Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Acta Médica Costarricense
On-line version ISSN 0001-6002Print version ISSN 0001-6012
Acta méd. costarric vol.53 n.4 San José Dec. 2011
Original
Evaluation of Local Infiltration with Bupivacaine for Pain Management after Partial Bilateral Salpingectomy
(Evaluación de la infiltración local de bupivacaina en el manejo del dolor post salpingectomía parcial bilateral)
Mariella Fajardo-Arcia1, Leonardo Orozco-Saborío2, Gerardo Montiel-Larios3
Abstract
Objective: the efficacy of locally applied bupivacaine for decreesing postoperative pain was evaluated, in patients who underwent mini-laparotomy partial bilateral salpingectomy.
Methods: A total of 100 women, scheduled for surgical sterilization, were randomized to either an intervention group that received 2.5mg of bupivacaine in the mesosalpinx and 2.5 mg in the fallopian tube stump, or a control group that received no intervention. Postoperative pain was measured one and four hours after the procedure, using the visual analogue scale (VAS, 0-10 cm), and the need and quantity of postoperative analgesia was determined. The Student t-test was used to compare averages, and all analyses were made with the Stata 10.0 statistical software, a critical point of 0.05 (p≤ 0.05) was defined as statistically significant.
Results: Scores on the visual analogue scale (VAS cm) for the bupivacaine group were 4.7 and 2.6, compared to 5.3 and 2.6 for the control group, one and four hours after surgery respectively (p> 0.05). Application of bupivacaine significantly reduced the patients´ requests for a second dose of analgesics one hour after surgery (p<0.03). The control group had a greater need to use opioids (n=8) compared to the bupivacaine group (n=1).The application of bupivacaine in the fallopian tube stumps and mesosalpinx at the time of mini-laparotomy surgical sterilization does not produce differences in postoperative pain management, as measured by the visual analogue scale at one and four hours post-surgery.
Conclusions: Application of bupivacaine is effective in reducing the need for analgesics one hour after surgery and reduces the use of opioids.
In developed countries, laparoscopy is performed, based on its safety and effectiveness. However, in developing countries, mini-laparotomy is used because of low available resources, performing 696 procedures in 2006 for example, at the Gynecology Department of the Hospital de las Mujeres in San José, Costa Rica.7
Several studies have been performed to evaluate the improvement of postoperative pain with local anesthetics after partial bilateral salpingectomy. Most of them showed that these anesthetics diminish pain scale scores, besides decreasing the need for postoperative analgesia.8-27 However, most of studies used laparoscopy as the approach method, which is why the objective of this study was to evaluate the efficacy of local bupivacaine infiltration to reduce postoperative pain in patients subject to mini-laparotomy partial bilateral salpingectomy.
Materials and methods
This was designed as a randomized, double blinded, study. Previously being approved by the Institutional Ethics Committee, the Informed Consent was obtained, and 100 patients were enrolled in this study. These patients were women who were programmed for surgical sterilization in the ambulatory surgery program of the Gynecology Department of the Hospital de las Mujeres. The inclusion criteria were: women older than 18 years old and who met the necessary paperwork for surgical sterilization. Women excluded were those with a history of tubal surgery, intra-abdominal adhesions, chronic pelvic pain, psychiatric disorders or mental retardation, and a history of any type of allergic reactions to local anesthetics. This trial´s sample population was chosen based on another study, 28 which determined that 57 women were necessary to detect, with a 95% probability and 90% power, a 25% reduction in the visual analogue scale after 2 hours.
After the acknowledge that with 57 women the above mentioned indicators were obtained, and taking into account the number of groups to be compared in this study, a sample of 100 randomized women was obtained, equally distributed to both treatment groups.
The making of the randomizing list was performed with the aid of computer software, assigning 50 participants to the intervention group and the other 50 to the control group (Figure 1). To hide this assignation, sealed envelopes were used, which were later opened by the operating rooms anesthesiologist once the patient was anesthetized. The participants and physicians who applied the visual analogue scale were blinded to the group assignations (Figure 1).
All proceedings were realized under a general anesthesia standardized regimen. Before anesthetic induction, patients were pre-medicated with 10mg of metoclopramide, 1mg of midazolam and 0.75 micrograms/kg of fentanyl, the latter was used as analgesia.
Standard anesthetic induction was performed with propofol at a 2mg/kg dose, 5mg of atracurium and 100mg of succinylcholine were applied to facilitate endotracheal intubation. All participants were subject to mechanical ventilation, and maintenance of anesthesia was performed with sevoflurane and oxygen. Intraoperative monitoring was made with clinical standards. Anesthesia was stopped at the end of the surgery, and the blocking was not reverted. Modified Pomeroy partial bilateral salpingectomy was the technique used for surgical sterilization. The intervention group received 5 cc of 0.5% bupivacaine (5mg/ml flask presentation) in each Fallopian tube as follows: 2.5 cc in the mesosalpinx and 2.5 cc in the surgical stump. The control group did not receive any drug in the Fallopian tubes.
In the hospital room, the evaluation of the visual analogue scale (VAS, 0-10cm) began after 1 and 4 hours of the surgical intervention.
The applied regimen for those patients who requested analgesia in hospital room was, a 75mg dose of Intramuscular diclofenac was given. If a second request was made, 50mg of subcutaneous tramadol was applied, and in case a third request for analgesia was made, 15mg of subcutaneous morphine was given. Postoperative analgesia was applied by the nursery staff, previously prescribed by a physician and recorded in the patients file, and according to the expressed requirements for each patient. The time of application and the type of analgesia were recorded.
For the data analysis, patients were characterized by estimating the frequencies and proportions for the qualitative variables, and estimating the averages and standard deviations as descriptive measures for the quantitative variables for each group. Characteristics were compared with the Student t-test for the quantitative variables, and with the chi-square test for the qualitative variable distribution between groups.
A comparison of the visual analogue scale between groups after 1 and 4 hours was made, by comparing the averages using the Student t-test. All analyses were made with the Stata 10.0 statistical software, defining a statistically significant critical point of 0.05 (p≤0.05).
Results
From April 1st until September 9th, 2008, a total of 100 participants agreed the Informed Consent.
A total of eleven participants were excluded, seven of them were part of the control group, and their causes were: an urticarial eruption after the anesthetic induction, one patient declined to participate, two patients did not fulfill the anesthetic protocol, and three patients had variations in the surgical technique. For the intervention group, four patients were excluded: one had a bladder lesion, and three had variations in the surgical technique. This resulted in 43 patients in the control group and 46 in the intervention group.
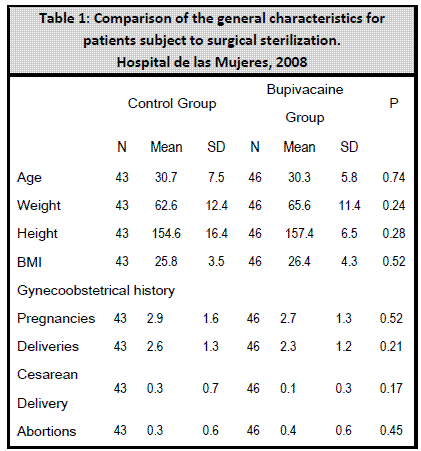
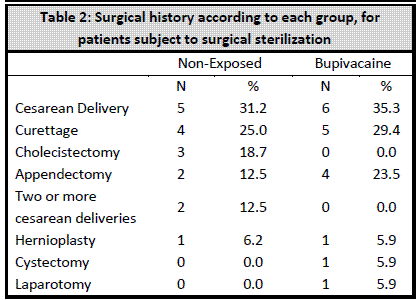
There were no significant differences in the sociodemographic characteristics or clinical history between both groups (Table 1; Table 2). The surgery length was 17.5 ± 6.1 minutes for the bupivacaine group, and 18.5 ± 5.9 for the control group (Table 1 and Table 2).
The VAS score one hour after surgery was 4.7 ± 2.7 for the bupivacaine group and 5.3 ± 3.2 for the control group (p= 0.30). Four hours after surgery, the scores were 2.6 ± 2.2 for the bupivacaine group and 2.6 ± 2.3 for the control group (Figure 2).
An exploratory analysis was made, comparing the VAS for the interventional and control groups one and four hours after surgery for those patients who did not request analgesia after surgery, without finding significant differences: 35.7 ± 24.8 for the intervention group and 38.0 ± 29.8 for the control group after one group (p= 0.79); 23.9 ± 5.3 and 17.2 ± 2.8, after four hours, respectively (p= 0.29). When comparing the magnitude of decrease in the VAS for patients who did not request analgesia, a significant difference was seen for the control group when comparing one to four hours after surgery, 38.0 ± 29.8 and 17.2 ± 2.8 respectively (p= 0.01), not so in the bupivacaine group, 35.7 ± 24.8 after one hour and 23.9 ± 5.3 after four hours (p=0.13).
In the control group, 15.9% of participants requested a second dose of analgesia compared with 2.2% in the bupivacaine group (p< 0.03). Furthermore, the control group had a larger use of opioids (n=8) compared to the bupivacaine group (n=1). No patient needed a third dose of analgesia (Figure 3).
Regarding the elapsed time from surgery to the first dose of analgesia, there was no difference between the groups (p= 0.76). No adverse effects were reported because of the intervention, and intraoperative complications or variations in the surgical technique were not related to the use of bupivacaine.
Discussion
Unlike previous studies; which showed an improvement in pain scales after partial bilateral salpingectomy;10, 28, 30 this study, showed no significant differences in postoperative pain scores (using the visual analogue scale, one and four hours after surgery), after applying bupivacaine in the tubal stumps and mesosalpinx, when performing mini-laparotomy surgical sterilization.
Remarkably, most studies which proved the effectiveness of a local anesthetic had a laparoscopic surgical approach, suggesting that dissection with mini-laparotomy of larger amounts of abdominal wall tissues (during pelvic access), highly influences postoperative pain.
However, applying bupivacaine was effective in reducing the needs for postsurgical analgesia and opioid use one hour after surgery, agreeing with a large number of studies which showed a variable decrease in analgesia consumption and the need for opioids for those patients with a local anesthetic.17-10, 16,17,20 This shows that applying bupivacaine has a short term benefit after surgery, even though it is not reflected in the VAS score, as the control group had a similar reduction in the VAS score to that of the intervention group (Figure 2). This could be explained if pain´s amount, perception or tolerance is differentiated.
There are some limitations for this trial. Firstly, although the applied dose was already used in other studies,7-10 in Costa Rica it is difficult to measure drug concentrations, and it depends only on the surgeon to achieve a homogeneous drug dose. Secondly, the amount of analgesics taken by the participants after discharge was not recorded, because this self-report could represent an increased work for the patient. It might be conceivable that there was a difference in the amount of analgesia taken between both groups. However, since patients with more pain would take more analgesics, the difference in pain levels should decrease instead of growing, and it would not be ethical to deny analgesia to a person in pain.
In conclusion, the fact that mini-laparotomy partial bilateral salpingectomy is an ambulatory procedure and that in some cases patients are not discharged due to pain, it is extremely important to seek for an improvement in postoperative pain relief. The use of bupivacaine by this surgical approach does not seem to benefit the achievement of this goal. However, it seems effective for diminishing the need for postoperative analgesia and the use of opioids.
The short effect duration of this treatment could postpone, but not eliminate the need for other analgesics; therefore bupivacaine should be seen as an add-on to therapy, not as a replacement of traditional analgesic therapy.
Acknowledgements
To the Anesthesia
department of HOMACE, especially to Dr. Leonardo Barquero, Dr. Doris
Sánchez
and Lic. Sara Campos for cooperating with this study.
References
1. Limpaphayom K. Sterilization. Curr Opin Obstet Gynecol 1991; 3: 501-509. [ Links ]
2. World Health Organization. Contraceptive use and commodity cost of female sterilization. What health workers need to know. WHO/ FHE/ FPP 1994;94.2. [ Links ]
3. World Health Organization, Task Force on Female Sterilization, Special programmed of Research, Development and Research Training in Human Reproduction. Minilaparotomy or laparoscopy for sterilization. Am J Obstet Gynecol 1982;143:645-652. [ Links ]
4. Wheeless CR. Outpatient laparoscope sterilization under local anesthesia. Obstet Gynecol 1972; 39:767-770. [ Links ]
5. Osathanondh V. Suprapubic mini-laparotomy, uterine elevation technique: simple, inexpensive and out-patient procedure for interval female sterilization. Contraception 1974;10:251-262. [ Links ]
6. Uchida H. Uchidatubalsterilization. Am J ObstetGynecol 1975; 121:153-158. [ Links ]
7. Centro de estadística del Hospital de la Mujer Adolfo Carit Eva, San José Costa Rica. [ Links ]
8. Van Ee R, Hemrika DJ, de Blok S. Effects of ketoprofen and mesosalpinx infiltration on postoperative pain afeter laparoscopic sterilization. Obstet Gynecol 1996; 88: 568-72. [ Links ]
9. Alexander CD, Wetchler BV, Thompson RE. Bupivacaína infiltration of the mesosalpinx in ambulatory surgical laparoscopic tubal sterilization. Can J Anaesth 1987; 34: 362-5 [ Links ]
10. Kaplan P, Freund R, Squires J, Herz M. Control of immediate postoperative pain with topical bupivacaine hydrochloride for laparoscopic Falope ring tubal ligation. Obstet Gynecol 1990: 798-802 [ Links ]
11. Smith BE, MAcPherson GH, de Jorge M, Griffith JM. Rectus sheath and mesosalpinx block for laparoscopic sterilization. Anaesthesia 1991; 46:875-7 [ Links ]
12. Wheatley SA, Millar JM, Jadad AR. Reduction of pain afeter laparoscopic sterilization with local bupivacaine: a randomized, parallel, double- blind trial. Br J Obstet Gynaecol 1994; 101: 443-6 [ Links ]
13. Tool Al, Kammerer-Doak DN, Nguyen CM. Posoperative pain relief following laparscopic tubal sterilization with silastic bands. Obstet Gynecol 1997; 90: 731-4 [ Links ]
14. Koetsawang S, Srisupandit S, Apimas SJ, Champion CB. A comparative study of topical anesthesia for laparoscopic sterilization with the use of tubal ring. Am J Obstet Gynecol 1984; 150: 931- 3. [ Links ]
15. Barclay K, Calvert JP, Catling. Analgesia after laparocopic sterilization. Effect of 2% lignocaine gel applied to Filshie clips. Anaesthesia 1994; 49: 68-70. [ Links ]
16. Ezed UO, Shoulder VS, Martin JF. Local anaesthetic on doubled- blind controlled trial. Lancet 1995; 346:82-5 [ Links ]
17. Fiddes TM, Williams HW. Herbison GP. Evaluation of postoperative analgesia following laparoscopic application of Filshie clips.Br J Obstet Gynecol 1996; 103:1143-7. [ Links ]
18. McKenzie R, Phitayokorn P, Uy NTL. Topical etidocaine during laparoscopic tubal occlusion for postoperative pain relief. Obstet Gynecol 1986; 67:447-9 [ Links ]
19. Baram D, Smith C, Stinson S. Intraoperative topical etiodocaine for reducing postoperative pain after laparoscopic tubal ligation. J Reprod Med 1990; 35:407-10 [ Links ]
20. Loughney AD, Sarma V, Ryall EA. Intraperitoneal bupivacaine for the relief of pain following day case laparoscopy. Br J Obstet Gynaecol 1994; 101: 449-51. [ Links ]
21. Benhamou D, Narchi P, Mazoit JX, Fernandez H. Postoperative pain after local anesthesics for laparoscopic sterilization. Obstet Gynecol 1994; 84:877-80. [ Links ]
22. Callesen T, Hijort D, Mogensen T. Combined field block and i.p. instillation for pain management after laparoscopic sterilization. Br J Anaesth 1999; 82: 586-90. [ Links ]
23. Mohammed E, Lahsae M, Alborzi S, Vafaei H, Heinrich E. Comparative, double- blind, randomized, placebo-controlled trail of intraperitoneal of bupivacaine and lidocaine for pain control after diagnostic laparoscopy. J Am AssocGynecollaparosc 2003; 10:311-315 [ Links ]
24. Hunter A, Fogarty P. Transcervical analgesia for laparoscopic sterilization. Br J Obst Gynecol. 1996, 103: 378-380 [ Links ]
25. Luscombe FE, Puonder D, Geraghty AV, Bevan JR. Percevicalintrafallopian bupivacaine instillation to reduce postoperative pain after laparoscopic tubal sterilization. Journal of Obstetrics and Gynaecology. 1989, 10: 145-148 [ Links ]
26. Wheatley SA, Millar JM, Jadad AR. Reduction of pain after laparoscopic sterilization with local bupivacaine: randomized, parallel, double-blind trial. British Journal of obstetrics and gynecology 1994; vol 101, 5:443-446 [ Links ]
27. Visalyaputra S, Lertakyamanee J, Pethpaisit N, SomprakitP, Parakkamodom S, Suwanapeum P. Intraperitoneallidocaine decreases intraoperative pain during postpartum tubal ligation. AnesthAnalg 1999; 88:1077-80. [ Links ]
28. Kelly MC. An assessment of the value of intraperitoneal bupivacaine for analgesia after laparoscopic sterilization. BJOG 1996, 103: 837-839. [ Links ]
29. Dionne RA, Khan AA, Gordon SM. Analgesia and COX-2 inhibition. Clin Exp Rheumatol 2001; 19(6 Suppl 25):S63-70. [ Links ]
30. Knight YE, Goadsby PJ. The periaqueductal grey matter modulates trigeminovascular input: a role in migraine? Neuroscience 2001; 106:793-800. [ Links ]
31. Ashpal K, Fisher K, Chabot J, Coderre TJ. Differential effects of NMDA and group I mGluR antagonists on both nociception and spinal cord protein kinase C traslocation in the formalin test and a model of neuropathic pain in rats. Clin J Pain 2001; 17:178-86. [ Links ]
32. Eastwood JD. The folly of effort: ironic effects in the mental control of pain. Int J ClinExpHypn 1998; 46 :19. [ Links ]
33. Fillingim RB, Maixner W, Kincaid S, Sigurdsson A, Harris MB. Pain sensitivity in patients with temporomandibular disorders: relationship to clinical and psychosocial factors. Clin J Pain 1996; 12:260-9. [ Links ]
34. Field HC. Brainsterm control of spinal pain trasmissor neurons. Ann Rev Physiol 1978;40:217-48. [ Links ]
35. Fillingim RB. Sex differences in temporal summation but not sensory-discriminative processing of thermal pain. Pain 1998; 75:121-7. [ Links ]
36. Foster NE, Baxter F, Walsh D, Baxter GD, Allen JM. Manipulation of transcutaneous electrical nerve stimulation variables has no effect on two models of experimental pain in humans. Clin J Pain 1996; 12:301-10. [ Links ]
37. Stanik-Hutt JA, Soeken KL, Belcher AE, Fontaine DK, Gift AG. Pain experiences of traumatically injured patients in a critical care setting. Am J Crit Care 2001;10 :252-9. [ Links ]
38. Fredman B, Jedeikin R, Olsfanger D, Flor P, Gruzman A. Residual pneumoperitoneum: a cause of postoperative pain after laparoscopic cholecystectomy. Anesth Analg 1994;79: 152–4. [ Links ]
1.
Gynecology and
Obstetrics Resident. Hospital
de las Mujeres Dr. Adolfo Carit Eva (HOMACE). 2.
Gynecologist, HOMACE. 3. Chief of
the Gynecology Department,
HOMACE. CCSS.
Hospital
de las Mujeres Dr. Adolfo Carit Eva. Gynecology Department. Clinical
Investigation
Unit, Hospital de las Mujeres, Dr. Adolfo Carit Eva. *Correspondence:
Leonardo
Orozco
S. P.O. Box 11619-1000. San José, Costa Rica E-mail: loscr@yahoo.com











 text in
text in