Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Acta Médica Costarricense
On-line version ISSN 0001-6002Print version ISSN 0001-6012
Acta méd. costarric vol.53 n.4 San José Dec. 2011
Clinical case
Evans Syndrome of Sudden Onset in Pregnancy
Jorge Barboza-Retana, Pilar Bogantes-Ledezma, William Carballo-Gutiérrez, Jorge Díaz-Camacho
*Contact informationAbstract:
Thrombocytopenia complicates up to 10% of pregnancies. Evans syndrome is the coexistence of immune thrombocytopenia with autoimmune hemolytic anemia. We report a case of Evans syndrome during pregnancy complicated by preeclampsia and fetal neutropenia. A 20year-old primigravida, previously healthy, presented at 34 weeks of gestation epigastric pain, thrombocytopenia and preeclampsia. She underwent cesarean delivery for HELLP syndrome. In the 25th postpartum day, she was readmitted to the hospital with severe thrombocytopenia, platelet count in 2000x mm3, anemia, hemoglobin 5.3 g/dl and fever. The direct Coombs was positive and subsequent analysis showed the presence of platelet antibodies, and anticardiolipin. She received blood and platelet transfusions. She was treated with prednisone, plasmapheresis, azathioprine, and finally recovered 10 days in an intensive care unit.
Keywords: Evans syndrome, thrombocytopenia, autoimmune hemolytic
anemia, pregnancy
The Evans syndrome is a rare condition, initially reported in children, and characterized by the simultaneous or successive occurrence of thrombocytopenia and hemolytic anemia; although the actual incidence is not well known, according to estimations it affects between 1.8% and 10% of patients with ITP.
Evans was the first one to describe the syndrome as such in 1951, and the first published case about its occurrence during pregnancy dates back to 1966. Since then, there have been few worldwide reports about Evans syndrome in association with pregnancy. A total of 14 publications, which include clinical cases and systematic reviews, have been reported. This is why a case diagnosed at the Fetomaternal Medicine Unit of the HCG is presented.
Clinical case
A 20-year old female, resident of Moravia, unemployed, with 34-weeks of gestational age, primigravida without prenatal care; is referred from the clinic of Curridabat due to severe abdominal pain, predominantly epigastric, nausea and vomiting. She is admitted at the Emergency Service of the HCG, where a personal history of allergy to clindamycin, amoxicillin and Voltaren is recorded. She does not smoke or use drugs. Her vital signs were stable, with BP 100/70mmHg, HR 88 per minute, FHR140 per minute.
The abdominal ultrasound is reported as normal; an obstetrical ultrasound indicates: "Fetometry for 28 weeks, estimated fetal weight of 1201 grams, normal amniotic fluid index, fetal biophysical profile normal."
She is admitted to the maternity rooms; epigastric pain persists, her blood pressure rises to 167/102 mmHg, mean arterial pressure of 126 mmHg. She begins treatment with magnesium sulfate and the new laboratory tests show a platelet count of 42 000 x mm3.
In the perinatology session, the decision to interrupt the pregnancy is taken, due to severe preeclampsia and HELLP syndrome. The newborn was born alive through a Kerr caesarean; with a weight of 1200 grams, Apgar 9-9, small for its gestational age, with severe neutropenia; she remains hospitalized for 11 days because of persisting severe thrombocytopenia and epigastric pain. Her symptomatology improved and was discharged on February 13, with a reference for further control in the Rheumatology outpatient clinic.
She is readmitted to the HCG’s maternity with a history of persistent abdominal pain, nausea, anemia and severe thrombocytopenia, in postpartum day 25, 17 days after discharge.
The patient is admitted to the intensive care unit because her parameters do not improve and the destruction of platelets and hemoglobin is so active that, despite several transfusions of platelets and packed red blood cells (PRBC) during two days, platelet count remained in 1000 and Hb in 2g/dl; treatment with prednisone and immunoglobulin is started.
On February 28 she begins treatment with steroids and gamma globulin, 20 grams IV a day; she receives a transfusion of 2 units of filtered PRBC and 6 units of platelets.
The medical condition improves spontaneously after 10 days of hospitalization and the patient is transferred to the Rheumatology unit, with a platelet count of 70 000 x mm3 and Hb of 9 g/dl; because of her improving conditions, she is discharged and continues under control at the outpatient clinic.
Discussion
The Evans syndrome is a chronic hematological condition, initially described as the simultaneous or sequential occurrence of autoimmune hemolytic anemia, Coombs-Positive and autoimmune thrombocytopenia.1-3
The association to pregnancy was reported by Silberstein in 1966;1,2 cases in worldwide literature are scarce, and the association to pregnancy is an even rarer entity.
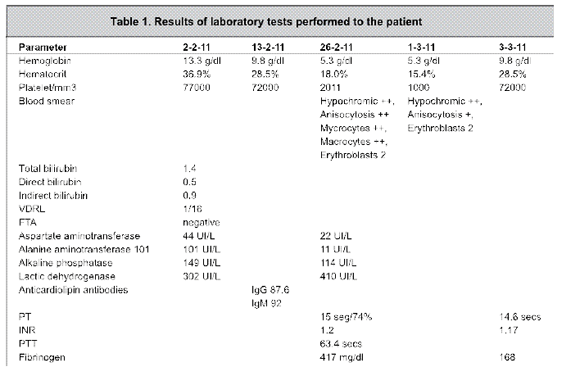
It may occur alone or together with the presence of another autoimmune disease like systemic lupus erythematosus, antiphospholipid syndrome and autoimmune lymphoproliferative syndrome.1,3 The patient was diagnosed with an active antiphospholipid syndrome in the immediate postpartum period, with positive anticardiolipin antibodies (IgG 87.62 and IgM greater than 92, both positive), a reactive VDRL 1 in 16 with negative FTA.
In some cases, the Evans syndrome may precede the development of a myelodysplastic syndrome, or of a non-Hodgkin lymphoma.
Only 4% of the cases show a platelet count below 20 000 platelets/mm3.5,6 The patient showed platelet counts below 1000 platelets/mm3. As with hemolytic anemia, the Evans syndrome may have one immunologic cause. In the case under discussion, diagnosis occurs on the patient’s late postpartum period.
In a systematic review published in 2010, only 10 cases had been reported since first described by Silberstein,1,4,7 whose diagnoses were made before the patients were pregnant. The average age of diagnosis was 21 years, on a range from 19 to 34 years; most of these cases were diagnosed between 14 and 38 weeks of gestation. Only 2 of the cases showed simultaneous thrombocytopenia and hemolytic anemia. Birth occurred between gestation weeks 32 and 40 and it was vaginal in 7 out of the 10 cases; 8 out of 10 products were born alive; one of the newborns suffered from hemolytic anemia until 2 months after delivery.5.7
The 10 women received prednisone during their pregnancy, at doses between 10 and 80 mg per day; four responded satisfactorily, three did so when intravenous gamma globulin (400 mg/day/kg during 2-3 days) was added, one received anti D globulin during 3 days with no response, another one underwent an splenectomy during pregnancy 9 and the other one after pregnancy.8,10 In this case’s patient, the medical condition did not recede until Azathioprine was prescribed.
The differential diagnosis of Evans syndrome in pregnancy includes mainly microangiopathic hemolytic anemia, such as the one observed in HELLP syndrome and in rare cases in idiopathic thrombocytopenic purpura, or in the hemolytic uremic syndrome, in both of these cases, the Coombs is negative.9, 10
The diagnosis for Evans is performed as a result of laboratory findings of anemia and thrombocytopenia with polychromasia, macrocytosis, spherocytosis, normal reticulocyte count, increased indirect bilirubin and decreased haptoglobulin.11 Most patients require treatment with corticosteroids, but in resistant or recurrent cases, treatment with intravenous γ-globulin, danazol, cyclophosphamide, vinca alkaloids and azathioprine; or even plasmapheresis or splenectomy, might be neccesary.11, 12
In the literature, the treatment to be chosen during pregnancy is based on corticosteroids and IVIG.11 Azathioprine has proven to be safe during pregnancy and lactation.
Laparoscopic splenectomy is considered acceptable in patients with refractory Evans syndrome after the second trimester of pregnancy.10,11 Forceps or vacuum extractor delivery is contraindicated; cesarean delivery only if preceded by obstetric recommendation.11, 12
Although autoimmune thrombocytopenia during pregnancy can
cause moderate or severe fetal thrombocytopenia,
in this case the only manifestation in the product is a moderate
neutropenia
at 40 days old.
References
1. LefKou, Elefdehtheria. Evans syndrome in pregnancy: a systematic literature reviews a two view cases. Eur J Obstet Gynecol Reprod Biol. 2010; 149: 10-17. [ Links ]
2. Evans, RS. Primary thrombocytopenic purpura and acquired hemolytic anemia: evidence for common etiology. Arch Intern Med 1951; 87:48– 65. [ Links ]
3. Silberstein MN, Aaro LA. Evans syndrome and pregnancy. Am J Med Sci. 1966; 252; 206-11. [ Links ]
4. Vorapong, Phupong. Evans syndrome and pregnancy: a case report an International. J Obstet Gynecol. 2004; 111:274 –276. [ Links ]
5. Savasan S, Warrier I The spectrum of Evans’ syndrome. Arch Dis Child. 1997; 77: 245–248. [ Links ]
6. Selcuk Tuncer Z, Buyukasik Y. et al. Pregnancy complicated by Evan’s syndrome. Eur J Obstet Gynecol Reprod Biol 2001; 100:100-101. [ Links ]
7. Sherke RR, Rao MS. Anaesthetic management of splenectomy in Evan’s syndrome during pregnancy with pregnancy induced hypertension. J Postgrad Med. 2001; 47:196-198. [ Links ]
8. Z. Selçuk, Tuncera. Gestación complicada por el síndrome de Evans. Eur J Obstet Gynecol Reprod Biol 2002; 2: 120-122. [ Links ]
9. Passi, Gr. Isoinmunehemolisis in an infant due to maternal Evans síndrome. Indian J Pediatrics 1997; 64: 893-5. [ Links ]
10. Sherrke RR, Rao Ms. Anaesthetic management of splenectomy in Evans syndrome during pregnancy with pregnancy induced hypertension. J Postgrad Med 2001; 47:196-8. [ Links ]
11. Boren TReyes C, Montenegro R, Raimer K, Acase of Evans syndrome in pregnancy refractory to primary treatment options. J Matern Fetal Neonatal Med 2007; 20:843-5. [ Links ]
12. Norton A, Roberts I. Management of Evans syndrome. Br J Haematol 2006; 97:125-37. [ Links ]
Abbreviations: DLP, date
of last period; ALI, amniotic liquid index; PRBC, packed red blood
cells; HCG, "Dr. Rafael Calderón Guardia" Hospital. *Contact
information: Pilar Bogantes
Ledezma
Obstetrics
Department, Hospital Dr. Rafael Calderón Guardia, Caja
Costarricense del
Seguro Social [Dr. Rafael Calderón Guardia Hospital, Costa Rican
Social Security
Institution]











 text in
text in 


