Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Acta Médica Costarricense
On-line version ISSN 0001-6002Print version ISSN 0001-6012
Acta méd. costarric vol.58 n.4 San José Oct./Dec. 2016
Articles
Prevalence of cachexia related to cancer in patients at a primary level: a palliative approach
1Cuidados Paliativos. Área de Salud de Atenas.
2Subárea de vigilancia epidemiológica. Caja Costarricense de Seguro Social. yirleyvaa@gmail.com
Weight loss and malnutrition are common in cancer patients, both of which are the source of complications during the course of the disease. The maximum expression of malnutrition is tumor cachexia, a complex syndrome in which, along with a state of malnutrition, it includes weight loss, decreased muscle mass, anorexia and early satiety, weakness, anemia and edemas.1
Currently, other authors also point out that cachexia is “a complex metabolic syndrome associated with anorexia, inflammation, insulin resistance and increased muscle protein degradation and lipolysis”.1
The main clinical characteristic of cachexia associated with neoplastic disease is involuntary weight loss, which exceeds 5% in a short period of 3 to 6 months.2 Even other authors consider as a major criterion for the diagnosis of cachexia, a weight loss greater than or equal to 5% in the period of one year.3 This scenario is frequent among patients with malignant tumors and their result, malnutrition, leads to a series of complications in the form of immune system disorders and related to active cancer treatment, with these patients having a worse prognosis.4
The prevalence of cachexia in cancer patients is a common problem, since it is estimated that it ranges from 15% to 40% at the time of diagnosis and can increase up to 80% in cases of advanced disease.5 The most frequent types of tumors that are associated with this are those of gastrointestinal origin.6
The maximum expression of malnutrition in cancer is tumor cachexia, which will be directly or indirectly responsible for death in one-third of cancer patients,7 in fact, the degree of cachexia is inversely correlated with the survival time of the patient, and always implies an unfavorable prognosis. Of the patients with cancer, from 16 to 73% present the symptoms of cachexia.11
It is important to determine the prevalence of oncological cachexia in primary care and in palliative conditions to diagnose it, since weight changes are often overlooked, and these changes must also be studied in depth to make earlier diagnosis of cachexia in a neoplastic disease.
Once the cachexia is established, the most relevant aspect in its management will be the taking of preventive measures, and providing biopsychosocial and spiritual support,4 guided by a palliative care team, in the most opportune way possible, for the patient with terminal illness and his family, and thus guarantee a better quality of life. As there is no possibility of cure, palliation is the most viable alternative in this context.12
Due to all of the above and due to the absence of a timely diagnosis of malnutrition in these patients, it was essential to carry out the investigation to determine the prevalence of cachexia in primary health care, since it is the doctor at this level who has always the first contact with the patient and must recognize that he has to send patients with neoplastic diseases in early stages to an interdisciplinary team in palliative care.
Table 1 Distribution of people diagnosed with cancer, according to age group in years, in the EBAIS of San Isidro of Atenas, during the 2010-2013 period
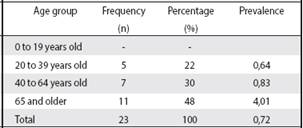
Source: our own information collected for the research * Population according to population pyramid of the EBAIS of San Isidro.
Methods
A cross-sectional observational study was performed in patients diagnosed with neoplastic disease and in palliative conditions, belonging to the EBAIS of San Isidro, from the Health Area of Atenas, Alajuela, Costa Rica, between 2010 and 2013.
All patients with oncologic disease diagnoses were selected according to ICD10 codes during the study period. As a source of data, the clinical records of the EBAIS, of these patients diagnosed with neoplastic disease in the health area under study, were used during the period 2010-2013.
Quantitative variables such as age, weight and length of all one-year consultations were collected in prior and subsequent consultations at the time of diagnosis. In addition, qualitative variables such as: gender, cancer type, religion, occupation, EBAIS ascribed, nationality, type of treatment, condition of the patient, treatment within the CCSS, inclusion in the Atenas palliative care program, personal pathological antecedents, Socioeconomic level, deaths per year and year of diagnosis.
The records of those patients due to immobilization syndrome or other causes of incarceration were excluded, as well as those who do not have a record in the EBAIS for reasons of private medical care, or foreigners who are not members of the CCSS health system, and which, therefore, were not weighed or measured.
Table 2 Distribution of people diagnosed with cancer, according to the EBAIS sector, during the 2010-2013 period
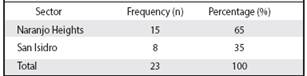
Source: our own information collected for the research * Population according to population pyramid of the EBAIS of San Isidro.
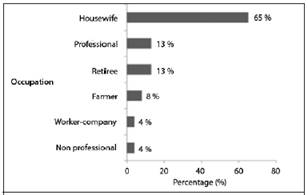
Figure 1 Distribution of people according to occupation in the EBAIS of San Isidro de Atenas, during the period 2010-2013. Source: our own information collected for research.
Cachexia was defined as any person within the study time who lost weight of at least 5% of the weight during the 12 months prior to diagnosis, or 12 months after diagnosis, or when body mass index (BMI) is less than 20 kg / m2.1 Cachexia is classified as mild, moderate or severe according to a weight loss of 5%, 10% or 15%, respectively.15
Frequency measures were calculated: absolute and relative, such as prevalence for qualitative variables and measures of central tendency, such as mean, and dispersion measures, such as the standard deviation for quantitative variables.
The percentage of weight loss was calculated one year prior to diagnosis, and the post-diagnostic weight loss, using the following formula and interpretation of weight loss percentage: percentage weight loss = habitual weight - current weight x100 / habitual weight.
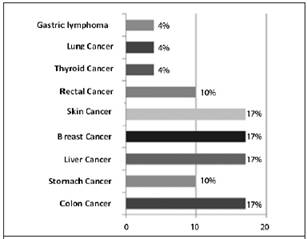
Figure 2 Distribution of the types of cancers in the EBAIS of San Isidro, Atenas, during the period 2010-2013. Source: our own information collected for researchinformation collected for research.
Mild weight loss was considered: <5% (mild cachexia); Moderate weight loss: 5-10% interpreted as moderate cachexia, and severe weight loss:> 10%, interpreted as severe cachexia.
The Epi info 3.5.4 program was used for the elaboration of a matrix that allowed consolidating the information and analyzing the data. This research was presented and approved by the Local Bioethics Committee (CLOBI) of the Health Area of Atenas.
Results
23 medical records that met the inclusion criteria for the study were analyzed. The mean age of all persons studied was 59.8 years ± 18 years. The most frequent age group was 65 years and older, with 48%; No cases were diagnosed between the ages of 0 and 19 (Table 1). 65.2% (n = 15) were female. All the people analyzed were of Costa Rican nationality.
In the EBAIS of San Isidro, the total prevalence of people diagnosed with cancer was 0.72%, the prevalence being higher in the group of 65 and over, with 4% (Table 1). As for the occupation of the people, 65% were housewives; non-professionals and workers or company dependents, were the least frequent, with 4% each, respectively (Figure 1).
The classification of cancers diagnosed in these individuals during the study period showed that the most frequent types were: colon, liver, and skin, with 17% each (Figure 2).
Regarding the inclusion of these people in the palliative care program of the Atenas Health Area, it was evidenced that 52% of the people analyzed are included in this program. In terms of the treatment received, the most frequently used was surgery, in 65% of cases, followed by palliative care in 43% (Table 3).
Table 3 Distribution of the types of treatment used in the patients analyzed in the Atenas Health Area, during the 2010-2013 period
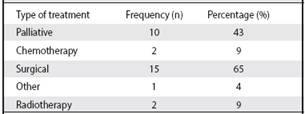
Source: our own information collected for research.
With regard to the condition of the disease, 63% of the patients who presented palliative condition were included in the palliative care program. Of the patients who had an oncologic condition resolved by medical treatment, none were included in a palliative care program. In addition, it was found that 71% of the patients who died were included in the palliative care program (Table 4).
The weight classification of these patients, according to their BMI, showed that 48% had a BMI higher than what was established as normal weight. 4% had BMI that was consistent with malnutrition (Figure 3).
After analyzing weight loss during the year following cancer diagnosis, a prevalence of cachexia (using as a diagnostic criterion the weight loss of more than 5% in the year following diagnosis of oncological disease) was determined in this area 21.7%, with this condition being more frequent in cancers of the digestive tract (8.7%) followed by lung 4.3% (Table 5). The weight gain during the year following their disease in the patients under study was 34.4%.
Discussion
Few investigations refer to the prevalence or incidence of cachexia in neoplastic disease. There is no significant evaluation of the weight loss prior to the diagnosis of cancer, nor the weight after diagnosis of oncological disease, for many reasons, being in our country one of them, the absence of medical training in palliative care.
Although there are few studies related to the subject, the prevalence of oncological cachexia in the population studied was within what the international bibliography mentions;5-11 however, it is necessary to mention that if this was based on body mass index, only 4.34% (n = 1) of the patients would be malnourished.
Table 4 Distribution of the condition of the disease and its inclusion in the Palliative Care Program of the Atenas Health Area, during the 2010-2013 period
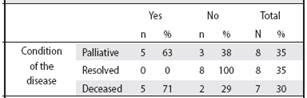
Source: our own information collected for research
As mentioned in the few studies done on the subject, cancers of the digestive tract and lung are the most associated with cancer cachexia. In none of the persons investigated was there a specification of symptomatology or other markers that may accompany the diagnosis and be taken as minor criteria for the diagnosis of cachexia, such as decreased muscle strength, fatigue, anorexia or other biochemical criteria, such as hemoglobin <12 g /dl, increased inflammatory markers (CRP, IL-6), hypoalbuminemia <3.2 g /dl, 1 which would also be important in the comprehensive approach of these individuals.
Knowing the process of demographic aging is fundamental in the country, as the older adults of tomorrow, were already born. The most numerous generations of Latin American countries, born between 1960 and 1980, entered the group of 65 years and more, from 2020.47 In the national bibliography and hospitalization, it is the group of people over 65 years old who has the highest incidence rates of some cancers. In this analysis, the age group of 65 and over was also the most frequent.
More than half of the people surveyed were in the palliative care program, which goes beyond what was mentioned and presented at the VIII Congress of the Spanish Society of Medical Oncology (SSMO), where only 30% of the 95,000 patients who died from cancer in Spain during the year 2000, received palliative care.48 This is of great significance for the Costa Rican society, although in spite of being an underdeveloped country, the coverage of palliative care services is being improved, and many patients with this disease benefit from an improvement in their quality of life, in a more integral form.
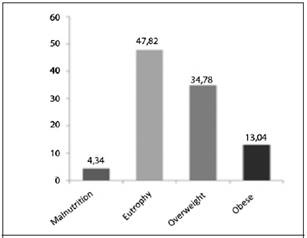
Figure 3 Distribution of weight according to BMI in patients with oncological diagnosis in the area of Health of Atenas during the 2010-2013 period. Source: our own information collected for research.
This makes us think of the need to value the inclusion of professionals with training or knowledge in nutrition among the palliative care teams, so that inter, multi and transdisciplinary work can be achieved in order to improve the quality of life of these people, and ensure that their families can participate more actively and safely in their care.
Early nutritional intervention is recommended. To do this, it is essential to follow up the nutritional status from the diagnosis and continue until the end of the treatment, elaborating an instrument that allows to include some parameters for the diagnosis of cachexia, including albumin, hemoglobin, hematocrit, muscle strength, frequently evaluated in the oncological patient or with palliative conditions, for an earlier intervention in their nutritional scope. A basic nutritional examination is also suggested, including anthropometric parameters, including weight, height, percentage of weight loss and skin folds.
Additionally, it is necessary to recommend, after the results of this research, to strengthen the training and sensitization of health professionals so that the nutritional history includes aspects related to treatment, intensity of vomiting and nausea, alterations of taste, presence or not of esophagitis, diarrhea, depression, alterations of the sleep / wake cycle and the order of the meals, among other aspects to be evaluated.
The syndrome of cachexia and anorexia causes a deterioration of the quality of life and the concepts of self-image and self-esteem in these patients. For this reason, the evaluation of the emotional aspects is very relevant to establish the support strategy and treatment of the patients, and the psychological support should be part of the approach in the palliative care programs.
Table 5 Evolution of weight of cancer patients, in the year after diagnosis, in the area of Health of Atenas, during the 2010-2013 period
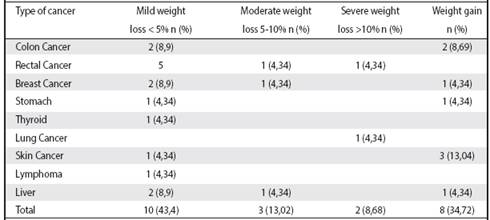
Source: our own information collected for the research.
Work performed in the Health Area of Atenas.
Affiliation of authors:
1 Palliative Care. Health Area of Atenas.
2 Subarea of epidemiological surveillance. Costa Rican Department of Social Security.
yirleyvaa@gmail.com
Referencias
1. Milke G, Rivera F . Síndrome de anorexia-caquexia. Rev Gastroenterol Mex. 2010; 75:205-7. [ Links ]
2. Jiménez G, Cabanas A, Fernández N, Chagues L, González C , Peón B, et al. Caracterización nutricional del síndrome anorexia-caquexia en el paciente oncológico pediátrico. Rev Cubana Pediatr. 2011; 83: 337-45. [ Links ]
3. Tuca R, Calcina B, González B, Gómez B. Caquexia oncológica. Med Clin. 2010; 135:568-72. [ Links ]
4. Sanz J, López V, Rivera F, López C, López A, Vega M. El síndrome anorexiacaquexia. SEOM. 2004; 1: 101-6. [ Links ]
5. Dufau L. Prevalencia de la desnutrición en el paciente oncológico. Rev DIAETA Arg. 2010; 28:31-6. [ Links ]
6. Soza S, Sánchez K, Motola D, Green D. Síndrome de anorexia- caquexia en el paciente oncológico. Gac Médica México. 2008; 144:435-40. [ Links ]
7. García L, Parejo Cs y Pereira C. Causas e impacto clínico de la desnutrición y caquexia en el paciente oncológico. Nutr Hosp. 2006; 3:10-6. [ Links ]
8. OPS. El cáncer en la región de las Américas, 2012. OPS. El cáncer en la región de las Américas, 2012. Recuperado el 19 de febrero de 2014. En: En: http://globocan.iarc.fr . [ Links ]
9. Situación del cáncer en Costa Rica. Rev Costarric Salud Pública. 2000;16:80-2. Print versión ISSN 1409-1429. En: http://scielo.sa.cr [ Links ]
10. Mestre R, Moya R, Velásquez G, Jiménez P, López V. Nutrición oncológica. SAMF y C. 2010. 24 páginas. Recuperado el 19 de febrero de 2014. En: En: http://samfyc.es>pdf>GdTonco [ Links ]
11. Moore C R, Poblete B, González G, Palomo G. Desgaste muscular en caquexia asociada a neoplasia: mecanismos proteolíticos implicados. Rev Biomed. 2007; 18:182-91. [ Links ]
12. Lara S, Tamayo V, Sandra P, Gaspar C. Manejo del paciente terminal. Rev Cancerología. 2006; 1:283- 295. [ Links ]
13. Fearon K, Strasser F, Anker SD. Consenso internacional sobre la definición de la caquexia por cáncer. J Lancet Oncol. 2011; 12:489-95. [ Links ]
14. Cancer E, Canovas. G, Durán M, Álvarez J, Gorgojo J. Nutrición basada en la evidencia en el cáncer como enfermedad caquectizante. Endocrinol Nutr. 2005; 52:91-6. [ Links ]
15. Milke G, Rivera F R. Síndrome de anorexia caquexia. Rev Gastroenterol Mex. 2010; 75:205-7. [ Links ]
16. Harrison. Principios de Medicina Interna. XV Edición en español. Editorial Mc Grawll Hill- Interamericana. 2009; 297-299. [ Links ]
17. Herrera E., Bruera E. Nuevos fármacos potencialmente útiles para el tratamiento de la caquexia en Cuidados Paliativos. Med Pal. 2001:144-58. [ Links ]
18. Casas F T. Principales síntomas secundarios asociados a los tratamientos antineoplásicos: cirugía, radioterapia y quimioterapia. 2007; 53-61. [ Links ]
19. Fitzgibbon D R, Loeser J D. Dolor asociado al cáncer. Evaluación, diagnóstico y tratamiento. Barcelona España: Wolters Kluwer Health España, S.A. 2011; 379. [ Links ]
20. Casas A, Valentín. V, Benavides. M, Camps. C, Carulla. J, González. M, Pascual.A. Guía de anorexia y caquexia. Soc Esp de Oncol Med. 2005; 47-55. [ Links ]
21. Sosa-Sánchez R. Síndrome de anorexia-caquexia en el paciente oncológico. Recuperado el 4 de enero de 2014. En: En: http://new.medigraphic.com/cgi-bin/resumenMainI.cgi?IDARTICULO=21453&IDPUBLICACION=2181&IDREVIS TA=16&NOMBRE= [ Links ]
22. Camps C. Resúmenes de ponencias I simposio SEOM de Cuidados en oncología médica. 2004. 77 páginas. Recuperado el 4 de enero 2014. En: En: http://seom. org>socios>2004Sep_30Pon [ Links ]
23. Sánchez. K, Sosa. R, Green. D, Méndez. N. Observaciones sobre patogénesis de la anorexia asociada a cáncer y su regulación por el sistema nervioso central. Rev Costarr Salud Pública. 2011; 26: 677-88. [ Links ]
24. Casado, H. Estudio de fase II rabdomizado de dos niveles posológicos de acetato de megestrol versus placebo para el tratamiento de la anorexia y de la caquexia en pacientes con cáncer locorregional avanzado o metastásico. Tesis doctoral. Universidad Complutense de Madrid. España; 2009. 167 páginas. Recuperado el 19 de febrero de 2014. En: En: http://eprints.ucm.es> [ Links ]
25. Argilés J M, Busquets S, López Soriano F J, Figeras M. Fisiopatología de la caquexia neoplásica. Nutr Hosp. 2006; 2: 4-9. [ Links ]
26. Ferriols. F, Toldera. M. El síndrome caquéctico en el paciente oncológico: fisiopatología, manifestaciones clínicas y tratamiento. Rev Farmacia Hosp. 2003; 27:308-16. [ Links ]
27. Planas. M, Puiggrós. C, Redecillas. S. Contribución del soporte nutricional a combatir la caquexia cancerosa. 2006; 21:27-36. [ Links ]
28. Sierrasesumaga L. Soporte nutricional en el niño con cáncer. Nutrición en pediatría. II Edición. Madrid: Ergón, 2003; 435-444. [ Links ]
29. Norma Nacional de Soporte Nutricional para el paciente con cáncer. Ministerio de Salud. Costa Rica. 2012. Recuperado el 19 de febrero de 2016. 100 páginas. En: En: http://ministeriodesalud.go.cr/...de...salud/normas...norma.../file [ Links ]
30. Marín M, Castillo R, Laurenco T, García M, Loría V. Evaluación del riesgo nutricional e instauración de soporte nutricional en pacientes oncológicos, según el protocolo del grupo español de nutrición y cáncer. 2008; 23: 458-68. [ Links ]
31. Bertolino M, Bonacina R, Sofía B, Cullen C, Noemy D, Farías G, et al. Manual de Cuidado Paliativo Argentino. Fundación FEMEBA. 2007. [ Links ]
32. De Nicola D, Flores R J, Zamora V J. Tratamiento Nutricio del paciente con cáncer gástrico. Rev Cancerología Mex. 2007; 337-44. [ Links ]
33. Fauci A, Kasper D., Braunwald E. Harrison Principios de Medicina Interna. 16 Edición. Editorial Mc Grawll Hill- Interamericana. 2009; 298. [ Links ]
34. Marian M., Robert S. Clinical Nutrition for oncology patients. USA: Editorial Jones and Bartlett, 2010; 379-408. [ Links ]
35. Espinós J, Reina C., de la Cruz S., Olivier C, Hernández A, Fernández Hidalgo O., et al. Tratamiento hormonal del cáncer de mama. Rev Med Univ de Navarra. 2008; 52:40-8. [ Links ]
36. García G M. Aumento de peso en cáncer de mama. Enfermería Oncológica. 2007; 77-80. [ Links ]
37. González C M. Asistencia nutricional en el paciente oncológico. Una forma de mejorar su calidad de vida. 2007; 26:63-69. [ Links ]
38. Rabanal T M, Rans P N. Uso terapeútico de los cannabinoides: estudio seguivex y emesis. Boletín de información terapeútica. 2008; 20:26-30 [ Links ]
39. Cardona D. Tratamiento farmacológico de la caquexia cancerosa. Rev Nutr Hosp. 2006; 21:17-26. [ Links ]
40. Valenzuela B. Rodrigo, Bascuñan G. Karla, Chamorro M. Rodrigo, Valenzuela B. Alfonso. Ácidos grasos omega - 3 y cáncer una alternativa nutricional para su prevención y tratamiento. Rev Chil Nutr. 2011; 38: 219-26. [ Links ]
41. Camarero González Emma. Nuevos nutrientes en caquexia cancerosa. Enfermería Oncológica. Sociedad Española de Enfermería Oncológica. 2006. 80 páginas. En: http://seeo.org [ Links ]
42. Silvério R, Laviano Al, Rossi F F, Seelaender M. Levocarnitina y caquexia oncológica: Clínica y aspectos experimentales. Springer. 2011; 37-44. 8 páginas. En: http// www.nutritotal.com.br/.../217--consensocaquexia.pd [ Links ]
43. Arends J. ASPEN Support Practice Nutricion Manual. Estados Unidos de América: ASPEN. ASPEN A.S. 2006. 32 páginas. En: http//achinumet.cl/guias-soporte/Guias%20Soporte%20Nutricional%20UCI.pdf [ Links ]
44. Marín M., Laviano A., Pichard C, Gómez C. Relación entre la intervención nutricional y la calidad de vida en el paciente. Revista Nutrición Hospitalaria. 2007; 22: 337-50. [ Links ]
45. Urdaneta A. La nutrición del paciente en Cuidados Paliativos. Guía de Cuidados Paliativos SECPAL. España, 2002; 169-187. [ Links ]
46. Casas F T, Valentín M V, Benavides O M, Campos H C, Carrulla T J, González B M, et al. Guía anorexia y caquexia. Sección española de oncología médica; 2010. [ Links ]
47. Reyes C D, González O J, Mohart B A, Meneses G A. Epidemiología del dolor por cáncer. Rev Soc Esp Dolor. 2011; 18: 118-34. [ Links ]
48. La situación del cáncer en España. Ministerio de Sanidad y Consumo. Cyan, Proyectos y Producciones Editoriales, S.A. Madrid, 2015; 1-188. [ Links ]
49. Fernández L M, Sáenz F C, Prada M F, Urrutia S A, Bardasco A, Álves P M, et al. Desnutrición en pacientes con cáncer; una experiencia de cuatro años. Rev Nutr Hosp. 2013; 28:372-81. [ Links ]
bold: ; Received: May 12, 2016; bold: ; Accepted: August 11, 2016











 text in
text in 


