Introduction
In the last decade HIV/AIDS in- cidence and prevalence have diminished, with about 36.9 million people living with HIV/AIDS (PL- WHA) worldwide (UNAIDS; 2016) (UNAIDS; 2015). Reports from the European Union showed a stable incidence trend of HIV from 2011 to 2015, with approximately 30000 new cases per year (Pharris, A; et ál.; 2015).
In Chile, the annual prevalence rate increased, between 2010 (21.4 cases for every 100.000 persons ≥13 years old) and 2015 (27.7 cases for every 100.000 persons ≥13 years old). The most vulnerable group was within the adults between 20 and 29 years of age, with a prevalence of infection of 40.4% (Instituto de Salud Pública; 2016). Another study showed that between 2008 and 2012, adolescents between 15 and 19 years of age, presented a 72% incidence of HIV notification (Departamento de Epidemiología; 2015). Overall, the statistics report- ed for the Chilean population are not promising.
To eliminate this overwhelming number of cases, nations have in- cluded guidelines that symbolize the commitment to eliminate this virus worldwide. At the core of these programs is the 2011-2015 guide for health sectors developed by the World Health Organization (WHO) Global Strategies (World Health Organization, 2011). In 2005 Chilean public policies were de- creed to provide access and availa- bility to HIV testing, accompanied with counseling and treatment for HIV carriers (Departamento de Asesoría Jurídica; 2005) (Ministerio de Salud de Chile; 2013). Likewise, laws have been slowly implemented in several countries to help eliminate the discrimination and stigma associated with carrying this virus.
Stigma is the result of attitudes, acknowledged or not, that is of- ten derived from misinformation (Foreman, M; Lyra, P; Breinbauer, C; 2003). Literature related to attitudes and knowledge of health professionals and PLWHA is increasing. In the last decade, articles in this topic have covered many aspects. For example, some articles aim to identify factors, such as attitudes, that affect adherence to treatment; others to evaluate how it affects the willingness of health professionals to treat; and some to focus on strategies that PLWHA use to manage negative attitudes towards them ( Lam, Y; et al.; 2016) (Lee, C; et al; 2017) (Brisdon, A; Abel, G; Desrosiers, J; 2017). Never- theless, there are still regions in the world where studies in this topic are still scarce (Conejeros Vallejos, I; et al.; 2010).
In Chile the studies assessing the dimensions of knowledge and at- titudes in health professionals is limited (Ferrer, L; et al. 2015) (Irar- rázabal, LP; 2016) (Rivas, E; 2009). This study contributes to the literature by providing a description of the attitudes and knowledge of health professionals, which can act as barriers or facilitators in the treatment of PLWHA.
Methods
In this cross sectional study, the first inclusion criteria was to be a health professional or technician such as physicians, dentists, midwives, nurses, medical technologists or nurse technicians. They also had to work in the West Metropolitan Health Service health centers (SSMOcc) in Santiago, Chile. This Heath Service has approximately 70 health centers, including hospitals, specialty centers, emergency care and primary health care centers.
To assess attitudes and knowledge of health professionals, the research team used a survey that evaluated the dimensions of HIV prevention, transmission and treatment knowledge, and attitudes towards treating PLWHA. The survey covered the most relevant topics as stated by the available literature, the opinions of experts, and the re- searchers’ knowledge on the topic. Once the survey was tested and retested with researchers and experts in the field it was showed to the target population and their opinion was taken into account regarding the questions and answers categories (Converse, J; Presser, S; 1996). Lastly, the instrument reliability and internal consistency analysis was evaluated using Cronbach’s al- pha calculation. Considering mini- mum acceptable Cronbach’s alpha 0.7 and the maximum expected value of 0.90 (Oviedo Celina, H; Campo-Arias, A; 2005).
Researchers used the following data collection process: 1) Firstly, they contacted the directors of each health center via email, they disclosed the nature of the study and explained that it counted with the ethics committee approval. In the email body, the researchers asked for a contact list of all health professionals that met the inclusion criteria. 2) If the email was not answered in 7 days, a researcher from the team would call the director to verbally ask for the information and resolve any concerns he/ she might had about the study. 3) All contact information was gathered in an excel file with password.
4) Then an email was sent to health professionals (n=719) inviting them to participate in the online survey that the researchers had created. To access the survey all participants had to previously read and agree to an informed consent document. 5) Two reminder emails were sent to the participants during the same month. Directors and healthcare professionals were re- minded that at all times their participation was voluntary and their answers anonymous. The ethics committee of SSMOcc approved this research study.
A descriptive analysis with its correspondent frequency tables and graphs was done in order to show the distribution of the variables associated with attitudes and knowl- edge.
Results
The response rate was 32.7% (n=235). Of these, 23 participants did not meet the inclusion criteria and were excluded of the study, obtaining a final sample of 212 par ticipants.
The survey started with back- ground questions of the partic- ipants, then there was a section that inquired about their attitude and knowledge about HIV. This second segment showed moderate reliability (Cronbach Alpha=0,615), and no changes were made to the survey.
Nursing technicians were the most practiced health providers among the responders (27.4%; n=58), con- trary to the nurse professionals (12.3%; n=26) that were the least. Of the participants, 42.9% (n=91) had practiced their profession for less than 5 years, 23.6% (n=50) from 6 to 10 years, and 21.7% (n=46) for more than 16 years. Most of the health professionals indicated that they had treated PLWHA; 73% (n=155) recorded this experience while working in the public health system, 26% (n=55) in a private clinic, and 1% (n=2) in a private practice. Also, it is important to mention, that 92.5% (n=196) had not received any HIV related training during the last 6 months.
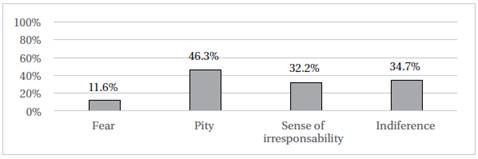
When evaluating attitudes towards treatment of PLWHA, one out of 10 participants declared to feel fear, and 1 out of 3 participants thought that PLWHA were irresponsible people (Figure 1). 90.6% (n=192) declared their disagreement with the statement “I should be able to refuse to attend [PLWHA]”.
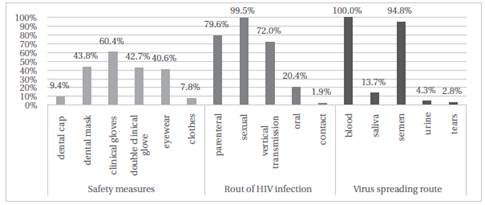
Regarding HIV related knowledge, wearing gloves (60.4%) and masks (43.8%) were correctly identified as protective measures for universal care (Figure 2). A 100% of the re- spondents identified that the HIV virus can spread through blood and fluids, and 94.8% said through semen; 99.5% identified sexual transmission as a route of HIV infection; and 49.5% (n=105) knew referral centers, within their health network that offered treatment to PLWHA.
On the other hand, 52.4% (n=111) of the respondents did not know the clinical guidelines of the Chilean Ministry of Health; 66% (n=140) believed that strategies for diagnosis and prevention are age dependent; 1.9% stipulated that HIV can be transmitted by physical contact; and 2.8% by tears and 4.3% by urine. Finally, 42.7% of the participants indicated that using double glove works as barrier in case of contagion with a sharp object.
Discussion
In Chile, the third chapter of the 17.779 law, states that no public or private health center may deny admission or care to people infected with HIV, or condition their attention to a preliminary examination (Departamento de Asesoría Jurídica, 2005). Four years after the implementation of this law a group of researchers evaluated the knowledge of a group of health professionals in this topic. They conducted a quasi-experimental study with a control and an educational intervention group. The initial evaluation showed poor results that varied between 16,3% in knowledge about the existence of this law to 44.7% of knowledge about the implementation it in their health field. The educational intervention group which received eight face-to-face learning sessions demonstrated having a significantly higher knowledge about the HIV bill than the control group (Ferrer, L; et al.;2011). Our study showed that health professionals also had limited knowledge in other topics related to HIV such as the use of double gloves as a protection health measure. This action alone could make people feel discriminated; therefore, it is necessary to develop a set of educational training tools, like the one used by Ferrer et al, to improve knowledge in HIV and other threatening virus such as Hepatitis B.
Studies show that 69% to 87% of PLWHA do not disclose their status to their health care provider, because they fear discrimination or rejection (Mayfield Arnold, E; et al; 2008).Fear can act as a barrier for seeking healthcare, and could be increased if the healthcare professional showed restraint as well. In the present study, fear and willingness to attend PLWHA had low percentages; nevertheless, low percentages are insufficient, the healthcare system should aim to have a zero discrimination.
It is noteworthy that 92.5% of participants had not received any training or update in general knowledge about HIV during the last six months. Even though the availability of training tools has increased with time, there still is disinformation of HIV in a large sec- tor of society, including the health system (Herrera, C; et al;2008). Especially considering, that in Chile there was a 72.6% raise in the number of HIV confirmed cases between 2010 and 2015 (Instituto de Salud Pública, 2016). Other topics that should be covered during the training are the national clinical guidelines of care and indications for referral centers for treatment. The knowledge of HIV treatment and prevention is of extreme importance for every health professional and technician. The goal being that the treatment provided complies with international stand- ards, and has high levels of adherence and efficacy.
A limitation in this study was that participants were mainly employees from the public health system. The strength is that this is the first study to provide a basic layout of the knowledge and attitude of health professionals towards treatment of PLWHA in Santiago, Chile. Future research studies should aim to determine the gaps in knowl- edge of health professionals in order to develop interventions and training courses and evaluate them. Also, research at a national level is needed to evaluate stigma- tization and discrimination at a healthcare level.