Serviços Personalizados
Journal
Artigo
Indicadores
-
 Citado por SciELO
Citado por SciELO -
 Acessos
Acessos
Links relacionados
-
 Similares em
SciELO
Similares em
SciELO
Compartilhar
Acta Médica Costarricense
versão On-line ISSN 0001-6002versão impressa ISSN 0001-6012
Acta méd. costarric vol.63 no.2 San José Abr./Jun. 2021
Brief communication
Radiotherapy in the pediatric oncologic population of Costa Rica: 2-year experience
1 Caja Costarricense de Seguro Social, Hospital Nacional de Niños “Dr. Carlos Sáenz Herrera”, Servicio de Oncología. San José, Costa Rica
Childhood cancer is a rare entity whose incidence is increasing.1 In Costa Rica, pediatric oncology care is centralized, and therefore, according to data recorded in the Hemato-oncology Department of the Hospital Nacional de Niños “Dr. Carlos Sáenz Herrera” (HNN) of the Caja Costarricense de Seguro Social (CCSS), 1,389 new cases of cancer were diagnosed in children under 13 years of age between 2007 and 2016; the most common diagnosis being leukemia, followed by central nervous system (CNS) tumors and, in third place, lymphomas.
Radiation therapy is one of the mainstays in the treatment of some childhood cancers; up to 50% of pediatric patients may require this therapy during the course of their disease. Radiotherapy can be used as a single or combined treatment modality. 2,3
Ionizing radiation therapy has particularities and challenges when applied to children; from the heterogeneity of tumors, the differences inherent to the patient’s age, the varying degrees of maturity, the need for immobilization for adequate and safe treatment, the need for general anesthesia and the psychosocial aspects of the patient and his or her family.1
The curative indication of treatment aims to eliminate the tumor and reduce the risk of recurrence, while the palliative intention aims only to alleviate the symptoms to improve the atient’s quality of life. 3
Linear accelerators are currently the most widely used equipment in external radiation therapy to deliver ionizing radiation, via photons or electrons.
The radiation dose is prescribed in Gray units (Gy), which represent the amount of energy deposited in tissue. The total dose is divided and administered in different sessions; this is known as fractionation. 3-5
Adequate positioning and immobilization of the patient are necessary during the planning and each radiotherapy session to guarantee the effectiveness of the treatment and to avoid toxicity as much as possible.3,4 However, this can be a problem in children, due to their age, maturity, or anxiety level. Children under 3 years of age do not usually lie still for long periods, so they frequently require sedation or general anesthesia during treatments for adequate immobilization. The use of anesthesia adds potential risks and challenges, so it should be performed by an experienced pediatric anesthesiologist, if possible.1,6
There is little information about pediatric radiotherapy in the international literature and, in Costa Rica, there is only one previous study on the subject.7 Waiting times for radiotherapy have increased worldwide and this harms the prognosis and survival of these patients. 8
The objective of this study was to describe the epidemiological, clinical, and therapeutic characteristics of pediatric patients with oncologic diagnoses treated at the Hospital Nacional de Niños “Dr. Carlos Sáenz Herrera” and received external radiotherapy as part of their therapeutic management, during the period from January 1, 2015, to December 31, 2016.
Methods
This is an observational and descriptive study. Information was collected retrospectively from the clinical records of pediatric patients with oncologic diagnoses, who were treated at the HNN and who received radiotherapy, during the period from January 1, 2015, to December 31, 2016.
Data were recorded using a data collection sheet, which included the following study variables: sex, age, type of tumor, anatomical site irradiated, indication for radiotherapy (curative or palliative), need for anesthesia, waiting time for treatment initiation, and reason for the delay in treatment initiation. Cases whose records presented less than 50% of the variables of interest were excluded, as well as cases who did not complete treatment with radiotherapy due to the death of the patient.
The ideal scenario is for patients to start radiotherapy no later than 7 days after the simulation CAT scan; thus, the waiting time was defined as the time elapsed beyond 7 days after the simulation CAT scan. Treatment delay was defined as those cases in which the treating physicians recorded the word “delay” in the file, or if they subjectively considered that the start of radiotherapy had been very prolonged (without following standardized definitions or criteria).
The information was collected in an electronic database created with Epi Data version 3.1. For statistical analysis of the data Stata 14.0 and Excel 2007 software programs were used. For the descriptive analysis of the information, the qualitative variables were organized in simple frequency tables and association or contingency tables. Quantitative variables were analyzed using central tendency and position statistics (minimum, average, maximum, quartiles), and variance statistics (standard deviation).
The study protocol was approved by the Local Bioethics and Research Committee of the HNN, with code CLOBI-HNN-003-2016.
Results
During the period under analysis, 132 pediatric patients were registered with an oncologic diagnosis and received radiotherapy, of whom 124 patients who met the inclusion criteria were included. Of the 124 patients included, 7 patients were subsequently excluded for the following reasons: 4 patients died before completing their radiotherapy treatment, 2 patients completed radiotherapy at a date later than the period under study and 1 patient had an incomplete record. The final population included and analyzed in this study were 117 patients, of whom 69 (59%) were boys and 48 (41%) were girls.
The mean age ± SD of the patients under study was 7.7 ± 3.9 years old, with a range between 1.7 and 16.5 years; 75% of the patients were 11.5 years old or younger. Among female patients mean age was 7.2 ± 4.2 years old with a range between 1.8 and 16.5 years, although 75% were 11.7 years old or younger; meanwhile, the average age of male patients was 8.0 ± 3.5 years old with a range between 1.7 and 15.1 years, and 75% were 11.1 years old or younger.
The most frequently irradiated tumor type was leukemia, with a total of 30 patients (25.6%). In second place was Hodgkin’s lymphoma with 13 patients (11.1%) and, in third place, medulloblastoma with 12 patients (10.3%). However, when grouping CNS tumors in one category, they represent the most c irradiated group of tumors (27.5%), very similar to leukemias.
A total of 138 anatomical sites were reported as irradiated, which is explained by the fact that some patients received radiotherapy in more than one site. The most frequently irradiated anatomic site was the CNS in 40.6% (56 patients), followed by neck in 10.1% (14 patients), abdomen in 10.1% (14 patients) and testicles in 8.0% (11 patients). The pelvis was the least irradiated anatomical site, with only 3 patients (2.2%). Table 1 shows the radiotherapy indication according to tumor type; some tumors can be irradiated with curative or palliative intent, depending on the stage of the disease.
Table 1 Distribution according to tumor type and indication for radiotherapy (curative or palliative) of the 117 patients who received radiotherapy, period January 2015 to December 2019. Department of Hemato-oncology, National Children’s Hospital “Dr. Carlos Sáenz Herrera”, Caja Costarricense del Seguro Social.
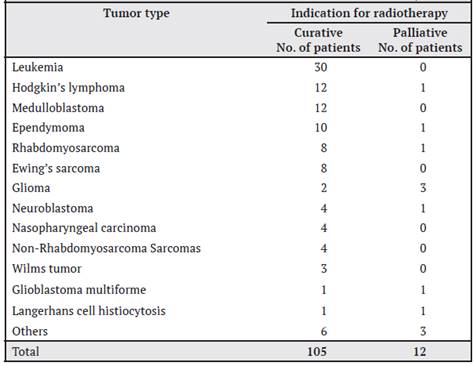
The use of anesthesia during radiotherapy sessions was required in 34 patients (29.1%). The average age of patients who required anesthesia was 4.4 years old ± 3.8 years among female patients and ± 2.9 years among male patients. The age group that required anesthesia the most was the under 4 years of age, representing 23.1% (27 patients) of the population studied.
All patients who received radiotherapy treatment had a waiting time; that is, all patients started radiotherapy beyond 7 days after the simulation CAT. The average waiting time was 30.2 ± 19.0 days, with a range from 6.0 to 101.0 days; for 75% of the patients, this period was 36.0 days or less.
The waiting time for patients who received curative radiotherapy (31.5 ± 19.2 days) was longer than for those who received palliative radiotherapy (15.1 ± 4.4 days) and it was also longer for patients who received anesthesia (33.3 ± 18.9 days) compared with those who did not require anesthesia (29.0 ± 19.0 days).
Concerning the reason for the delay in starting treatment with radiotherapy, the treating physician documented a delay in 23 patients (19.7%), but only in 20 of them was the specific reason noted, no data was found in the records of 3 patients. The causes of delay most frequently documented were non-clinical factors: treatment equipment failure (2 patients), absenteeism to medical appointments (2 patients), absenteeism to the simulation CAT (1 patient), a data error during the initial simulation CAT (1 case), change in radiotherapy modality to a specialized technique (1 patient) and problems with the immobilization mask (4 patients).
The patient’s clinical condition was the cause of delay in 9 patients when it was mentioned as a reason such clinical conditions were: the need for surgical resection of the previous tumor (1 patient), second- line chemotherapy for local tumor control (1 patient), the need for completion of chemotherapy (1 patient), the need for general anesthesia (2 patients), infectious processes (2 patients), non-infectious complications from chemotherapy (1 patient), and complications related to a percutaneous gastrostomy device (1 patient).
Discussion
The population of this study consisted of 117 pediatric patients with an oncologic diagnosis who received radiotherapy as part of their therapeutic management and were treated in the Department of Hemato-oncology of the HNN, at any time during the 2 year study period.
Male patients were the most frequently irradiated, which is to be expected since childhood tumors occur more frequently in men.1,9 Selo et al, studied the adverse effects of ionizing radiation in children under 19 years of age, and 55.9% of their population was male.10 Cerdas and Rodriguez studied irradiated patients under 18 years of age, and also described a predominance of the male sex (59.0%), data similar to those of Ahern. 2,7 Childhood cancer is more frequent in children under 5 years of age;1 this age is lower than the mean obtained in the study (7.7 years), a discrepancy that can be explained by the fact that the study only contemplates irradiated patients and not the totality of oncologic patients. In Ahern’s study, the most irradiated group were patients aged between 10 and 15 years.2 The difference in the results between the studies can be explained by the variability according to the prevalence of pediatric tumors, the treatment protocols, and the age of care in each region or hospital center.
It is to be expected for leukemias and CNS tumors to be the most frequently irradiated malignancies; first, because together they account for about 50% of tumors in children under 14 years of age and second because they are very radiosensitive tumors and include radiotherapy in their treatment protocols. It is also to be expected for the CNS site to be the most irradiated anatomical site since it includes patients diagnosed with brain tumors and leukemias with CNS infiltration. 2,9,11-13
The main indication for radiotherapy treatment was curative (89.7%); results comparable with the literature reviewed, which describes curative radiotherapy in 72-99% of cases, and palliative in 11% of cases.14,15
Almost one-third of all patients analyzed required anesthesia during radiotherapy treatment sessions due to their young age. Several international studies support these findings, as they report that patients who most commonly require anesthesia are those under 5 years of age (especially those under 3 years) and that the older the patient, the lesser the need for anesthesia. 6,16
The waiting times found in the study merit special attention. Although 75% of the patients had waiting times of less than 35 days, some had longer waiting times. Palliative radiotherapy patients had shorter waiting times than curative radiotherapy patients, due to the promptness with which symptoms need to be treated in these patients with limited survival and the lower radiotherapy planning complexity in these cases. 15
The deleterious effect of waiting time for the initiation of radiotherapy in oncologic pathology is well described in adults and could be extrapolated to the pediatric population. Prolonged waiting time favors tumor cell survival and unnecessary tumor growth; this increases the need for higher radiation doses, increases the risk of metastasis, and decreases local disease control and patient survival. 8. In this regard, Liang et al analyzed the effect of waiting times on the survival of patients with nasopharyngeal carcinoma treated with radiotherapy and documented that a waiting time longer than 30 days increases the mortality of these patients. 17
There are studies with models to predict the effects of increased waiting times, as well as others that analyze the contributing factors.18,19 Oberreuter et al. found that the main delays in initiating radiochemotherapy for patients with head and neck tumors were the patient’s delay in consultation, biopsy report and access to treatment. However, they also mention that in some cases there was a delay due to the need to stabilize the patients’ comorbidities or to their post-surgical recovery.19 Despite observing a large underreporting of information on the reasons that may delay the initiation of radiotherapy, when the reason was noted, it was possible to document that for 55% of patients, it was attributed to non-clinical factors of the patient; the importance of this result is that these are potentially correctable factors.
The limitations of the study are related to the retrospective nature of the data collection and the lack of information recorded in the patients’ medical records.
In conclusion, radiotherapy is a treatment modality used in pediatric oncology patients of different ages and both sexes and mainly among cases diagnosed with brain tumors and leukemia. In most cases, it is offered as curative and in some patients, due to their young age, the use of anesthesia may
be required during treatment. In all cases a waiting time for the start of treatment was documented, in most cases, the delay was less than 36 days and in a minority of cases it was documented that the main reason was a non-clinical factor of the patient.
Abbreviations: HNN, Hospital Nacional de Niños; CNS, central nervous system; CAT, Computed axial tomography. Sources of support: There is no external financing, and it did not generate expenses for the Caja Costarricense de Seguro Social. Conflict of interest: The authors declare that they have no conflict of interest. marijo13_an@hotmail.com
Referencias
1. Thorp N. Basic Principles of Paediatric Radiotherapy. Clin Oncol. 2013;25:3-10. [ Links ]
2. Ahern V. Utility of an Australasian registry for children undergoing radiation treatment. J Med Imaging and Radiat Oncol. 2014;58:693-9. [ Links ]
3. Choong ES, Turner RN, Flatley MJ. Radiotherapy: basic principles and technical advances. Orthop Trauma. 2014;28:167-1. [ Links ]
4. Murray LJ, Robinson MH. Radiotherapy: technical aspects. Medicine. 2016;44:10-4. [ Links ]
5. Smith S, Prewett S. Principles of chemotherapy and radiotherapy. Obstet Gynaecol Reprod Med. 2017;27:206-12. [ Links ]
6. Stackhouse C. The use of general anaesthesia in paediatric radiotherapy. Radiography. 2013;19:302-5. [ Links ]
7. Cerdas B, Rodríguez C. Características clínico- epidemiológicas de los pacientes menores de 18 años tratados con acelerador lineal. Acta pediátr costarric. 2014;23:29-35. [ Links ]
8. Bütof R, Baumann M. Time in radiation oncology- keep it short! Radiother Oncol. 2013;106:271-5. [ Links ]
9. Ward E, DeSantis C, Robbins A, Kohler B, Jemal A. Childhood and adolescent cancer statistics, 2014. CA Cancer J Clin. 2014;64:83-103. [ Links ]
10. Selo N, Bölling T, Ernst I, Pape H, Martini C, Rübe C, et al. Acute toxicity profile of radiotherapy in 690 children and adolescents: RiSK data. Radiother Oncol. 2010;97:119-26. [ Links ]
11. Bartlett F, Kortmann R, Saran F. Medulloblastoma. Clin Oncol. 2013;25:36-45. [ Links ]
12. Laprie A, Hu Y, Alapetite C, Carrie C, Habrand JL, Bolle S, et al. Paediatric brain tumours: A review of radiotherapy, state of the art and challenges for the future regarding protontherapy and carbontherapy. Cancer Radiother. 2015;19:775-89. [ Links ]
13. Vaidya K, Smee R, Williams JR. Prognostic factors and treatment options for paediatric ependymomas. Journal of Clinical Neuroscience. 2012;19:1228-35. [ Links ]
14. Rao AD,Chen Q,Ermoian RP,Alcorn SR,Figueiredo MLS, Chen MJ, et al. Practice patterns of palliative radiation therapy in pediatric oncology patients in an international pediatric research consortium. Pediatr Blood Cancer. 2017;64(11):e26589. https://doi.org/10.1002/pbc.26589 [ Links ]
15. Stachelek GC, Terezakis SA, Ermoian R. Palliative radiation oncology in pediatric patients. Ann Palliat Med. 2019;8:285-92. [ Links ]
16. McMullen KP, Hanson T, Bratton J, Johnstone PAS. Parameters of anesthesia/sedation in children receiving radiotherapy. Radiat Oncol. 2015;10:10-3. [ Links ]
17. Liang H, Xiang YQ, Lv X, Xie CQ, Cao SM, Wang L, et al. Survival impact of waiting time for radical radiotherapy in nasopharyngeal carcinoma: A large institution-based cohort study from an endemic area. Eur J Cancer. 2017;73:48-60. [ Links ]
18. Riff MC, Cares JP, Neveu B. RASON: A new approach to the scheduling radiotherapy problem that considers the current waiting times. Expert Syst Applications. 2016;64:287-95. [ Links ]
19. Oberreuter E, Oliva C, Contreras JM, Cardemil F. Análisis de tiempos de espera en pacientes con cáncer de cabeza y cuello en el Hospital San Juan de Dios. Rev. Otorrinolaringol. Cir. Cabeza Cuello. 2017;77:144-9. [ Links ]
Received: October 14, 2020; Accepted: August 19, 2021










 texto em
texto em