Introduction
Gingivitis associated with plaque accumulation is the most common form of the periodontal diseases. It is defined as inflammation of the gingiva in the absence of clinical attachment loss and occurs in the presence of dental plaque 1.
Susceptibility to develop gingival inflammation impacts 100% of the population at some point in their lives 2), (3. Gingivitis presents with specific clinical features such as erythema, edema, change in contour and consistency of the gingival tissue and bleeding upon probing with no radiographic evidence of crestal bone loss 1.
Gingivitis can present in early childhood 4. Hugoson et al.5 reported that prevalence of gingivitis increases with age and is of the order of 95% in populations over 30 years of age. Zhang et al.6 reported a prevalence of 97.9% in the Chinese adult population, meanwhile De Vizio et al.7 reported a 93.9% prevalence in the American adult population.
Plaque induced gingivitis is reversible with appropriate treatment; however, when not treated it becomes a risk factor for periodontitis 3), (8.
Latin America is a heterogeneous region in which epidemiological information regarding gingivitis is scarce 9. The great need to obtain information on this subject underlies the purpose of this investigation which was to estimate the prevalence and severity of plaque induced gingivitis in three Latin American cities.
Materials and methods
This cross-sectional multicenter study utilized stratified, multi-stage probability samples of the civilian, non-institutionalized adult populations in three Latin American cities: Great Metropolitan Area-Costa Rica (GAM), Bogota-Colombia (BC) and Mexico City-Mexico (CDMX). Data were collected from June to December 2015.
Following the protocol used in a previous study in three South American cities 10, which based the sample size on gingivitis prevalence reported in other studies of approximately 94%, (average Gingival Index (GI) ≥ 0.5) with a precision rate of 95% and a 2% error, the sample was defined on 550 subjects per city giving a combined total of 1650 subjects.
The protocol was approved by the Ethic Committee of Pontificia Javeriana University, Colombia, University of Costa Rica and National Autonomous University of Mexico.
Subjects were selected based on population registries of each city, according to their last census, and accounting for differences in gender and age.
Inclusion criteria: 1) age ≥18 years; 2) good general health; 3) at least four natural permanent teeth excluding third molars; 4) ability to understand and answer questions.
Exclusion criteria: 1) antibiotics intake at the time of clinical examination or the preceding three months; 2) pregnancy; 3) breast-feeding; 4) coagulation problems; 5) medications that could interfere with the results of the study; 6) fixed orthodontic appliances 7) antibiotic prophylaxis prior to dental examination. Selected subjects signed informed consent forms.
Sample was divided into five groups according to age range (18-19; 20-29; 30-39; 40-49; and ≥50 years of age ).
Examinations were performed by one calibrated examiner per city. After training, duplicate measurements of GI were taken together with the reference examiner (CKR). Reproducibility analysis revealed inter-examiner kappa values greater than 0.75. Questionnaires about medical history and oral hygiene habits were completed.
Clinical assessment included: Recording of missing teeth (excluding third molars, severely worn/damaged teeth and teeth with prosthetic crowns or cervical restorations). Visible plaque was scored at six sites per tooth (mesiobuccal, midbuccal, distobuccal, mesiolingual, midlingual and distolingual): absence of plaque (0), presence of plaque (1). Calculus was registered on the lower anterior teeth on three surfaces per tooth (mesiolingual, midlingual and distolingual): absence of calculus (0), presence of calculus (1). Loe-Silness modified index 11 was used to assess gingival health on six sites per tooth (distobuccal, mesiobuccal, midbuccal, distolingual, mesiolingual and midlingual):
0= Absence of inflammation. Normal gingiva.
1= Mild inflammation: slight change in color and texture. No bleeding on probing.
2=Moderate inflammation: moderate redness, edema, glazing, bleeding on probing
3=Severe inflammation: marked redness and edema, tendency to spontaneous bleeding and/ or ulceration.
Statistical analysis was performed using SPSS22 software. It was conducted via frequency distribution and crossing of variables. Variance analysis was used in means comparison assuming normality and homogeneity of variances; otherwise the Kruskall-Wallis test was used. Analysis of correlation was made through the Pearson coefficient.
Results
Average age was 41.4 years (39.97 in BC, 39.97 in GAM, 44.19 in CDMX), ranging between 18 and 87 years. Gender distribution varied according to population characteristics of each city (p=0.010): 62.5% males and 37.5% females in CDMX; 54% males and 46% females in GAM and 59% males and 41% females in BC. Total sample: 964 males (58.4%) and 686 females (41.6%). Average number of teeth per subject was 24 (22 in BC, 24 in GAM, 24 in CDMX), ranging from 4 to 28.
The overall average gingival index (GI) was 1.36. No statistically significant difference (p>0.05) was found between GAM (1.45) and BC (1.48), but GI in CDMX was significantly lower (1.16). The highest values for GI were associated with molar teeth (1.5 vrs.1.3 for premolars, 1.3 for canines and 1.3 incisors).
Only 3.4% of the subjects had a GI value lower than 0.5, all within CDMX. Moderate gingivitis predominated in the three cities (Table1). In BC, 94.7% of the subjects had moderate gingivitis with no significant difference (p>0.05) between men and women; of the remaining 5.3% (2.7% with mild gingivitis and 2.5% with severe gingivitis) men showed greater severity than women. Moderate gingivitis also predominated in GAM in both genders (96%), but on the remaining 4% (3.6% with mild gingivitis and 0.4% with severe gingivitis) there was a higher percentage of women with a severe form of the disease. CDMX also had a predominance of moderate gingivitis but statistically significantly lower than the other two cities (p=0,0001), with a 61.5% total. Of the remaining 38.5% participants, 3.3% had severe gingivitis, 34% mild gingivitis and 3.4% were healthy. In all cases there were no significant differences by gender (p>0.05). No statistically significant difference was found for age range in any city. However, CDMX showed a higher percentage of mild gingivitis than GAM and BC at all age groups (Table 1).
Average gingival bleeding on probing across the three cities was 43%. In BC the percentage remained constant irrespective of age. In GAM, it lowered as age increased (r=0,0038). CDMX registered significantly less bleeding on probing in every group (p=0,0001), than BC and GAM. Total bleeding on probing in CDMX was 29,2%. Between BC and GAM there was no statistically significant difference (Table 2). A positive correlation was found between gingival bleeding and site location (r=0.954), being significantly higher at interproximal sites (p=0.0001).
Table 3 shows the percentage of individuals with ≥50% bleeding sites by city, age group and gender. From the total sample, 38.5% had 50% or more bleeding sites. As age increased the percentage of subjects with ≥50% bleeding decreased. In terms of city, BC showed the highest percentage of individuals with ≥50% bleeding sites (55.8%) and CDMX the lowest (16.4%). This difference was statistically significant (p=0.0001). On the other hand, there was no statistically significant difference according to gender.
Table 1 Severity of Gingivitis according to Gingival Index per city and age.
| Gingival Index (GI) | |||
|---|---|---|---|
| City | |||
| Bogota City | |||
| 20-29 | |||
| 30-39 | |||
| 40-49 | |||
| ≥50 | |||
| Total | |||
| GAM | |||
| 20-29 | |||
| 30-39 | |||
| 40-49 | |||
| ≥50 | |||
| Total | |||
| CDMX | |||
| 20-29 | |||
| 30-39 | |||
| 40-49 | |||
| ≥50 | |||
| Total | |||
| Total | |||
| 20-29 | |||
| 30-39 | |||
| 40-49 | |||
| 100,00 % | |||
Range: 0.28-2.97 CI: 95%:1.36-1.39
Table 2 Bleeding on probing per age and city.
| Age | |
|---|---|
| N | |
| 18-19 | |
| 20-29 | |
| 30-39 | |
| 40-49 | |
| ≥50 | |
| Total | 1650 |
Significance: 95%
Table 3 Average bleeding by city, age group and gender.
| City Age group (years) | ||
|---|---|---|
| Male | ||
| Average | ||
| Bogota City | ||
| 18-19 | ||
| 20-29 | ||
| 30-39 | ||
| 40-49 | ||
| ≥ 50 | ||
| GAM | ||
| 18-19 | ||
| 20-29 | ||
| 30-39 | ||
| 40-49 | ||
| ≥ 50 | ||
| Mexico City | ||
| 18-19 | ||
| 20-29 | ||
| 30-39 | ||
| 40-49 | ||
| ≥ 50 | ||
| Total | ||
| 18-19 | ||
| 20-29 | ||
| 30-39 | ||
| 40-49 | ||
| ≥ 50 | 0,24 | |
Average plaque index was 76%. Significantly highest accumulations were located at interproximal sites (83%) in contrast to mid areas (59%) (p=0.0001) (Table 4). Maximum plaque deposition was observed in molars and lower central incisors. Minimum plaque accumulations were associated with upper anterior teeth. Across the overall sample a positive correlation was found between the presence of plaque and GI (r=0.59).
Table 4 Plaque Index according to surface and tooth site.
| Tooth Site | |
|---|---|
| Buccal | |
| Distal | |
| Mesial | |
| Mid | |
| Total | 75 , 52 |
Dental calculus was present in at least one of 18 sites evaluated for 98% of the sample, without statistically significant differences (p>0.05) between the three cities (GAM: 97.3%, BC: 99.1%, CDMX: 97.5%). Interproximal sites showed the highest calculus index. In terms of tooth type, canines had the lowest amount of calculus while central incisors had the highest. A statistically significant (p>0.05) positive correlation was found between calculus and gingivitis (r=0.229).
From the total sample, 88% brush their teeth three or more times a day (BC: 92%, GAM: 96.6%, CDMX: 73%), 2.1% brush once per day and 9.9% twice per day. An inverse correlation between tooth brushing and the presence of plaque was found (r=-0.122). Only 6.2% reported using dental floss. No positive correlation was found between presence of plaque and flossing.
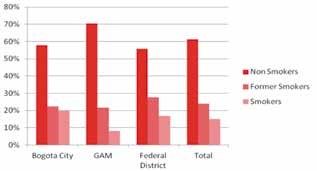
Of the total subjects, 61.3% were nonsmokers, 23.8% former smokers and 14.3% current smokers (Figure 1).
There was no statistically significant difference in GI between smokers, former smoker and non-smokers (p>0.05) (Table 5). Plaque Index was statistically significantly higher in smokers than non-smokers and former smokers (p=0.007). Between non-smokers and former smokers there was no significant difference. This was not reflected by bleeding on probing which had no statistically significant difference between smokers and nonsmokers (p=0.068) (Table 5).
Educational level was not a significant contributing factor in gingivitis (p>0.05) (Table 6).
Table 5 GI, Bleeding on Probing and Plaque Index according to smoking habits.
| Smoking habits | |
| Mean | |
| Gingival Index | |
| Bleeding on probing | |
| Plaque Index | 0 , 15 |
Discussion
Plaque-induced gingivitis is reported as a very common disease amongst the general population. Loe et al.12 showed that, following withdrawal of oral hygiene, 100% of the population develops gingivitis. However, there is a dearth of available information reporting prevalence data for gingivitis in specific populations.
The present study found gingivitis (GI ≥0.5) in 96.6% of subjects from the three Latin American cities analyzed. A previous study following the same protocol in three South American cities, reported a very similar prevalence (95.6%) (10). Both studies confirm that gingivitis is a highly prevalent disease in Latin America. Previous epidemiological studies in China and the USA reported a prevalence of gingivitis of 97.9% and 93.9% respectively (6,7), indicating that gingivitis is a highly prevalent condition regardless of ethnicity.
Moderate gingivitis predominated in the three cities. There was, however, a statistically significant difference in terms of good gingival health between CDMX and the other two cities. In CDMX, almost 40% of the subjects had mild gingivitis and 3.4% had a GI <0.5, suggesting healthy gingiva. In BC and GAM, moderate gingivitis was also the most prevalent condition but in contrast to CDMX, neither had healthy subjects (GI <0.5). A significant positive correlation was found between presence of plaque and GI (r=0.59), confirming that the higher the plaque index, the higher the Gingival Index. This is in accordance with the directly proportional relationship between presence of bacterial plaque and gingival inflammation reported in the literature 1,6,7,12),(13),(14),(15),(16),(17),(18),(19. Analyzing the correlation by city, data reported in BC and GAM coincides with data reported for the total sample. However, CDMX had the lowest GI scores without statistically significant difference in plaque index compared with the other two cities.
No significant associations were found between GI and age group supporting the findings of Winkel et al.20, who concluded that age is of minor importance with regard to plaque accumulation and development of gingival inflammation in individuals not susceptible to periodontal destruction. In the same manner, Nonnenmacher et al.21 found no significant difference for plaque accumulation and gingival inflammation in relation to age.
A higher prevalence of gingivitis has been reported in men compared with women (6, 7, 18). A study of the urban population of Sweden showed that women had better oral hygiene as well as periodontal status than men 22. However, in this study, no gender-related differences in gingival health were seen which agrees with the findings of a previous study in South America 10, highlighting the need to understand gingival health at the level of specific populations.
It´s been widely documented that dental plaque is a direct etiological factor for gingivitis (1, 2, 3, 4, 12, 14, 16, 18, 19) which coincides with results of the present study. It has also been established that removal of plaque from sites with gingivitis results in resolution of soft tissue inflammation (13, 19). This investigation found an overall plaque index of 76%. This contrasts with information provided by the subjects, where 88% claimed to brush their teeth three or more times per day. Previous studies have reported that the majority of subjects brushed twice per day and only a small percentage brush three times or more per day 14. Lowest gingivitis prevalence has been reported among subjects with regular tooth brushing habits 23. Zimmermann et al.24 concluded from their meta-analysis that infrequent tooth brushing is statistically significantly associated with periodontitis. Taking into account the high plaque index amongst subjects, results clear that effectiveness of their tooth brushing and oral hygiene habits were far from ideal. Plaque accumulation was significantly higher at interproximal sites (83%) compared to mid areas (59%). This is in accordance with data published by Theilade 19 and could be explained by the fact that only 6.2% of total subjects in this study floss. Highest plaque scores were associated with molars, perhaps due to difficulties in tooth brushing and accessing posterior sites, especially on teeth with furcation exposure. In contrast, anterior maxillary teeth had the lowest plaque accumulation, presumably due to better and easier access during tooth brushing.
The highest percentage of smokers was reported in BC and the lowest in GAM. It has been reported the negative impact of smoking on periodontal health 25; however, no statistically significant difference was found in GI between smokers, former smokers and non-smokers.
Smokers showed a slightly higher but not statistically significant plaque index than non-smokers. Aligned with this findings, numerous investigations have reported similar plaque accumulation regardless of smoking habits 26), (27), (28. In contrast, some studies have reported greater plaque accumulation in smokers compared with non-smokers
(29, 30,31. There is also controversy in terms of bleeding on probing. This study found no statistically significant difference on bleeding on probing between smokers and non-smokers. Van der Velden et al.26 concluded from his study that there are no differences between smokers and non-smokers in terms of plaque accumulation and gingival bleeding, providing that good oral hygiene is maintained. They also reported that in the presence of plaque, smokers tend to bleed less than non-smokers. According to Calsina et al. 32 this occurs due to reduction in vascular inflammation associated with tobacco-induced vasoconstriction at the gingival level. Absence of bleeding on probing has been regarded as a sign of gingival and periodontal stability 33. Smoking could therefore mask gingival inflammation leading to a false negative diagnosis, as previously suggested by Bergstrom 34.
Previous investigations have reported a higher prevalence of gingival inflammation in subjects with ≤12 years of education compared with those with >12 years of education 10. However, no statistically significant differences in GI were found in this study according to educational level.
Conclusions
Gingivitis prevalence was 99.6%, with moderate gingivitis as the predominant form and no statistically significant differences by city or by gender. Dental plaque accumulation was the most important risk factor associated with the establishment of the disease. The study data underlines the importance of understanding oral health at the geographical population level and provides valuable information on gingival status in Latin America that could help develop programs to benefit oral care in these populations.