Kerr, USA) restorative materials were used. The contents of the materials are shown in Table 1. In order to compare before-after measurements with 95% confidence level (α= 0.05) and 80% power (β: 0.20), the minimum number of samples to be taken per group was calculated as 10 when the effect size was predicted as 1.04. The materials were placed in a specially prepared 2mm thick and 10mm wide polyethylene Teflon mould and lightly pressed with a glass plate to remove excess. The polymerization was carried out with a II. generation LED light device (Guilin Woodpecker Medical Instrument Co., Guilin, China) which produces light intensity with of 800 mW/cm² and a wavelength of 460-480nm. Each sample was cured for 20 seconds (8 J/cm²) in accordance with the manufacturer's recommendations. Thirty disc-shaped samples obtained from each material were polished with the help of coarse, medium and fine polishing discs (OptiDisc, Kerr, USA) in accordance with the manufacturer's instructions. Subsequently, all samples were kept for 24 hours in distilled water at 37°C. After those 24 hours, each material was divided into three subgroups (n=10) and the basic colour values (T0) of each sample in the group were measured and recorded using a spectrophotometer (VITA Easyshade V, VITA Zahnfabrik). Initial surface roughness values (Ra0) were determined and recorded using a mechanical profilometer (Mitutoyo SJ-210, Japan).
Table 1 Restorative materials used in the study.
| Composite | Type | Compound | Manufacturer |
|---|---|---|---|
| Arabesk | Microhybrid | Resin: Bis-GMA, TEGDMA, UDMA Particles Size: 0,5-2μm, Filler: Silicon dioxide, Barium-/strontium borosilicate, 76.5% by weight, 60% by volume. | Voco,Germany |
| Herculite XRV Ultra | Nanohybrid | Resin: Bis-GMA, TEGDMA Particles Size: 0,05μm Filler: Colloidal Silica, Barium-aluminium-silicate glass, 78% by weight. | Kerr Corp., Orange, CA, USA |
| Beautifil II | Giomer | Resin: Bis-GMA, TEGDMA, UDMA Particle Size: 0,8μm (avarage), 10-20nm (nanofillers) Filler: S-PRG, 83.3 % by weight, 68.6% by volume. | Shofu, Kyoto, Japan |
Coloring procedure
The samples were kept in a coffee solution (3.2g in 250mL of boiling water) for 12 days (Nescafe Gold, Nestle, Switzerland) which was renewed every other day and prepared in separate containers for each group according to the manufacturer's recommendations. Total holding time and coffee concentration were calculated by taking the average daily coffee consumption as 3.2g and the average time as 15 minutes as reference, and calculating it to correspond to the 1-year coffee consumption (14).
Brushing procedure
Prepared composite samples were brushed with 3 different whitening toothpastes (Opales- cence Cool Mint With Fluoride (OCM), Colgate Optic White Extra Power (COW), Signal White Now Gold (SWN)) using an electric toothbrush (Oral B Clean DB04, Procter & Gamble, USA). The composition of toothpastes is described in Table 2. The brushing process was continued for 2.5 minutes once a day for 12 days for each sample kept in the coffee solution. To maintain standardization, this process was carried out by a single operator. Brushing times in the population range from 30 to 180 seconds, with an average brushing time of about 60 seconds. The maximum contact time for each tooth was determined as 5 seconds. Thus, the colouring and brushing process continued for 12 days, corresponding to approximately 1 year (15).
Taking colour measurements
A spectrophotometer was used to measure the colour of all samples by the same operator (VITA Easyshade V, VITA Zahnfabrik) with the aid of D65 illumination on a standard white background and calculating the CIEDE2000 colour coordinates. The probe tip was measured from 4 different points of the sample at the same distance from the center and recorded by taking the average. Colour measurements were performed: before the colouring-brushing cycle began (T0) and after the 12-day colouring-brushing cycle had ended (T1). The formula CIEDE2000 (ΔE00) was used to calculate colour changes (16).
ΔL', ΔC' and ΔH' describe changes in colour, hue and lightness differences between two samples. SL, SC and SH are weighing functions for colour, hue and lightness parameters. KL, Kc, and KH are factors regulated by different observed parameters and were accepted as 1 according to other studies (17). The CIEDE2000 colour difference formula's parametric factors are set to 1 in this study. The detectability threshold was determined as ΔE00>0.8 units and the clinical acceptability threshold as ΔE00≤1.8 units (16).
Surface roughness measurements (RA1) after brushing
After brushing the materials with whitening toothpastes, the final surface roughness values (Ra1) were also measured using a mechanical profilometer (Mitutoyo SJ-210, Japan) and the obtained values were recorded.
Statistical analysis
For overall variables, the data were reported as median (min-max) values. The Shapiro Wilk test was used to determine normality. The related data of colour change and roughness were not normally distributed (p<0.05). The Kruskal Wallis H test was used to compare the non-normally distributed data (i.e., colour change and roughness) among the groups/subgroups. When significant differences were found in colour change and roughness, the Mann Whitney U test with Bonferroni correction was used to perform multiple comparisons. P<0.05 values were considered as significant. IBM SPSS statistics versión 26.0 for Windows was used for statistical analysis.
Table 2 Toothpastes used in the study and their ingredients.
| Whitening Toothpastes | Compound | Manufacturer |
|---|---|---|
| Opalescence Cool Mint with Fluoride(OCM) | Glycerin, Water, Silica, Sorbitol, Xylitol, Aroma, Poloxamer 407, Sodium Lauryl Sulphate, Carbomer, Sodium Benzoate, Sodium Fluoride, Sodium Hydroxide, Sucralose, Xanthan Gum, FD&C Blue No. 1, FD&C Yellow No. 5 (Cl 19140 (Tartrazine, Yellow Pigment). | Ultradent Products, USA |
| Colgate Optic White Extra Power (COW) | Water, Hydrated Silica, Sorbitol, PEG-12, Pentasodium Triphosphate, Tripotassium Pyrophosphate, Aroma, Sodium Lauryl Sulfate, Cellulose Gum, Potassium Hydrooxide, Phosphoric Acid, Cocamidopropyl Betaine, Sodium Fluoride, Sodium Saccharin, Xanthan Gum Lemon, Cl74160 (Blue Pigment). | Colgate-Palmolive, USA |
| Signal White Now Gold (SWN) | Water, Hydrogenated Starch Hydrolyzate, Hydrated Silica, PEG-32, Sodium Lauryl Sulphate, Lecithin, Oleic Acid, Capryl Glycol, Lauryl Alcohol, Limonene, Cl 74160 (Blue Pigment), Cl 74260 (Green Pigment), Cl 77891 (Titanium Dioxide, Whitening Pigment. | Signal Unilever, UK |
Results
Results of surface roughness
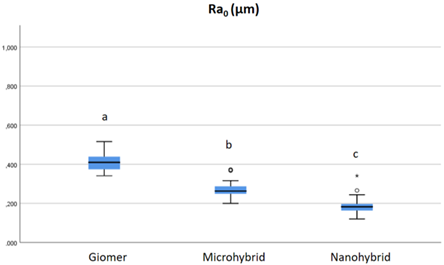
The median values of initial surface rough- ness (Ra0) of the main groups of restorative materials are shown in Figure 1.
When the data obtained from the comparison of giomer, microhybrid and nanohybrid composite main groups were evaluated; it was observed that the group with the lowest initial surface rough-ness was the nanohybrid composite group, while the group with the highest value was the giomer group. A significant difference was found between the main groups in the pairwise comparison of the restorative materials (p<0.05).
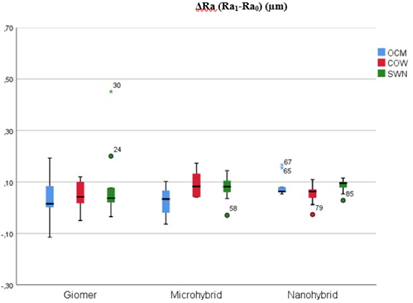
The first surface roughness values (Ra0) of the subgroups of the restorative materials and the end surface roughness values (Ra1) after brushing with OCM, COW and SWN are shown in Table 3, and the median ΔRa (Ra0-Ra1) values of the subgroups are shown in Figure 2.
Table 3 Median Ra0 and Ra1 values of subgroups.
| Restorative Materials | Whitening Toothpastes | n | Ra0 Median (minimum-maximum) (µm) | Ra1 Median (minimum-maximum) (µm) |
|---|---|---|---|---|
| - | OCM | 10 | 0.412ª (0.341-0.454) | 0.457ª (0.296-0.601) |
| Giomer | COW | 10 | 0.397ª (0.344-0.425) | 0.443ª (0.316-0.545) |
| - | SWN | 10 | 0.444ª (0.342-0.516) | 0.474ª (0.404-0.808) |
| - | OCM | 10 | 0.292ᵇ (0.243-0.373) | 0.334ᵇ (0.282-0.358) |
| Microhybrid | COW | 10 | 0.265ᵇ ͨ (0.2-226) | 0.346ᵇ (0.302-0.446) |
| - | SWN | 10 | 0.252 ͨ (0.218-0.287) | 0.338ᵇ (0.257-0.363) |
| - | OCM | 10 | 0.182 ͩ (0.12-0.266) | 0.252 ͨ (0.223-0.353) |
| Nanohybrid | COW | 10 | 0.190 ͩ (0.151-0.341) | 0.259 ͨ (0.22-0.314) |
| - | SWN | 10 | 0.174 ͩ (0.13-0.197) | 0.252 ͨ (0.224-0.295) |
| p value | - | - | <0.001 | <0.001 |
Different lowercase given as superscript in the same column indicate statistically significant difference from other groups.
In the evaluations made, in the giomer group; 0.045µm increasing in OCM was not statistically significant (p>0.05). The 0.046µm increasing caused by COW and the 0.030 µm increasing caused by SWN created a significant difference between the initial-finish values (p<0.05). In the microhybrid composite group; 0.042µm increasing in OCM was not statistically significant (p>0.05). The 0.081µm increasing caused by COW and 0.086µm increasing created by SWN created a significant difference between the initial-finish values (p<0.05). Finally, in the nanohybrid composite group; 0.070µm increasing caused by OCM, the 0.069µm increasing caused by COW and 0.078µm increase caused by SWN created a significant difference between the initial-finish values (p<0.05).
Results of colour analysis
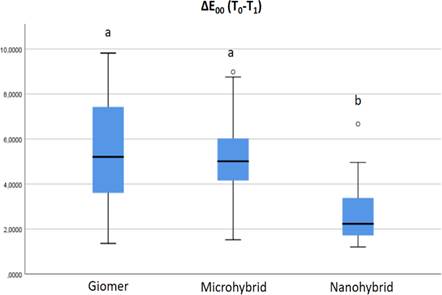
The median values of ΔE00 of the main groups after the colouring-brushing cycle are shown in Figure 3. Accordingly, there was a statistically significant difference between the giomer, microhybrid and nanohybrid composite groups to which OCM, COW and SWN were applied (p<0.05). There was no significant difference between the giomer and microhybrid composites in the pairwise comparison of the groups (p>0.05). There was a statistically significant difference between the giomer and nanohybrid composite group and between the microhybrid and nanohybrid composite group (p<0.05). While the colour change of the giomer group (ΔE00=5.204) has the highest value, the lowest colour change belongs to the nanohybrid composite group (ΔE00=2.229).
The median ΔE00 values of the subgroups are shown in Table 4. Colour changes in all groups were above the clinically accepted threshold after a 12-day colouring-brushing cycle (ΔE00>1.8). The least colour change was observed in the COW applied nanohybrid composite group, with this change being significantly different from the microhybrid and giomer material subgroups (p<0.05). The group with the highest colour change after the colouring-brushing cycle was the COW applied giomer group, with this difference being significantly different from the nanohybrid composite subgroups (p<0.05). The OCM subgroup of microhybrid composite was significantly different from nanohybrid composite subgroups except the SWN subgroup (p>0.05).
Table 4 Median ΔE00 values of subgroups.
| Restorative Materials | Whitening Toothpastes | n | ΔE00 (T0-T1) Median (Minimum-Maximum) | p value |
|---|---|---|---|---|
| - | OCM | 10 | 5.647 (1.36-8.953)ª | - |
| Giomer | COW | 10 | 5.943 (2.253-8.181)ª | - |
| - | SWN | 10 | 4.516 (2.537-9.819)ª | - |
| - | OCM | 10 | 4.683 (1.522-8.753)ªᵇ | - |
| Microhybrid | COW | 10 | 5.043(1.902-8.978)ª | <0.001 |
| - | SWN | 10 | 4.983 (3.734-6.422)ª | - |
| - | OCM | 10 | 2.22 (1.206-6.667) ͨ | - |
| Nanohybrid | COW | 10 | 1.814 (1.449-3.796) ͨ | - |
| - | SWN | 10 | 2.949 (1.716-4.957)ᵇ ͨ | - |
Different lowercase given as superscript indicate statistically significant difference from other groups.
Discussion
The increase in expectations in today's aesthetic understanding and the search for solutions to the discolouration of the teeth have caused an increase in the variety of teeth white ning products. Whitening toothpastes significantly affect surface roughness and discolouration on restorations compared to conventional toothpastes (18). This study evaluated the colour change and surface roughness of coffee-coloured giomer, microhybrid and nanohybrid composites after using whitening toothpastes. In the present study, top whitening toothpastes of some well- known oral and dental health brands were preferred. The null hypothesis of the study was rejected because of the different degrees of colour change and the increase of surface roughness after the use of whitening toothpastes on coloured restorative materials.
When the initial surface roughness (Ra0), finished surface roughness (Ra1) and colour change values (ΔE00) were examined, it was seen that the giomer had the highest values in all three parameters while the nanohybrid composite group had the lowest values. This condition could lead to the conclusion that the surface roughness and colour change parameters are proportional, similar to the findings of Kocaagaoglu et al. (19). When we considered the measured surface roughness values of the samples consisting of a total of 9 subgroups after the colouring-brushing cycle applied to the materials in our study, OCM was the only toothpaste that did not cause a significant increase in roughness on the giomer and microhybrid composite surfaces. Statistically significant increases were observed in surface roughness in all other groups. Another remarkable point was that the surface roughness change of the giomer restorative material was generally less than that of other materials. The groups with the highest difference in surface roughness change were the microhybrid composite subgroups brushed with COW and SWN. Yin et al. (20) tested the surface roughness formation efficiency of whitening toothpastes on giomer, microhybrid and nanofil composites and stated that the group with the least increase in surface roughness was the giomer, and the group with the highest increase was the microhybrid composite group, as in our study. Another important point they expressed in their study referred to the substances in the toothpaste; that abrasives played the main role in creating surface roughness differences. In our study, when the Ra1 values of the groups were examined, there was no significant difference between the subgroups of each main group, but there was a significant difference between the main groups representing each restorative material. This shows that the surface roughness of the toothpaste changes with the change in the structure of the restorative material to which it is applied, regardless of the abrasive feature of the toothpaste. In parallel with this result, Roselino et al. (9) in their study that tested whitening toothpastes on composites containing microfil and nonofil particles, stated that the surface roughness was not affected by toothpaste abrasiveness and was associated with restorative materials.
In the present study, colour differences were calculated using the CIEDE2000 formula. The clinical acceptability threshold was taken as ΔE00≤1.8 (21). The CIEDE2000 system is a good indicator of perceptibility and acceptability of colour changes (17,22). Perceptibility refers to the perception of the smallest colour difference by the human eye, while acceptability refers to the recognition of the colour between a tooth and an adjacent restoration as being similar (23). Colour changes were evaluated by making comparisons with 50%:50% detectability and 50%:50% acceptability thresholds. In our study, a statistically significant difference was observed in the ΔE00 values between the groups, and the ΔE00 values of all groups were found above the clinical acceptability threshold ΔE00≤1.8 units.
The hydrophilic structure of the restorative materials, which are different from each other, is one of the factors affecting the colour changes. The hydrophilic structure is effective in the absorption of water and other materials in the solution (24). Previous studies have reported that Substances such as tea, coffee and red wine may be important factors in the discolouration of teeth (17,22). Materials such as tannin and caffeine in coffee can penetrate deep into the restorative materials and cause colour changes. A significant part of the staining takes place in the first week and can reach a depth of 5µm (17,23). In the current study, coffee was used as a colouring agent and the samples were kept in a daily renewed coffee solution for 12 days and brushed every other day with whitening toothpastes. The average brushing time in the population is approximately 60 seconds and the maximum contact time for each tooth is 5 seconds. Brushing done for 12 days for 2.5 minutes/day corresponds to a period of 1 year under normal conditions (15). In the present study, the most colour change was observed in the giomer restoration group (OCM and COW subgroups), while the least change was observed in the nanohybrid composite group. In order to imitate the coloura- tion-brushing cycle in daily life, daily brushing with whitening toothpastes was applied to the samples after daily colouring with coffee solution. This made it possible to compare the effect of whitening toothpastes on colour change within the main groups, but limited the comparison of the effect between the main groups. This is because the degree of colour change may depend on the resistance of the material to coloration as well as the effectiveness of the pastes. In a study the authors stated that the composition of the material and the size of the filler particles are among the factors affecting the colouration (25). The lower colour change in the nanohybrid composite group in the present study can be explained by the low surface roughness due to the nano-filled structure of the material and therefore the low colour retention. In addition, the distribution of the particles and the type of resins in organic matrix are the factors that may affect the surface roughness (26). In a similar study, Chong et al. (27), when they tested the effect of whitening toothpastes on colour change on giomer, microhybrid and nanohybrid composites, stated that giomer was the group with the most colour change since the organic matrix part was higher than the others. In another study comparing whitening toothpastes and traditional toothpastes, composites and compomers were used.
According to the findings of that study, it was shown by the researchers that the surfaces of the compomers exposed to the same processes are more roughened and coloured than the composites (18). These studies show that more colouration can occur in glass ionomer-containing materials. In our study, the highest colour changes were observed in the OCM and COW subgroups in the giomer group, but this change was statistically significantly higher than only the nanohybrid composite subgroups. Choi et al. (28) who investigated the effects of different beverages on the wettability and colour stability of restorative materials showed that after five days of submersion, coffe was most significantly affected the contact angle of the giomer material and giomer had the highest reduction rate of colur change when compared with resin composite and compomer. Based on the findings of the current and similar studies, high wettability with coffe solution and the presence of hydrophilic poliacid-modified monomers in the giomer can be shown as the cause of more colouration.
In the same main group, the subgroups that provided the most colour change were the COW subgroup of the giomer and microhybrid composite main groups, and the SWN subgroup of the nanohybrid composite main group. Both toothpastes contain hydrated silica as an abrasive leads to the thought that hydrated silica may be more effective than the silica contained in OCM on colour change.
Whitening toothpastes also contain special chemical components in their structure to remove stains on the surface, and this type of toothpaste aims at the highest level of cleaning and minimal wear. Researchers have stated that the type of abrasive material in the paste and the size of the particles are directly proportional to the abrasiveness of the toothpaste (29). In another study, it was stated that not only abrasives, but also detergents added to the paste potentially cause dentin loss and that they have an important role in the occurrence of wear, such as the abrasives included in the chemical formulations of pastes (30).
The fact that the toothpastes used in the other studies contain similar abrasives and create different surface roughness and colouration values may be due to the difference in abrasives, as well as the fact that other active substances such as detergents play a role in these parameters (29,31).
Within the limitations, the whitening toothpastes used in this study caused an increase in roughness on the surface of the restorative materials. It is thought that the most important factor affecting the roughness differences on the surface is related to the structure of the restorative materials, as in the result of Roselino et al's study (9). It is another result of the study that the increase in surface roughness and changes in colouration can progress parallel to each other. Generally, OCM containing silica caused less roughness increase than the groups containing hydrated silica. For this reason, it may be recommended to use silicacontaining toothpastes in order to eliminate the negative effects of roughness in people where the restorative materials used in this study are widely used in the mouth. In terms of colour change, the use of COW on giomer and microhybrid materials and the use of SWN on nanohybrid composite were found to be more effective, but this was not statistically significant compared to other toothpastes in the same main group. The effects of brushing for 1 year or longer with toothpastes containing these active ingredients on the restorative materials and tissues in the mouth should be evaluated separately with other in vitro and in vivo studies using different study designs and different materials.
Conclusions
Within the limitations of this in vitro study, it can be concluded that the giomer composite group was most prone to coloration, while the nanohybrid composite group was more resistant to coloration. Surface roughness of microhybrid and nanohybrid groups increased at a similar rate. Although the group with the highest initial surface roughness was the giomer composite, it was the group in which the roughness changes occurred the least. The toothpastes used in the study were not superior to each other in removing discolouration.
Author contribution statement
Conceptualization and design: B.D. and F.Ö.
Literature review: F.Ö.
Methodology and validation: B.D. and F.Ö.
Formal analysis: B.D.
Investigation and data collection: F.Ö.
Resources: B.D.
Data analysis and interpretation: B.D. and F.Ö.
Writing-original draft preparation: B.D. and F.Ö.
Writing-review & editing: B.D. and F.Ö.
Supervision: B.D.
Project administration: B.D.
Funding acquisition: B.D.