Daily, clinicians strive for the most predictable and safe treatments for their patients by selecting interventions with strong scientific evidence, using the best available techniques/materials and offering a pleasant and relaxing environment in their clinics. By considering all these variables, most certainly the patient’s acceptance of the treatment will be positive and clinical success is almost guaranteed; obtaining satisfied patients and proud clinicians. Still, in some cases an external “factor” may jeopardize this outcome, and a happy ending turns uncertain. This “factor” sometimes refers to the subjective interpretation and expectations of the patient. Patients’ needs share similar characteristics than can usually be measured and managed with standardize procedures. Nonetheless, how patients interpret a clinical procedure that we perform and what expectation they may have for this procedure, are unique for each individual and greatly influenced by their own previous experiences and second hand information. That is why, to define a common term such as “pain” results in a compilation of several individual experiences that will never fit to a standard concept. This article summarizes the importance of recognizing nocebo and placebo effects in dental practice; and how these might impact a dental treatment.
WHAT IS THE DIFFERENCE BETWEEN NOCEBO AND PLACEBO EFFECTS?
Both nocebo and placebo effects are psycho- neurobiological effects influenced by conscious and unconscious factors (1). Although there is no clear definition for these phenomena; in general, placebo/nocebo effects are psychobiological events attributable to certain therapy; being placebo the beneficial response to an inert substance and nocebo the induction of harm caused by an inactive substance (2). Referring to a mere antagonist response, Glick refers to nocebo effect as the “evil twin” of placebo; and refers to both responses as expectation effects (3).
BIOLOGICAL PROCESSES INVOLVED
The placebo/nocebo phenomena have been described in several medical conditions, across different drug classes, and even more significantly in non-pharmacological contexts. As an example, the placebo response to achieve an analgesic effect, has been associated with the release of endogenous opioids (such as endorphins and dopamine), which provide a neurochemical explanation of the effect (4). Early evidence of augmented levels of endogenous opioids present in placebo analgesia was reported by Levine et al, when treating dental postoperative pain and reversing this effect by administering the opiate antagonist naloxone (5).
Placebo/nocebo responses occur within a synergy of psychological and physiological variables widely influenced by different individual and contextual factors. This amalgamation of variables and factors are critical for obtaining a response (positive or negative) and each clinical circumstance around a placebo/nocebo effect must be individually analyzed. Specifically, the factors related to the patient and to the clinician-patient relationship must be weighted individually to assess their impact in the patient response to certain treatment (4).
HOW THE CLINICIANS CAN BENEFIT FROM ENHANCING PLACEBOS?
Ethically, a clinician should not use a placebo intervention as the only therapy to treat a suffering patient, considering that a placebo could influence signs and symptoms of a clinical condition, but does not offer a “real” cure (3). Therefore, considering the use of a placebo as the only intervention to a condition or illness, will deliberately deprive the patient to access the required treatment. Yet, to enhance a clinical intervention with the combination of a possible placebo effect is not only beneficial but recommended. A mere educative and motivational explanation or the use of innocuous approaches that bring an emotional support (6), such as music therapy or aromatherapy, could help clinicians improve the patient’s response to a certain treatment. Even when some of these alternative treatments (such as holistic medicine or homeopathy) lack of adequate scientific evidence supporting a biological plausibility, for some patients and based on previous positive experiences, the beneficial effect could certainly be obtained. As always when recommending any therapy, the treating clinician is responsible for carefully analyzing if this “personal aid” is really innocuous or if it could interfere with the actual treatment and must always try to avoid possible side-reactions. For example, some medicinal plants or natural treatments may not always be as safe as a patient might think. Also, not all alternative treatments that may seem beneficial for one patient will show the same effect in another patient and this is why the communication between the clinician and the patient must be straight and open. This last issue remind us that experiences (bad or positive) can be shared, but the individual interpretation of a certain situation will always be different.
HOW THE NOCEBO PHENOMENON MAY JEOPARDIZE THE DENTAL TREATMENT?
Negative expectations about a treatment are usually composed of basic psychological mechanisms and may induce a nocebo effect on a
patient. Anticipation of information about negative outcomes, prior lack of therapeutic effectiveness, and observation or verbal suggestion about other patient’s bad experiences in the dental office, may trigger physiological changes that could consequently affect the perception, efficacy and even the outcome of a certain therapeutic intervention (7). This phenomenon is especially probable in the dental setting as, simply the context of attending a dental appointment or sitting on the dental chair, may imply a series of multifaceted psychosocial dimensions with powerful therapeutic effects, which could influence the patient’s reactions to a simple procedure. Not to mention that all this situation could be worsened simply by the presence of pain. Catastrophizing, a relevant psychological factor for pain management therapies, is an undesirable occurrence which have the potential of generating nocebo effects in dental patients. When treating patients with pain, factors such as anxiety, helplessness, pessimism, and fear of pain must be addressed by the clinicians in order to prevent a nocebo effect on their treatments (8,9). In recent years, when access to information (true or false) is literally “in our hands” thanks to intelligent mobile phones and portable computers, the clinicians must be ready to manage misinformation and self- interpreted medical data from unknown sources, that may induce new nocebo effects. Under these terms, education must be the most important resource to fight this problem.
CLINICAL MANAGEMENT
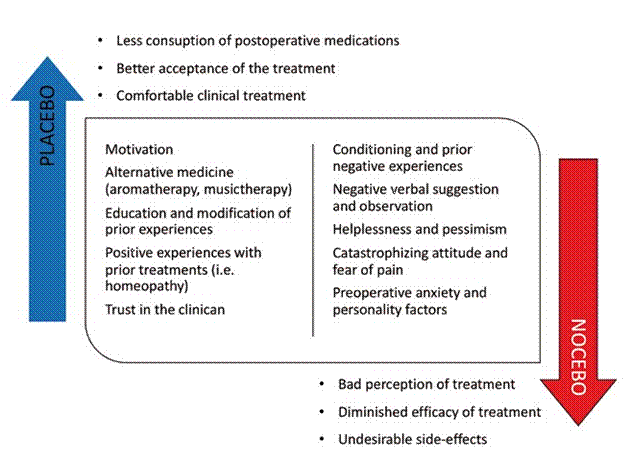
Figure 1 describes the possible nocebo/ placebo balance that might be present during a regular dental appointment. It is of outmost importance that the clinician understands this balance in order to suppress such negative factors preventing the setting of a nocebo effect; and to recognize and enhance personal placebos. Webster et al, suggested that clinicians seeking to reduce the undesirable side effects induced by any nocebo effect associated with their interventions, must try to identify the real patient expectations of the possible adverse effects of the intervention. Also, clinicians could avoid giving suggestions of side effects associated with the intervention to reduce the patient’s exposure to side effects experienced by others (10). This recommendation rises a significant ethical dilemma about the amount of information that clinicians should provide to their patients. The process of informed consent is fundamental and is instituted so that the patient’s autonomy is assured when receiving any treatment. Restricting the information that is being provided to a patient, even when it is done with honest intentions to prevent triggering a possible nocebo effect, is still not suggested and future research should focus on developing innovative ways to reduce nocebo effects that does not require withholding vital information about possible side effects of dental treatments. A practical approach to minimize nocebo effects while still maintaining patient’s independence has been proposed through a “contextualized informed consent” (11). In this model, the amount of information given to a patient is tailored in a way that it will reduce the expectancy of induced side effects while preserving the patient’s right to be informed. These processes must be carefully accomplished with a medico-legal background.
Clinical management of the nocebo effect must include the recognition by both the clinician and the patient of the present phenomenon. Once this has been discussed and the patient personality type has been identified, shaping patient’s expectations to therapy must be attained (11). A suggested method is placing more emphasis on bringing the patient’s attention to the benefits rather than the losses. One example for this management in a dental clinical setting, is when while discussing a necessary invasive treatment and the clinician mentions the need of local anesthesia. Instead of focusing on the pain generated by the needle, the clinician must highlight the benefits of not feeling any pain or discomfort during the clinical procedure and the probable benefit of giving enough time to post-operative medication to work by the time the anesthetic effect wears out. If the patient had previous negative experiences with needles, the clinician must avoid the visual exposure of the syringe and may try to employ any kind of distraction during the injection process. This approach and the enhancement of certain placebo interventions (such as overestimation of topical anesthetic spray for example) may be positive for this specific patient.
In conclusion, placebo/nocebo effects will always be present during the therapeutic process and may positively or negatively impact the treatment effects. Appropriate measures must be taken by all clinical staff in order to find the balance between boosting a positive placebo effect that may contribute to the outcome of the clinical treatment and suppressing the factors which may induce a nocebo effect in a patient. Finding such balance, will finally generate a positive impression in the patient as the clinician could be certain that the best treatment has been provided. When considering the nocebo/placebo balance, the individualization of each treatment is crucial.