INTRODUCTION
Vitiligo is a depigmenting disorder of the skin which is characterized by selective loss of melanocytes and leads to pigment dilution in affected skin areas. The vitiligo lesion is a totally amelanotic, non-scaly chalky white macule with distinct margin. Now it has been classified as an autoimmune disease, associated with genetic, environmental factors, metabolic disorders and cell detachment abnormalities (1). 50% of the patients have childhood onset of the disease and the prevalence of vitiligo is 1-2% worldwide. Female predominance is seen in pediatric vitiligo as seen in adult vitiligo. The vitiligo lesions in pediatric patients are distributed as generalized disease-34% followed by acrofacial-13%, mucosal-3%, segmental -29%, and undetermined -21%. The psychological problems such as depression, lower self-esteem, anxiety and poor quality of life are seen in childhood vitiligo. The autoimmune diseases such as thyroiditis, pernicious anemia, atopic dermatitis, diabetes mellitus and alopecia areata are associated with vitiligo (2). 25% of vitiligo in children are diagnosed before 10 years of age. The age of onset of vitiligo in children ranges between 4 to 8 years (3). So far, vitiligo is the most frequent disorder of pigmentation. Prevalence of vitiligo in India is 8.8% which is highest in the world and in U.S.A. it is about 1%. In addition, in world about 1% of the population has vitiligo according to the literature (4). In the literatura only very few cases of oral vitiligo have been reported. Vitiligo of the oral mucosa is rare. Lip is most commonly affected followed by palate and gingiva. Immunomodulators, micropigmentation, phototherapy, and invasive surgical treatment are the various treatment modalities followed in treating the disease. In the oral region, the response to the treatment is very minimal and hence the early diagnosis helps in treatment success and also reduces the aesthetic damage.
CASE REPORT
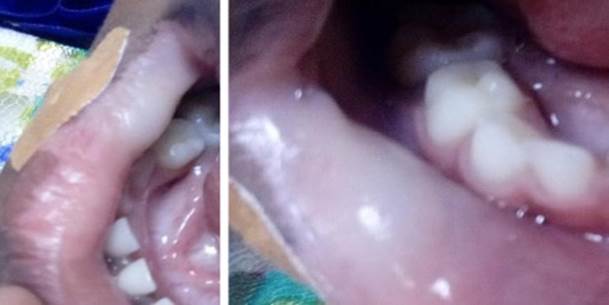
A 9 year old patient reported to the department of oral pathology with the chief complaint of a whitish patch on her lips for the past two year. The lesion was asymptomatic. Initially the lesion was a small dot and gradually increased to the present size. The patient was healthy and was not taking any medication. There was no familial history of the present disease and nor a history of trauma on the affected site. The patient’s parents were concerned about the color change in the child’s lip and reported to the hospital to find the underlying cause.
Extra orally, there was no abnormality detected and there was no lesions elsewhere in the body. Intra orally, in vermilion border of the lip, there was a diffuse patch of size 2.5×3.5cm involving the labial mucosa. Laboratory examinations were ordered for complete blood count, hemoglobin, TSH, anti-thyroglobulin and anti-thyroperoxidase antibodies. No abnormalities were present in the results. The thyroid examination was done to rule out the autoimmune disorder associated with vitiligo.
Based on the clinical examination and clinical presentation, the final diagnosis was made as vitiligo. The vitiligo in this patient was an unclassified type since the patient presented the lesion only in the vermilion border of the lower lip involving the labial mucosa without any other lesion in other areas of the body. The patient was referred to the dermatologist for further treatment.
DISCUSSION
Vitiligo is the most frequently occurring depigmentation disorder, affecting approximately 0.5-1% of individuals. There is no gender prevalence. Vitiligo is an asymptomatic disease. However, associated symptoms have been demonstrated in some cases, including pruritus and burning sensation of the skin. The symptoms can also be due to psychological distress (5). Vitiligo affects the skin most commonly, which includes neck, face, and scalp. Mucosal involvement of lips, genitals, gingiva and nipples are reported. In oral tissues, vitiligo is very rare. In a systematic review of vitiligo in childhood, autoimmune thyroid disease was found in 14.3% of patients with vitiligo and it was most commonly seen in female gender, since they report more than the male. The melanocyte dysfunction and disappearance are due to environmental cause, genetic liability, metabolic deformity, impaired renewal, and altered inflammatory and immune respons (7).
Diagnosis is mainly based on clinical features. The Wood’s lamp, a hand held ultraviolet irradiation device emitting UVA can be used in the diagnosis of vitiligo. The Wood’s lamp detect the areas of depigmentation that is not visible to the naked eye. The vitiligo lesions emit a bright blue-white fluorescence under the Wood’s light. The evaluation of the presence of organ-specific autoantibodies, especially those directed against thyroid and adrenal glands could be useful to find out whether the disease is associated with an autoimmune disorder (1,11-12).
The vitiligo is classified into segmental and non-segmental vitiligo, non-segmental vitiligo is divided into generalized, acrofacial, universal, mucosal and mixed vitiligo. In Mucosal vitiligo, oral and genital mucosa are involved. Mucosal vitiligo is included in the non-segmental vitiligo, when there is a skin involvement. If skin lesions are not present, mucosal vitiligo is classified as undetermined or unclassified vitiligo (5,6,7).
The Vitiligo subcommittee of the European Dermatology Forum has given certain guidelines for the management of the vitiligo. The guidelines of the vitiligo management includes, first-line to fourth-line options. The first line of treatment option includes topical treatment that is topical application of corticosteroids and calcineurin inhibitors. The second line of treatment option includes phototherapy (NB-UVA) and psoralen and UVA (PUVA) and systemic steroid treatment. Third line treatment option includes surgical grafting. The fourth line of treatment includes depigmentation. Afamelanotide, the analog of α-melanocyte-stimulating hormone which is synergistic with NB-UVB has shown promising results in promoting re-pigmentation (1,6,7,9). The vitiligo in the oral mucosal region is more resistant to treatment as there is no melanocyte reservoir in those areas because of no hair follicles. The topical tacrolimus is effective in early vitiligo (8,13).
CONCLUSION
Even though the vitiligo lesions are rare in oral mucosa, when the initial lesions of vitiligo are seen during dental screening, it is very important that the patients are informed and the treatment is started as early as possible since the early intervention shows promising results in treating the lesions of vitiligo. And the dentist along with the dermatologists should identify the most suitable treatment for the patient depending up on the clinical form and extent of the lesions.
Patient consent: Consent for the publication was obtained from the patient’s parents.