Introduction
The elbow joint is the second most commonly dislocated joint in adults after dislocation of the shoulder joint. The annual incidence of simple and complex elbow dislocations is 6.1 per 100,0001. Elbow dislocations are classified as simple or complex types2. The simple dislocation is characterised by the absence of fractures, while the complex dislocation is associated with intra-articular fractures of the radial head and coronoid process. This injury frequently occurs during sporting activities when a person falls on an extended elbow. Elbow dislocation is usually posterior and the semilunar notch of the ulna is dislocated posteriorly from the distal humerus. The elbow joint is a stable joint and a significant force is required to disrupt the joint. Neurovascular complications are rare. The less encountered anterior elbow dislocation requires much more force. A dislocated elbow requires immediate closed reduction to prevent complications.
Case report
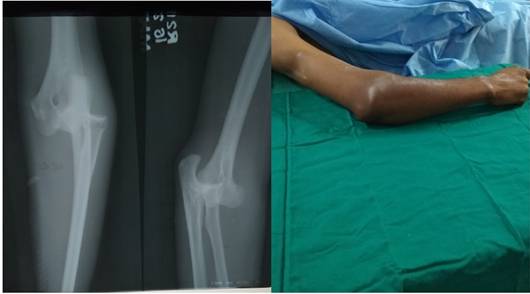
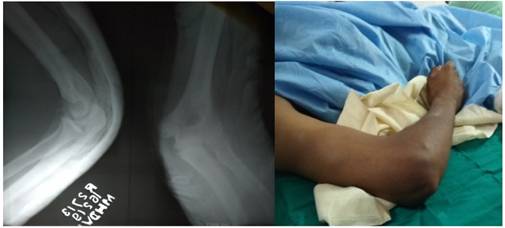
A 29 years old male sustained a fall on outstretched hand from two wheeler and presented to the department of General Surgery at a peripheral hospital in Nasik, Maharashtra, India with pain, swelling , deformity and inability to move his Right elbow. Imaging in the form of X Ray Right elbow revealed a dislocated elbow. Closed Reduction was done under General Anaesthesia and Congruity of the bones forming the elbow joint was achieved which was confirmed on check X Ray Right elbow. He was offered immobilisation of the elbow joint in the form of above elbow Posterior slab for 3 weeks followed by active and passive elbow movements to achieve full range of movements at the elbow joint. He was advised to consult an Orthopaedician after discharge from the hospital.
Discussion
The elbow represents one of the most stable joints in the human body. Despite its name, simple elbow dislocation is a complex injury of the capsule-ligamentous structures. Typically, simple elbow dislocations occur when a person falls onto an outstretched hand. Complex dislocation is associated with intra-articular fractures of the radial head and coronoid process. Elbow dislocations are classified by the direction of their displacement. Most of the elbow dislocations are posterior dislocations and anterior elbow dislocations are rare.
In 58% of patients, the simple elbow dislocations were on the non-dominant side3. Following reposition and treatment in plaster of simple dislocations, recurrent dislocations and chronic instability are not or only rarely seen 2.
Etiology: A posterior elbow dislocation often occurs when a person falls on an outstretched hand. Anterior elbow dislocations occur when the elbow is flexed, and there is a direct blow on the posterior aspect of the elbow.
Epidemiology: Elbow dislocation is the most common joint dislocation in paediatric patients and the second most common in adult patients. The injury more often occurs in adolescent male athletes. Footballers and wrestlers are prone to this injury. Posterior elbow dislocations comprise 90% of all elbow dislocations 4.
Anatomy: The elbow joint is a highly congruent articulation that confers substantial bony stability5. The coronoid process enhances stability particularly in flexion and the contact area of the radio-capitellar joint increases with flexion6.The medial collateral ligament and the lateral collateral ligament complex (including the lateral ulna collateral ligament (LUCL)) are the primary stabilisers. These are complemented by the secondary stabilisers; the radial head, the joint capsule and the common flexor and extensor origins. This is also augmented by dynamic stability provided by the muscles crossing the elbow joint.
Pathophysiology: The brachial artery and ulnar and median nerves are particularly susceptible to injury because the anterior compartment is often disrupted during posterior dislocation. The ulnar nerve may become entrapped as it passes posteriorly around the medial epicondyle. Anterior dislocations are often associated with olecranon fractures and may also disrupt the posterior elbow compartment which contains the radial nerve.
History: History includes the details of mechanism of injury. The patient should be asked if there have been previous elbow injuries in the past. The patient should be asked about the symptoms suggesting a neurovascular compromise and inquire about numbness, tingling or coolness of the distal extremity.
Local Examination: The elbow joint should be inspected for swelling, deformity or bruising. Posterior elbow dislocations often present with an upper extremity that is flexed and appears shortened. Anterior elbow dislocations are held in extension, and the upper extremity appears elongated. Open wounds would suggest a complex dislocation. The functionality of the elbow joint should be assessed by observing a range of movements.
Neuro-vascular damage: The most common neurovascular structures injured during an elbow dislocation include the brachial artery , ulnar nerve and median nerve. Radial and ulnar pulses should be palpated . Median nerve sensation can be assessed by a light touch of the palmar aspect of the thumb and index finger. Median motor function is tested by observing the strength of thumb opposition. A light touch on the palmar aspect of the ring and little fingers can assess ulnar sensation. The ulnar motor function is tested by observing the strength of finger abduction and adduction.
Imaging: Plain Radiographs of elbow joint taking anterior-posterior , lateral and oblique views help evaluate joint congruency and associated fractures. Computerized tomography may be considered to identify periarticular fractures not easily seen on plain radiographs.
Treatment: Initial treatment of simple, closed posterior elbow dislocations is closed reduction. Complex elbow dislocations require open reduction and internal fixation. Open dislocations require extensive washout during an open reduction. Any dislocation with signs of neurovascular compromise requires immediate closed reduction7.
There are two common approaches to the reduction of a posterior elbow dislocation. The first technique is attempted with the patient lying down in the prone position. The affected arm is abducted with an elbow on the edge of the cart. The wrist is then grasped and the forearm placed in slight supination while gentle traction is applied. The coronoid process must be distracted and disengaged from the olecranon fossa. Once this has been accomplished downward pressure with the other hand on the olecranon should reduce the dislocation with the operator feeling a confirmatory clunk. A two-person technique is also described where one operator applies downward traction at the wrist, and other applies the downward force onto the olecranon with both their thumbs.
The alternative method is performed with the patient seated or lying supine on the cart. An assistant stabilizes the affected humerus while the operator flexes the elbow, supinates the wrist slightly and applies distal and downward traction at the wrist with one hand. The other hand is placed just distal to the elbow on the volar aspect of the forearm applying slow, gentle inline traction until the confirmatory clunk is appreciated.
Following reduction, a neurovascular examination should be performed to identify improvement in any previous neurovascular symptom or a new symptom that may have manifested following the reduction. The elbow should be held in 90 degrees of flexion for about 3 weeks of splinting and a specific range of motion plan thereafter.
After reduction of the elbow joint, targeted clinical examination should be performed in order to ascertain and record the severity of the injury and assess whether an MRI is needed for further diagnosis.
Conclusion
Simple elbow dislocations are a commonly seen injury within orthopaedic practice and expedient closed reduction and early active mobilisation usually results in excellent or good long-term functional outcomes. Elbow dislocation is usually posterior. Neurovascular complications are rare. A dislocated elbow requires immediate closed reduction to prevent complications.MRI can identify those that may require surgical intervention.