Malaria research remains as one of the priorities for the improvement of public health around the world. World Health Organization (WHO) reported in 2016 around 198 million cases worldwide and 4.3 million deaths, even though the increased in prevention measures had accomplished the reduction of the mortality in a 58 % in in children under 5 years. The population living in the sub-African region is the most affected by this disease accounting for 90 % of the cases reported. Malaria cases worldwide seem to increase with time due to the raising transmission risk in endemic areas, where sanitary control is deficient allowing expansion through the diverse media transport available in the modern day (Winter et al., 2008; WHO, 2016).
Malaria is cause by protozoa parasites of the genus Plasmodium; and Plasmodium berghei is a murine strain which causes malaria in rodents (Jambou, El-Assaad, Combes, & Grau, 2011; Knell, 1991). Rodent Plasmodium berghei ANKA model validity has been previously reported for human cerebral malaria, primarily due to the ease of handling and maintaining rats and mice in the laboratory. Also large-scale sequencing projects have generated a substantial information allowing the genetic comparison between P. falciparum and P. berghei where many protein motifs and signatures were identified as being conserved between the species (Carlton, Silva, & Hall, 2013). It is always important to consider the right combination of the experimental animal host and the malaria parasite able to mimic the patterns seen in the human pathologies, as it is impossible to obtain a detailed examination of the multiple disease’s processes in clinical trials, especially at an early stage of the drug evaluation (Craig et al., 2012). To study the curative effect of the compounds this rodent model was chosen as a good malarial experimental model.
Antimalarial drugs can be classified according to their action on particular stages of the life-cycle of the parasite. The categories are: Causal prophylactic drugs (act on the pre-erythrocytic forms); Gametocytocidal drugs (act on gametocytes); Sporontocidal drugs (inhibit the sporogonic phase of development of the parasite in the mosquito) and last Schizontocidal drugs (act on the asexual erythrocytic forms of all species of malaria parasites). Chloroquine (ClQ) is a Schizontocidal drug, which has a strong and rapid for the treatment and prevention of clinical symptoms (Bruce-Chwatt, 1962).
Recently there are various difficulties regarding the developing of new antimalarial drugs, like cost, toxicity and drug resistance; nonetheless it has been considered globally the importance of finding new ways to improve antimalarial treatments (Hsu , 2006). Between 1975 and 1999 around 1 400 new antimalarial drugs were registered worldwide, although only a few of them were considered as “adequate drugs” for the efficient control of malaria (Wongsrichanalai & Meshnick, 2008). Chloroquine being one of them, has been used for more than 50 years as malaria treatment, which made its resistance appeared in a slow and a progressive manner (Abdi, Gustafsson, Ericsson, & Hellgren, 1995; Cooper & Magwereb, 2007). When treatment with an antimalarial drug has been administered but still results in an incomplete clearance of parasites from the patient’s blood is called drug resistance. Resistance has emerged to almost all antimalarial drugs except the artemisinins causing an increase in malariarelated mortality (White, 2004).
The compounds derived from the chalcone nucleus, which incorporate electron-donating substituents in benzene rings, have interesting biological activity as antioxidants, anticancer, antifungal and antituberculosis (Liu, Wilairat, Croft, Tan, & Go, 2003; Satyanarayana, Tiwari, Tripathi, Srivastava, & Pratap, 2004). In particular, the 3- (4-methoxy-phenyl) -1- (4-pyrrol1-yl-phenyl) prop-2-en-1-one compound has activity against Plasmodium falciparum (Ono et al., 2007; Reddy et al., 2008).
The experimental compounds have been previously characterized as photosensitizer, which are light-sensitive molecules. Photo-toxicity induced by drug administration is triggered by sunlight exposure and occurs as the result of an hydrogen or electron transfer; a process which leads to the formation of free radicals capable of reacting directly with biomolecules in the environment or with molecular oxygen to form various Reactive Oxygen Species (ROS) (Baptista & Wainwright, 2011; Seto et al., 2011). The ROS output through photosensitizer mechanism involve the transference of energy through chromophores to oxygen molecules. Previous studies have reported evidence of the mechanism of action of ROS which triggered different physiological and pathological responses in the organisms (Lavi, Shainberg, Shneyvays, Hochauser, & Isaac, 2010). In this study we evaluated the antimalarial effect of two photo-excitable compounds in a murine model in vivo, assessed their cytotoxicity in vitro and observed the incorporation of the compounds though Indirect Immunofluorescence Assay (IFA). This compounds were evaluated as antimarial drugs, because in previous assays they presented hemolysis effect on red blood cell (RBC).
Materials and methods
Malaria Parasite: Plasmodium berghei ANKA strain was used as experimental mice model. The adults female BALB/c mice (Mus musculus) from 10 weeks of age and 22 g of weight were inoculated with 200 µl cryopreserved blood with parasitized red blood cells (RBCs) stored with 20 % glycerol at -80 °C. After, the parasite challenges were administered by intravenous injection of five thousand PRBCs.
Isolation of parasitized RBCs: Three adult female BALB /c mice with 10 weeks of age and 22 g of weight were infected with 5x103 parasitized red blood cells (RBCs) of Plasmodium berghei ANKA strain intraperitonially (IP). When parasitemia reached 40 %, parasitized RBCs were isolated by a cellulose column (CF-11 (Sigma), using NaCl 0.85 % solution). The trophozoites and schizonts were isolated by a discontinuous Percoll column (60, 70 and 80 % gradient in ascendant form) previously described by Spencer, Quintana, and Hidalgo (2008).
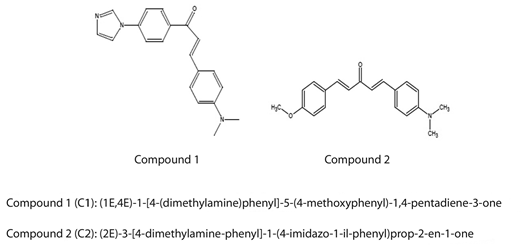
Incorporation of experimental compounds in fundamental state and photoproducts in Short-term in vitro cultures of P. berghei: The Compound 1: (2E)-3-(4-dimethylamino-phenyl)-1-(4-imidazol-1-yl-phenyl) prop-2-en-1-one) (C1), which has been reported its anti-malarica activity in its fundamental state (Zhang, Guo, Lin, & Benet, 1999); and Compound 2:(1E,4E)-1-[4-(dimethylamino) phenyl]-5-(4-methoxyphenyl)-1,4-pentadiene3-one) (C2). The compounds derived from Curcumin, in a more stable monocarbonic structural version, are identified with substituted dibenzylidene ketone structures, which are associated with the structure of compound C2 (Das et al., 2007). These compounds were donated by Prof. Nieves Canudas from Photochemistry and Photobiology Laboratory at Universidad Simon Bolivar, Venezuela and they were prepared by Claisen-Schmidt condensation under basic condition in the Organic Synthesis Laboratory at Universidad Simón Bolívar (USB) (Ono et al., 2007). The compounds were solubilized previously in PBS with 10 % Dimethyl sulfoxide (DMSO). Then, 5 x 106 /150 µl of parasitized RBCs and 5x105 /5 µl healthy RBCs were added to culture plates containing MEM (Minimum Essential Media Eagle, Sigma) supplemented with Bovine Fetal Serum (BFS) 10 %; non-essential amino acids 1 %; glutamine 1 % and penicillin/streptomycin 1 %. Later one experimental compound was added per culture plate (Chloroquine, Compound 1 or Compound 2) at 100 µg/µl. Culture plates were incubated for 1 hr at 37 °C (5 % CO2). Later culture samples were taken at 15, 30 and 60 min, and acetone-fixed onto IFA commercial slides to be stored at -20 °C until further use (Spencer et al., 2008). In order to the irradiation experiment, the same procedure was followed. However, before the incubation, the plates were irradiated in a Solar Simulator (Luzchem Research, Inc) at 1 500 Foot-Candles (FC) for 5 minutes. Fluorescence images were observed by fluorescence microscopy. Excitation wavelengths were selected at 490 nm to FITC and 372 nm to DAPI.
Absorption and Fluorescente measurements: All the solvents (spectroscopic grade) were used without purification, and none on them showed absorption or residual fluorescence at the wavelengths of interest. The solutions (1x10-6 M) were deoxygenated by N2 bubbling. UV-vis absorption spectra were recorded on a Cary 50 UV-Vis spectrophotometer. Steady-state fluorescence emission and excitation spectra were measured using a Varian Cary Eclipse Spectrofluorimeter. The fluorescence spectra were corrected for the wavelength response of the system. Fluorescence quantum yields were obtained using fluorescein and Rhodamine B as standards (Williams, Winfield, & Miller, 1983).
Production of Antibodies: Polyclonal antibodies against C1, C2 and ClQ were generated by immunizing of three groups of adult female BALB/c mice from 10 weeks of age and 22 g of weight with 200 µl cryopreserved blood with parasitized red blood cells (RBCs) (stored with 20 % glycerol at -80 °C), were used in groups of 5 animals. When parasitemia reached 40 %, blood was collected without anticoagulant and the sera obtained was stored at -20 °C until further use (Spencer-Valero et al., 1998; Moll et al., 2003).
Indirect Immunofluorescence Assay (IFA): The IFA was carried out at room temperature in a moist chamber. Schizont of P. berghei were acetone-fixed preparations were incubated for 1 hr at 37 °C (5 % CO2) with primary antibody (serum from immunized mice diluted in PBS 1:100), the negative control was incubated with serum from unimmunized mice and PBS. After incubation, slides were washed in PBS. Later, the preparations were incubated for 1 hr in fluorescein isothiocyanate (FITC)-conjugated anti-mouse immunoglobulin G (IgG) (Sigma) (diluted in PBS 1:1000), and washed again in PBS. After addition of mounting medium (Santa Cruz Biotechnology, Santa Cruz®), the preparations were examined with a fluorescence microscope (600X) (Harlow & Lane, 1988). In some cases, the preparations were treated further with 25 µg/ml 4’,6-diamidino- 2-phenylindole hydrochloride (DAPI) (Sigma) in PBS for 5 min to visualize both immunofluorescence and DAPI-stained parasite nuclei. The immunofluorescence samples were posteriorly analyzed with OptikaView7 software.
Drug treatment study with experimental compounds in fundamental / no irradiation and irradiation: A group of 12 female BALB /c mice (22 g of weight) was IP inoculated with 5x103 P. berghei parasitized-erythrocytes. The drugs (20 mg/kg Chloroquine, 20 mg/kg Compound 1 and 20 mg/kg Compound 2 in fundamental state for a 20 g of mouse weight) were orally administered 72 hours post-inoculation during 4 days, using a metylcellulose (1 %) and Tween 80 (0.5 %) as vehicle. For treatments with compounds with irradiation, mice were submitted each day after drug administration, to a 1 500 FC irradiation in a Solar Simulator (Luzchem Research, Inc) for 5 min. The dorsal area of mice was shaved 24 h previous the first day of drug administration for better exposure of the blood vessels. Parasitemia was monitored daily smears made from tail blood fixed with absolute methanol and Giemsa’s reagent. Finally the smears were examined by light microscopy (100X). All animal experimentation was approved by the Ethical Review board of USB.
Cell Proliferation Assay: A colorimetric method for determining the cytotoxicity of (2E)-3-(4-dimethylamino-phenyl)-1-(4-imidazol-1-yl-phenyl) prop-2-en-1-one) and (1E, 4E)-1-[4-(dimethylamino) phenyl]-5-(4methoxyphenyl)-1, 4-pentadiene-3-one) using Chloroquine as positive control. 105 VERO cells were obtained from culture plates by trypsinization process described previously by Abrahamsen and Lorens (2013) and the added to a 96-well culture plate with supplemented MEM (Minimum Essential Medium Eagle,
Sigma) and different concentration (0.5, 1, 5, 10 and 20 µg/ml) of experimental compounds C1, C2 and ClQ. The plate was incubated at 37 °C for 72 hours in a humidified, 5 % CO2 atmosphere. After incubation, MTS was added to the culture wells and the absorbance at 490 nm was measure at different times (0, 1, 2 h) using a 96-well plate reader (CellTiter 96® Aqueous, Promega, U.S.A, 2013). The cell proliferation assay with the compounds with irritation followed the same procedure. Before the 72 h incubation; the culture plate (with only the compounds) was irradiated in a Solar Simulator (Luzchem Research, Inc) at 1500 FC for 5 min. After the irradiation de medium was added followed by the VERO cells and the reduction in absorbance at 490 nm for the treated and untreated control cultures was measured and compared.
Results
Two compounds (C1 and C2) were evaluated as anti-malarial drugs and compared to ClQ. These compounds were irradiated to photo-excite them for 5 minutes in a solar simulator as explained in the materials and methods section. For IFA, cytotoxicity and cure assays with P. berghei in BALB/c mice. In addition, these are 99 % pure in their synthesis and are fluorescent in lipophilic medium and photo-hemolytic on human erythrocytes. Other authors have reported the biological activity as anti-plasmodium of these compounds in fundamental state on cultures of P. falciparum (Aher et al., 2011).
The antimalarial drugs used for this study were (2E)-3-(4-dimethylamino-phenyl)-1-(4imidazol-1-yl-phenyl) prop-2-en-1-one) (C1) and (1E,4E)-1-[4-(dimethylamino) phenyl]5-(4-methoxyphenyl)-1,4-pentadiene-3-one) (C2). The Chloroquine (ClQ) as a posited control of cure assays (Fig. 1).
In the Figure 2, we showed the immune fluoresce patron at 30 minutes to C1, C2 and ClQ. In the panel 2A and 2B. In all the treatments can see the compounds inside the PRBCs and this was indicated with the arrows.
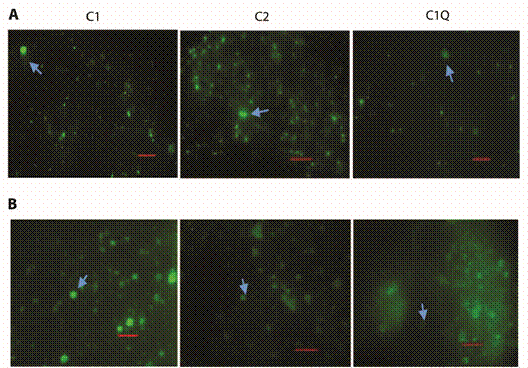
Fig. 2 Indirect immunofluorescence assay (IFA) staining of P. berghei within red blood cells (RBC) with different treatments (C1) Compound 1 (C2) Compound 2 and (ClQ) Chloroquine, A) Compounds without irradiation and B) after irradiation of 1500 FC at 30 min of incubation time. The thin films were fixed with acetone, later to be Giemsa stained and examined by fluorescence microscopy at 600 magnification. The arrows indicate the parasitized RBC with a typical fluorescence pattern of the PRBC, the yellow arrows indicate the compound inside the PRBC and the white arrows indicate the free compound, outside the PRB. The bar on the bottom right of each image represents the scale of 10 μm.
In order to know if the fluorescent pattern was not an artifact, we performed a DAPI stain to see the nuclei of parasites into the PRBC (Fig. 3). In Figure 3 could observed that each compounds had interaction with PRBC and however the intensity of fluorescence pattern was increased in the region of the cell membrane of the parasitized erythrocyte. This effect was observed to C1, C2 and ClQ compounds, and the fluoresce pattern were every similar to 15, 30 and 60 minutes (data not shown to 15 and 30 minutes).

Fig. 3 DAPI staining in the immunofluorescence assay performed with P.berghei short cultures with different treatments C1, C and ClQ in the ground state at 60 minutes incubation after irradiation with 1500 FC at 30 min of incubation time. The PRBC were fixed with acetone and observed through an epi-fluorescent microscope with 400 magnification. The different stains are shown, DAPI (blue color) using the UV filter; and FITC (green color) using the blue light filter. Binding of both fluorescence patterns is shown in the third column (overlapping). Red arrows indicate GRPs with a typical (spherical) marking pattern.
In Figure 4, we showed the cytotoxic effect of the compounds evaluated in cell cultures with VERO cells and determined by a colorimetric method from Promega, as explained above in the materials and methods section. The results were presented in histogram graphs and the bars represent the standard error for the two types of treatments, the compounds were irradiated and non-irradiated in the cell cultures before the incubation with 1 500 FC. Each experiment was performed in triplicated.
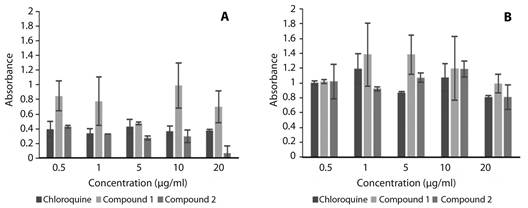
Fig. 4 Compounds cytotoxicity determination using a proliferation assay with VERO cells (MTS, Promega). (A) Assay with compounds no irradiation in fundamental state (B) Assay with compounds irradiation for 5 minutes. After 1 hour at 37 °C in a humidified, 5 % CO2 atmosphere; the absorbance at 490nm was measure using an ELISA plate reader. The bars represent the D.O obtained for the compounds in five different concentrations of 0.5, 1, 5, 10 and 20 μg/ml.
In figure 4A, the results of the cytotoxicity of the non-irradiated compounds in their fundamental state can be observed. In this treatment the most toxic compound was Chloroquine and C2 at the concentration of 20 μg/ml with an absorbance of 0.8 D.O. But, between the two experimental compounds was C2 is more cytotoxic in general, and especially at 5 μg/ml with an absorbance of 0,9 D.O.
On the other hand, when the compounds were irradiated in general their cytotoxicity increased considerably up to more than three times that in their fundamental state. The compound C2 was the most cytotoxic in this condition followed by chloroquine (Fig. 3B).
When the compounds were irradiated they can be decomposed into photo-products and these products were more cytotoxic than in their fundamental state without irradiation. Even more, they can increasing their toxicity up to eight times more and this case was to C2 at 20 µg/ml (Fig. 4B).
In the curing trials with the BALB / c mouse model with P. berghei. In Figure 5 showed the parasitemias of mice with the compounds presented in vivo experiments, when they were administrated orally for three days post infection as explained above in the methods section. The results were showed in figure 5, demonstrated that any the compounds 1 or 2 had anti-malarial activity compared to chloroquine as positive control of cure in their fundamental state. The compounds C1 and C2 presented a behavior in their parasitemias similar to the negative control without drug, dying all the mice around day 21. While, ClQ was able to control the parasitic infection and all mice survived to the infection by Plasmodium berghei.
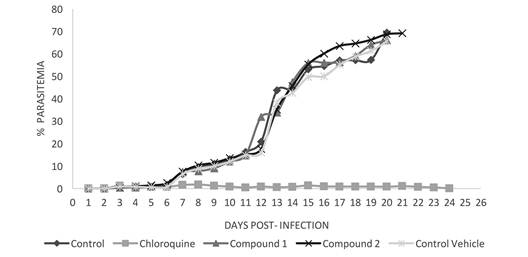
Fig. 5 Parasitemia-Time profile using BALB/c mice following the administration of a 4 dose regimen of 20 mg/kg Chloroquine (n = 3), Compound 1(n = 3), and Compound 2 (n = 3), in fundamental state; administered 72 hours after IP inoculation with 105 P. berghei parasitized-erythrocytes. Data are shown as total parasitemia (mean percentage of infected erythrocytes/total erythrocytes ± SD), starting from the time of drug administration. Parasitemia was monitored daily by smears fixed with absolute methanol and Giemsa stained.
However, the distribution of parasitemias changed when the compounds were irradiated and were used as anti-malarial drugs after irradiation. In these condition the C1 did not present curative effect, but C2 changed its percentage of parasitemia significantly with respect to fundamental state. A curative effect was observed, since the parasitemia diminished almost three times in relation to the negative control. Although, the mice died with a parasitemias of 25 %, in day 17 post infection and percentage of survive of mice was 33 % higher that C1 (data not shown). This suggests a high toxicity effect to the photo-product of C2 with respect C1 compound.
Therefore, the antimalarial effect from C2 was not equal to or higher than ClQ, being this last the best antimalarial in the cure trials and controlling the parasitemia from the beginning of the infection.
Discussion
Two compounds (C1 and C2) and Chloroquine were tested for several in biological assays. They were incorporated as drugs in short-term cultures of P. berghei and were assessed by an indirect immunofluorescence assay (IFA), cytotoxicity assays and evaluation of anti-malarial drugs in rodent model with P. berghei. All of compounds were treated in their fundamental state and they also were evaluated as photosensitizers under radiation 290-800 nm (solar spectrum). Then we analyzed our results in this section.
In the figure 2, we demonstrated by IFA with samples at 30 min of incubation of compounds on culture with P. berghei the incorporation of compounds at PRBC the indirect immunofluorescence assays showed a typical image of fluorescence pattern with all the compounds; this phenomenon could be caused by the accumulation of drugs into de cell biology membranes of schizonts. Because the lipophilicity associated to the chemical structure of C1 and C2, these can be located into the plasmatic membrane of PRBC.
The C1 y C2 compounds were prepared as was indicated in material and methods section. The molar extinction coefficient to C1 in dichloromethane as lipophilic environment was ε 31 717, absorption lab 425 nm, emission lem 530 nm, relative quantum fluorescence yield Ff 0,48. To C2 the molar extinction coefficient in dichloromethane as lipophilic environment was ε 26 084, absorption lab 425 nm, emission lem 557 nm, relative quantum fluorescence yield Ff 0,21. In protic polar medium no fluorescence was observed for either compound. The detection of fluorescence in the experiments with the use of FITC (fluorescein-5-isothiocyanate, lab 490 nm, lem 520 nm) together with C1 or C2 in the cellular system, it does not allow to affirm that the detected fluorescence comes exclusively from the FITC emission from conjugate, since both C1 and C2 absorb between 390-500 nm, reaching the excitation point used for FITC. The increased intensity in the images showing FITC (Fig. 3) could be associated with the presence of C1 and C2 in the membrane. In consequence, the higher fluorescence intensity obtained for PRBC in presence of compound C1 in photo-excitable state in comparison with compound 2 and Chloroquine (Fig. 3B) could be the result of the additive effect of the intrinsic fluorescence of compound 1 (bright yellow) incorporated in the PRBC and the secondary antibody label with fluorescein (green).
According to the results of cellular cytotoxicity with the compounds evaluated under radiation conditions for five minutes, they may have a photosensitizing effects on the biological system by the generation of ROS and/or the formation of toxic photoproducts (Fig. 4A and Fig. 4B). In the figure 4A, we represented the results of cellular cytotoxicity of the three compounds in their ground state, where compounds C2 and CLQ at 5 and 20 μg / mg showed the highest cytotoxicity with a value of 0.8 D.O. In contrast, after irradiation the most cytotoxic compound was C1 to 20 μg / ml presented a cytotoxicity around 8 times greater than in its ground state with a value of 0.1 D.O. (Fig. 4B).
In vivo evaluation of the compounds showed no antimalarial effect from both, compound 1 and compound 2 in fundamental state. Parasitemia-Time profiles were similar to control groups and resulted on the death of all experimental animals with a mean survival time of 20 days (Fig. 6). Early death only eight days post-infection was found on both experimental groups and was attributed to cytotoxicity of the compounds in fundamental state, corroborated by the proliferation assay results (Fig. 4A).
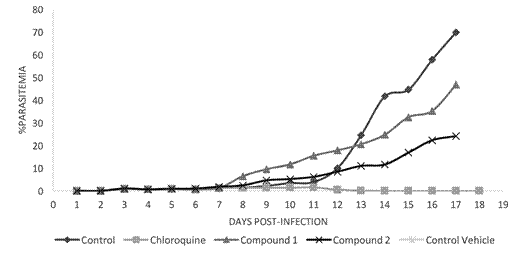
Fig. 6 Parasitemia-Time profile using BALB/c mice following the administration of a 4 dose regimen of 20 mg/kg Chloroquine (n = 3), Compound 1 (n = 3), and Compound 2 (n = 3), in photo-excitable state; administered 72 hours after IP inoculation with 105 P. berghei parasitized-erythrocytes. Each day after drug administration, mice were submitted to a 1500 FC irradiation in a Solar Simulator (Luzchem Research, Inc) for 5 min. Data are shown as total parasitemia (mean percentage of infected erythrocytes/ total erythrocytes ± SD), starting from the time of drug administration. Parasitemia was monitored daily by smears fixed with absolute methanol and Giemsa stained.
In order to evaluate the anti-malarial effect for the better take of The UV-vis radiation penetrated the skin and interacted with the erythrocytes inside the capillary in the shaved dorsal area of mice submitted to irradiation. Under irradiation conditions C1 and C2 lowered the parasitemia in comparison with the control group but were unable to cure the experimental animals like Chloroquine (Fig. 6). Nonetheless, 1/3 of the sample treated with compound 2 survived, and was “cured”. More tests need to be done due to the increase toxicity of this compound and low efficiency. Early death were also found after a week for both experimental compounds under irradiation conditions. This could be consequence of the environmental stress caused by the irradiation into the Solar Simulator chamber, but also the increased cytotoxicity of both compounds in comparison with their fundamental state obtained in the proliferation assay. These results suggest that compounds act as photosensitizers maybe inducing photo-hemolysis by cell membranes damage and therefore causing a progressive and lethal anemia to the experimental animals. The need for further trials arise to elucidate the phototoxic effect in vitro, allowing the reduction of experimental animal’s deaths and enhancement of the results of in vivo assays.
Sanz and colleagues (2012) determined that drugs that inhibit identical molecular targets or cellular functions, show similar parasitic mortality rates, meaning the parasitic mortality rate of every drug could indicate its mechanism of action. This suggest the compounds evaluated were not presented the same mechanism that Chloroquine, and in addition their structures are different to Chloroquine, therefore they do not have the same efficiency as antimalarial drug. Also, is necessary to point out that even though Chloroquine and compound 2 showed a similar in vitro cytotoxicity, the results obtained for in vivo assays were contradictory, expressing the importance of in vivo evaluation on the research of new antimalarial drugs.
This study suggests that this class of research should be followed developing this strategy, since this infection is typical of tropical countries, where the incidence of sunlight is throughout during all year and it would be an advantage to develop compounds that generate photoproducts that could act effectively as drugs Antimalarial drugs.
Conclusion
Chloroquine and the compounds used in this study have been reported as anti-malarial effect on the parasites. The antimalarial activity of compounds C1 and C2 in the ground state and under irradiation conditions suggests a photosensitizing effect observed in a reduction of the parasitemia in experimental infections with the P. berghei model and the results of cytotoxicity on the cultures of VERO cells, demonstrating that C2 was better antimalarial than C1, but both did not exceed the antimalarial effect of Chloroquina under the same experimental conditions.












 uBio
uBio