Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Acta Médica Costarricense
On-line version ISSN 0001-6002Print version ISSN 0001-6012
Acta méd. costarric vol.58 n.4 San José Oct./Dec. 2016
Articles
Antibiotic sensitivity profile of bacteria in urinary tract infections
1Facultad de Ciencias Médicas, Universidad Católica de Honduras.
Urinary tract infections (UTIs) have represented, over time, a reason for consultation in all private and public health institutions worldwide. Due to its high prevalence and frequent inadequate use of antibiotics, it is necessary to determine the most common causal agents, populations most affected and patterns of local sensitivity and resistance, to achieve better clinical results and to establish a better use of antibiotics.
UTIs usually occur in a variety of ways, depending on their chronological evolution or site of urinary tract infection, with clinical syndromes: asymptomatic bacteriuria, recurrent UTI, complicated UTI, UTI associated with bladder catheterization, acute cystitis and acute pyelonephritis.1
In the collection of published regional articles, results were found that show a wide difference between Escherichia coli and the rest of colonizing bacteria of the urinary tract. Of these, it is worth mentioning: Klebsiella pneumoniae, Proteus mirabillis, Enterobacter spp, Enterococcus spp, Citrobacter, Pseudomonas aeruginosa, Staphylococcus saprophyticus, streptococci, Serratia sp, Acinetobacter spp, amongst others.1-7
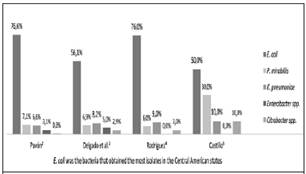
Pavón et al., in a study with 1256 patients in a third level hospital in Nicaragua, it was obtained 76.7% of E. coli isolates.2 Delgado, meanwhile, had 340 samples in another hospital of the same category in Costa Rica, of which 56.1% corresponded to E. Coli.3 Rodríguez et al. They worked 32 samples at another hospital of the same level in Honduras and reported 76% of E. coli.4 On the other hand, Castillo, with 20 samples in another hospital of the third level and in an asylum of disabled in Honduras, 50% of cases of E. Coli were reported.5 Figure 1 shows the comparison between the main isolates of the reviewed studies. This data is similar to those of other authors, such as Guevara et al., in which 71 samples showed that E. coli was present in 63.89% of the cases.6
The cases of UTI associated with bladder catheterization are closely related to the duration of bladder catheter use. The reported bacteria are usually the same cause in the other syndromes, with E. coli being the most frequently found germ and accompanied by Klebsiella spp, Enterococcus spp, Proteus spp, Pseudomonas aeruginosa and Candida spp.7
The clinical context is also an important factor for the initiation of an antibiotic regimen, due to the susceptibility to UTI complications. Febrile infants, 2 to 24 months of age, should initiate treatment and change the therapeutic regimen by obtaining culture result according to specific patterns of sensitivity.8
The purpose of this study was to provide information regarding the bacteria frequently found as a cause of UTI and its patterns of sensitivity and resistance in the localities of San Pedro Sula and El Progreso, Honduras. This will help improve epidemiological surveillance of these phenomena. It is outside the scope of this study to delve into the characteristics of each pathology.
Nor is it intended to describe whether these bacteria were acquired in a hospital or community. It is extremely important to analyze the sensitivity and antibiotic resistance in urine cultures, since this diagnostic tool is used to provide specific medical treatment to patients with UTI. By having an analysis of an important sample of these exams, results that best refer to antibiotic susceptibility profiles can be obtained, which translates into results that could be of importance to orient the empirical therapy of UTIs when the urine culture is not available.
Methods
This study is descriptive observational, transversal and retrospective.
The range of data collection included cities with high urban population density, so it was decided to take data from the different laboratories in the northwestern area of Honduras, which includes the cities of El Progreso and San Pedro Sula. San Pedro Sula is a part of the department of Cortés, and the city of El Progreso is located in the department of Yoro.
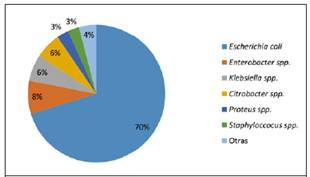
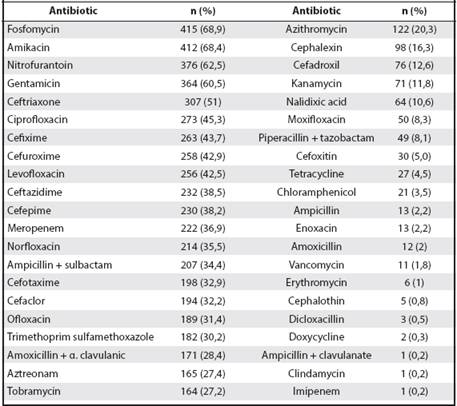
Figure 2 Results of Urine cultures of San Pedro Sula and El Progreso, Honduras, from February to June 2014 (n = 602) E. coli was the most isolated uropathogen in two of the most densely populated cities of Honduras
The results of the urine cultures were obtained through different researchers in laboratories under strict norms of privacy and with the proper authorization of each institution source of the samples. A format was used for each researcher, created by the study coordinators.
The method used in all laboratories to obtain antibiotic resistance and sensitivity profiles was Kirby Bauer, with sensitivity disks. 47 sensitivity discs were used in all laboratories. Each researcher reviewed the database of Bueso Arias (San Pedro Sula), Fiallos (San Pedro Sula), UDE (El Progreso), Calix (El Progreso), Bendana Hospital (San Pedro Sula), Valle Hospital San Pedro Sula), Clinical Diagnostic Center (San Pedro Sula). After the complete collection, the analysis was performed by the researchers JZ and HV.
The inclusion criteria for the samples were: bacterial microbiological isolation obtained from urine samples of patients of any age, treated on an outpatient basis by public centers or in private consultation.
We included samples from participating laboratories without gender differentiation, including pregnant women.
Microbiological isolates positive for fungi or parasites were excluded from the analysis.
The variables from which data were collected were: age, sex, microorganism and antibiotic sensitivity test. The research protocol included origin (domicile), however, this variable was not analyzed, since almost no source provided such information.
Each variable was obtained from the database of laboratories that agreed to provide specific information, without jeopardizing privacy or exposing the name of each of the subjects in the study. No variable or other information was obtained externally from the assigned laboratories.
The samples were not placed in one or another category depending on any specific variable, which could affect the results in a positive way for the benefit of the study. The possible information bias includes the absence of some antibiotic sensitivity discs, lacking results of other sensitive or resistant antimicrobials, which without altering the results, leaves out some antibiotics that could be resistant or sensitive than those presented in this study. It is also unknown if the samples came from patients with a primary infection, chronic infection, or if they had particular risk factors that could show different results.
A total of 602 samples were obtained and analyzed.
Quantitative variables were managed using coding. In the case of the age, in ranges of 10 years between 0 and 70. Regarding the antibiogram, the division of antibiotics was performed, to which the bacterium presented resistance, sensitivity and intermediate sensitivity.
All the results were sent to a data matrix in the program Microsoft Excel 2013®, to determine the percentages.
The study was carried out in line with good clinical practice, derived from the International Conference on Harmonization and the Helsinki Declaration. In addition, all existing laws were complied with. It was approved by the institutional ethics committee and local authorities, before starting the study.
Results
A total of 602 culture results were collected, of which 509 (84.6%) came from women and 93 (15.4%) from men. With respect to age, 84 samples (14%) belonged to individuals between 0-10 years old, 30 (5%) to cases between 11-20 years old, 260 (43%) between 21-60 years and 205 of the samples (34%) were for people over 61 years of age. No age data were obtained in 23 samples (4%) in which 18 were females and 5 males.
Data generated
Of the 602 samples positive for bacteria in the urine culture, Escherichia coli was isolated in 70.4%, Enterobacter spp. in 7,8%, Klebsiella spp. in 6,3%, Citrobacter spp. in 6,1%, Proteus spp. in 2,8%, Staphyloccocus spp. in 2,7%, Pseudomonas aueruginosas in 1,8%, Streptococcus spp. in 1,2%, Hafnia alveii in 0,3%, Morganella morgagni in 0,2%, Serratia marcenscens in 0,2% y Neisseria gonorrhoeae, in 0,2% (Figure 2).
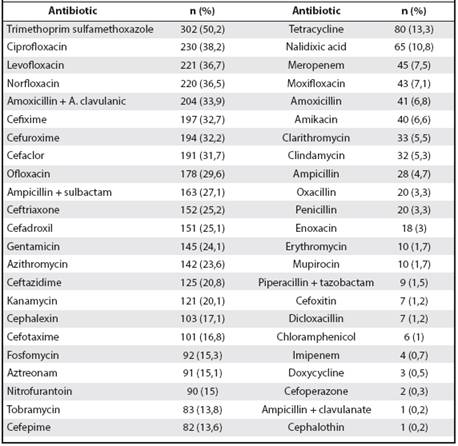
A total of 47 discs were used to determine the resistance and sensitivity profiles in each bacterial isolation. Antibiotics with high percentages of resistance were: trimethoprim sulfamethoxazole (50%), followed by third-generation quinolones with similar percentages, ciprofloxacin (38.2%), levofloxacin (36.7%) and norfloxacin 36.5%). The most resistant antibiotic in this study was amoxicillin plus clavulanic acid (33.9%) (Table 1).
According to the sensitivity profiles, the most effective antibiotics were fosfomycin (68.9%), amikacin (68.4%), nitrofurantoin (62.5%), gentamicin (60.5%) and ceftriaxone (50.1%) (Table 2).
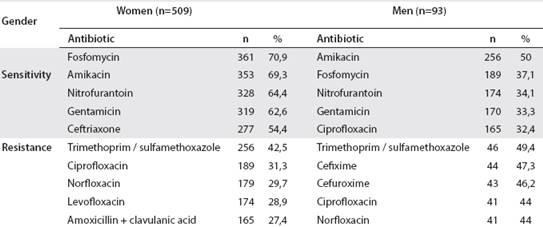
There was a clear difference between the number of women (n = 509) and men (n = 93), in the total of samples studied. The profiles of sensitivity and antibiotic resistance between men and women were similar to the general sensitivity. However, in men, resistance to some cephalosporins is greater, but not in women, where the same pattern is maintained as in general resistance (Table 3).
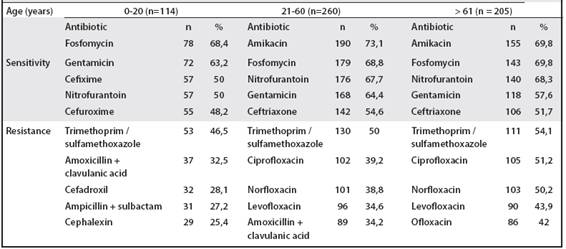
Patient ages were categorized into the following ranges of 0-20 years (n = 114), 21-60 years (n = 260), over 61 years (n = 205). The profiles were maintained in a similar way as reported, however, in the group of 0-20 years, it was shown that there is a sensitivity of 48% to cefuroxime. It should be noted that the percentages of resistance were higher in people in the group over 61 years (Table 4).
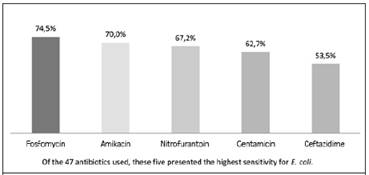
Taking into account that the E. coli bacterium was the one with the most isolates presented (n = 424) and the one that has been studied the most in the literature, the resistance pattern was analyzed independently. It was evidenced that this bacterium, in the isolates analyzed, had a sensitivity profile similar to that of general sensitivity. However, sensitivity to ceftazidime was found to be only 53.5% (Figure 3). It was also observed that E. Coli presented significant resistance to TMP-SMX and four third generation quinolones (Figure 4).
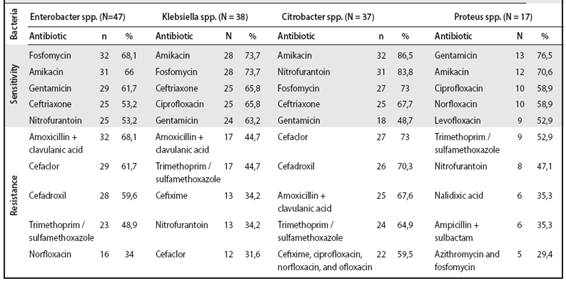
The profiles of the other bacteria that presented in this study with less frequency of isolation, showed the following. Enterobacter spp was isolated in 47 samples and presented a sensitivity profile similar to that of all isolates; But it was observed that the antibiotics to which it presented greater resistance were amoxicillin plus clavulanic acid, cefaclor and cefadroxil. On the other hand, Klebsiella spp (n=38) had a sensitivity profile with good sensitivity to ciprofloxacin. As for resistance, there was similar pattern to that presented with respect toEnterobacter. Citrobacter spp (n=37) had a resistance pattern that showed resistance to quinolones and several cephalosporins. Finally, Proteus (n=17), presented an important resistance pattern with antibiotics that did not appear in the previous reports (azithromycin and ampicillin + Sulbactam) (Table 5).
Discussion
Antibiotics such as fosfomycin and nitrofurantoin, in this study show a good sensitivity profile in the isolates of the urine cultures analyzed, suggesting that they are a good option for the empiric treatment of uncomplicated low UTIs, since they are oral drugs without good Renal penetration. It was also shown that antibiotics such as quinolones had a high resistance profile throughout all analyzes.
Table 5 Main patterns of sensitivity and antibiotic resistance of other bacteria identified most frecuently in the study
Amikacin showed good sensitivity profile throughout all the results, as has been reported by other authors.9-13 dDespite this, the antibiotic would not be used as empirical therapy for uncomplicated UTIs, but for the management of a UTI where there is a multiresistance towards the other antibiotics that could cause fewer adverse events. The quinolones had high percentages of resistance, which is important, since some authors in Latin America report a high resistance to quinolones,9-12,14-15 while others, a good sensitivity,16 which leads to think that at the moment of a possible empirical therapy, the endemic profiles of each country should be taken into account.
Certain authors consider age as a factor of importance with respect to increased resistance. Resistance is proposed to increase in people older than 60 years compared to those of younger age, which is usually associated with the use of catheters and chronic diseases.17,18 It is clear that in the study there was an interesting difference between age groups and resistance percentages. As the age group was higher, the percentages of resistance were also slightly higher.
The antibiotic with the highest percentages of resistance throughout the study was TMP-SMX, which is in agreement with other studies in Latin America where resistance to TMP-SMX is frequent.11-16,19-21 However, it has also been reported in the region, some sensitivity to TMP-SMX in the urine cultures.9,22
It is important to mention that, over time, good sensitivity profiles for nitrofurantoin have been beginning to be reported, albeit with limited spectrum; This antibiotic has been referred by many authors with a sustained sensitivity above 70% and even 80%.3,10-12,14,20 In addition to this pattern, some authors outline a low resistance profile for nitrofurantoin.13,15-16 This provides an interesting profile at the time of selection as empirical therapy for the management of uncomplicated low UTIs, in order to obtain high referral rates. In the study it was evident that this antibiotic, throughout all the analysis groups, was always sensitive above 50%.
Despite the fact that due to the method used for the isolation of the bacteria, direct detection of strains possessing extended spectrum beta-lactamases (ESBL) or cAMP was not made, it is necessary to mention as the Enterobacteriaceae acquire resistance by the mentioned mentioned above, and somehow could be inferred if indeed they are strains with these characteristics. It is known that the Enterobacteriaceae positive for ESBL possess significant resistance to ampicillin, ampicillin-sulbactam, ceftriaxone, sulfamethoxazole trimethoprim and quinolones.9, 14- 17, 23 This is of paramount importance, since the study shows that most of the isolates had a significant resistance to the antibiotics mentioned above. Secondly, Enterobacteriaceae also demonstrate a significant phenotypic characteristic, such as beta-lactamase cAmp, which confers significant resistance to third-generation cephalosporins.17,13
It would be advisable to carry out more observational studies in all the zones of the country, in order to promote the development of a local guide directed to the ambulatory management of the urinary infections of a staggered form, based on the resistance patterns that have in the region, through comparative studies.
Padgett, et al., in the Hospital of Specialties of the Honduran Institute of Social Security, reported the evolution of resistance of E. Coli from 2006 to 2009, through the committee of prevention and control of nosocomial infections. There was a slight decrease in resistance to ciprofloxacin from 42% to 35%, and ceftriaxone from 47% to 31%.24
The development of epidemiological and pharmacological surveillance programs would provide a powerful tool to reduce levels of antibiotic resistance related to causes such as underdosing, inappropriate use of antibiotics, among others. It is proposed to develop local prospective studies to determine which antibiotics would be most useful on a regional basis. The results encourage more complex studies, determine that there are actually better treatment options and have a good therapeutic escalation regarding patient management.
One of the limitations of the study was that the sensitivity disks were not the same in all laboratories. We did not obtain the addresses of the patient’s places of origin, which would have provided breadth with respect to which areas have a higher prevalence of certain bacteria or antibiotic resistance in the metropolitan area, to determine the heterogeneity of this area.
Funds: The financing of the study belonged to each participant researcher, for which it was stated that there was no conflict of interest.
Acknowledgments: to the reviewers of this article: Bárbara Bribiesca, MD, Monique Baudrit, MD and Daniel Bustos, MD; to those who provided results of urine cultures; to the laboratories Fiallos, Bueso Arias, UDE, Del Valle Hospital, Bendaña Hospital and Clinical Diagnostic Center, of the cities of San Pedro Sula and El Progreso, Honduras. For their logistical support to carry out the study and the data collection, the collegues Ángel Martínez, Eylin Urbina, Eduardo Borjas, María Elena Chavarría, Heidy Fúnez, Osman Fuentes, Dilcia Lagos, Rocío Lagos, Fernando Paz, María Mandujano, Shirley Baiza and Saúl Paz.
Work performed at the Faculty of Medical Sciences, Catholic University of Honduras, San Pedro y San Pablo campus.
Affiliation of authors:
1 Faculty of Medical Sciences, Catholic University of Honduras.
2 Honduras League Against Cancer. Abbreviations: UTI, urinary tract infection; TMP-SMX, trimethoprim sulfamethoxazole; ESBL, extended spectrum beta-lactamases
Conflict of Interest: the authors declare no conflicts of interest. jczm1991@gmail.com
Referencias
1. Wurgaft Andrés. Infecciones del Tracto Urinario. Rev Med Clin Condes. 2010; 21:629-633. [ Links ]
2. Pavón-Gómez NJ. Diagnóstico y tratamiento de infección de las vías urinarias en embarazadas que acuden a Emergencia y Consulta Externa del Hospital Bertha Calderón Roque en Managua, Nicaragua. Perinatol y Reprod Humana. 2013;27:15-20. [ Links ]
3. Delgado M, Sáenz C. Etiología y sensibilidad bacteriana de las infecciones del tracto urinario. Rev Médica Costa Rica y Centroam. 2004;61:113-118. [ Links ]
4. Rodríguez G. Pielonefritis en niños, estudio epidemiológico clínico en el Instituto Hondureño de Seguridad Social. Honduras Pediatr. 2005;25:5-16. [ Links ]
5. Castillo D. Tratamiento de la infección urinaria en el niño. Honduras Pediatr. 1968;3:254-261. [ Links ]
6. Guevara A, Machado S, Manrique E. Infecciones urinarias adquiridas en la comunidad: epidemiología, resistencia a los antimicrobianos y opciones terapéuticas. Kasmera. 2011;38:87-97. [ Links ]
7. Nicolle L. Catheter associated urinary tract infections. Antimicrob Resist Infect Control. 2014;3:23. [ Links ]
8. Subcommittee on Urinary Tract Infection, Steering Committee on Quality. Urinary tract infection: clinical practice guideline for the diagnosis and management if the initial UTI in Febrile Infants and Children 2 to 24 months. Pediatrics. 2011;128:595-610. [ Links ]
9. Leal AL, Cortés JA, Arias G, Ovalle MV, Saavedra SY, Buitrago G, et al. Emergencia de fenotipos resistentes a cefalosporinas de tercera generación en Enterobacteriaceae causantes de infección del tracto urinario de inicio comunitario en hospitales de Colombia. Enferm Infecc Microbiol Clin. 2013;31:298-303. [ Links ]
10. Guevara A, Machado S y Manrique E. Infecciones urinarias adquiridas en la comunidad: epidemiología, resistencia a los antimicrobianos y opciones terapéuticas. Kasmera. 2011;38:87- 97. [ Links ]
11. Orrego-Marin CP, Henao-Mejia CP y Cardona-Arias JA. Prevalencia de infección urinaria, uropatógenos y perfil de susceptibilidad antimicrobiana. Acta Med Colomb. 2014;39:252-258. [ Links ]
12. Pinto J, Carvajal P, Lopez Y, Palacio D, Torres T, Restrepo M, et al. Agentes etiológicos de infecciones del tracto urinario y su resistencia a antibióticos en población pediátrica; Medellin, Colombia. Arch Med (Manizales).2011;11:159-168. [ Links ]
13. Hoyos A, Serna L, Ortiz G y Aguirre J. Infección urinaria adquirida en la comunidad en pacientes pediátricos: clínica, factores de riesgo, etiología, resistencia a los antibióticos y respuesta a la terapia empírica. Infectio. 2012;16:94-103. [ Links ]
14. Paramo-Rivas F, Tovar-Serrano A y Rendon-Macias M. Resistencia antimicrobiana en pacientes con infección de vías urinarias hospitalizados en el servicio de Medicina Interna del Nuevo Sanatorio Durango, de enero a diciembre de 2013. Med Int Méx. 2015;31:34-40. [ Links ]
15. Sánchez S, Reyes P y Bermúdez D. Susceptibilidad microbiológica de los uropatógenos aislados en la comunidad en Colombia periodo 2009-2013. Rev. Medica. Sanitas. 2015;18:54-64. [ Links ]
16. Rendon MA, Reyes A, Rosas JB y Rodríguez F. Infecciones de vías urinarias. Patrón de resistencia in vitro de E. Coli y E. Coli ESBL a quinolonas, trimetoprimasulfametoxazol y nitrofurantoína. Med Int Mex. 2012;28:434-439. [ Links ]
17. García-Mostajo JA, Alva-Díaz C y Rivera-Morón P. Frecuencia de infección del tracto urinario intrahospitalaria por Enterobacterias productoras de betalactamasas de espectro extendido y factores asociados en un hospital. Rev Soc Peru Med Interna. 2015;28:113-120. [ Links ]
18. Sejia V, Frantchez V, Ventura V, Pintos M y González M. Factores asociados al desarrollo de infección urinaria de origen comunitario causada por Escherichia coli resistente a fluoroquinolonas. Rev Chilena Infectol. 2014;31:400-405. [ Links ]
19. Velez C, Serna-Higuita LM, Serrano AK, Ochoa-Garcia C, Rojas L, Bedoya AM, et al. Perfil de resistencia de los patógenos causantes de infección urinaria en la población pediátrica y respuesta al tratamiento antibiótico, en un Hospital Universitario 2010-2011. Colomb Med. 2014;45:39-44. [ Links ]
20. Bogantes R. Rodríguez J. Resistencia bacteriana a los antibióticos en infecciones del tracto urinario bajo, en pacientes en consulta externa en el área de salud de Palmares. Fármacos. 2004; :1-2. [ Links ]
21. Weber N. Estudio retrospectivo sobre resistencia antibiótica en la población del área de salud de La Unión entre enero y diciembre de 2010. Rev Médica Costa Rica y Centroam. 2012; 69:41-45. [ Links ]
22. Machado-Alba JE y Murillo-Muñoz MM. Evaluación de sensibilidad antibiótica en urocultivos de pacientes en primer nivel de atención en salud de Pereira. Rev. salud pública. 2012; :710-719. [ Links ]
23. Herrera C, Navarro D y Täger Marlis. Etiología y perfil de resistencia antimicrobiana en infección del tracto urinario en niños, Valdivia 2012. Rev Chilena Infectol. 2014; :757-758. [ Links ]
24. Padgett D, Luque M, Rivera D, Galindo C, Zepeda L y Hernández A. Resistencia Antimicrobiana en Bacterias Aisladas en el Instituto Hondureño de Seguridad Social. Rev Med Hondur. 2011;79:117-121. [ Links ]
Received: January 25, 2016; Accepted: August 18, 2016











 text in
text in