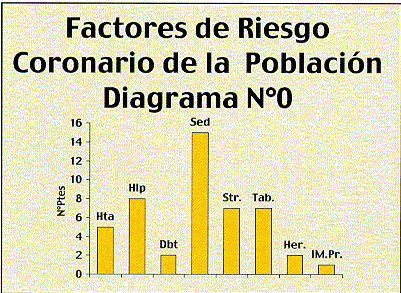
Referencias: Hta: hipertensión arterial, Hlp: hiperlipidemias, Dbt: Diabetes
mellitus, Sed: sedentarismo, Str: estrés, Tab: tabaquismo, Her: herencia
IM.Pr: infarto previo. ]]>
Angioplastía primaria en el manejo del infarto agudo al miocardio, experiencia incial en Panamá
*Dr. Antonio Rodríguez, Dr. Norberto Calzada, Dr. Percy Nuñez, Dr. Daniel Pichel, Dr. Jorge Motta, Dr. Alberto Arrocha.
Resumen
En los últimos años se han redoblado los esfuerzos para disminuir y en el mejor de los casos evitar el daño al músculo cardíaco durante el infarto agudo. Las drogas trombolíticas han contribuido positivamente al respecto. Sin embargo, nace la necesidad de buscar formas alternas de tratamiento que proporcionen un más rápido y efectivo restablecimiento de la circulación coronaria. Nos referimos a la Angioplastía Primaria como tratamiento inicial del infarto agudo. Presentamos los primeros 16 casos con infarto agudo al miocardio en curso, tratados con Angioplastía Primaria, 15 de 16 pacientes evolucionaron en forma satisfactoria, sin complicaciones intra-hospitalarias. Hubo una defunción más directamente relacionada a las complicaciones del infarto que al procedimiento de angioplastía per-se.
]]> De esta manera reafirmamos la utilidad de esta nueva forma de tratamiento, planteando una alternativa terapéutica adicional en beneficio de los pacientes que están sufriendo un infarto agudo al miocardio.Palabras clave
Angioplastía primaria, infarto agudo.
Summary
In the last several years there have been increased efforts to reduce, and in the best of cases to avoid , damage to the cardiac muscle during acute myocardial infarction. Thrombolytic drugs have contributed favorably in that respect. However, there has been the need to find alternative methods of treatment to provide faster and more efective reestablishment of coronary circulation. In this paper we refer to primary coronary angioplasty as initial treatment for acute myocardial infarction. We present our first 16 patients with an evolving acute myocardial infarction treated with primary angioplasty, 15 of the 16 patients had a satisfactory course, without inhospital complications. There was one death more directly related to complications of the infarction rather than to the angioplasty procedure itself.
In this way we reinforce the utility of this new method of treatment, making it an alternative therapeutic option in benefit of patients with an acute myocardial infarction.
Key Words
Primary PTCA, AMI.
En 1912 Herrick ( 1) describió la trombosis coronaria aguda, sin embargo, transcurrió mucho tiempo antes de entender la verdadera fisiopatología de la oclusión coronaria y su papel en la producción del infarto agudo al miocardio.
En las últimas décadas cobra vigor el concepto de la fisura de la placa arterioesclerótica complicada con trombosis sobreagregada como proceso desencadenante de la vasta mayoría de los infartos al miocardio, angina inestable y muerte súbita (2,3,4,5).
En 1980 DeWood y colaboradores (6) demostraron una alta prevalencia de trombosis en la arterias coronarias a las pocas horas de haberse producido un infarto agudo al miocardio.
Este hallazgo realmente produce cambios dramáticos en el tratamiento del infarto agudo al miocardio, dándole un lugar muy justificado a las drogas trombolíticas , las que inicialmente eran empleadas por vía intracoronaria y posteriormente por vía endovenosa (7).
Actualmente mucho es lo aprendido con respecto a ellas: tipos , dosificación, complicaciones, potencia fibrinolítica etc.
Los grandes estudios multicéntricos con estas drogas, enfatizan cada vez más lo importante y crucial de la reperfusión temprana y su positivo impacto en la reducción del tamaño del infarto (8) y en la mortalidad cardiovascular (9).
Sin embargo, este novedoso tratamiento no estaba exento de inconvenientes importantes tales como: a) la falta de una adecuada disolución del coágulo estimada en un 35-40% b) a pesar de la trombolísis, el flujo arterial no era óptimo para permitir una adecuada recuperación del miocardio isquémico (10,11), c) en algunos pacientes sobre todo aquellos mayores de 75 años, un importante riesgo de sangramiento (12) y d) sus contraindicaciones no son infrecuentes (hipertensión importante, cirugía reciente, alergia etc).
Tal vez motivado por alguna de las razones previamente anotadas, Meyer en 1982, describe la utilización de la angioplastía siguiendo a la administración de trombolíticos intracoronarios (13). En 1983 por primera vez Hartzler (14), describe con buenos resultados el uso de la angioplastía coronaria como tratamiento en el infarto agudo al miocardio sin la utilización previa de drogas trombolíticas. Esto se conoce como Angioplastía Primaria o Directa.
A continuación queremos presentarles nuestra experiencia preliminar con el uso de la Angioplastía Primaria como forma de tratamiento incial del infarto agudo al miocardio. ]]>
Material y método
En este trabajo se incluyeron 16 pacientes, todos con infarto agudo al miocardio en curso, cuyo tiempo de evolución osciló entre 30 minutos y 3 horas. Ninguno de los pacientes recibió terapia trombolítica. Antes de su ingreso a la sala de cateterismo cardíaco se les administró ácido acetil salicílico 325 mgs (aspirina); heparina no fraccionada 70 u/kg intravenosa directa; y algunos (10/16 pacientes) bolo de antiplaquetarios específicos inhibidores de los receptores IIb IIIa , abciximab ó tirofiban . El Abciximab en bolo e infusión (12 hrs) a dosis de 0.25 mgs x Kgs y 10mcg x minuto respectivamente. El Tirofiban en bolo 10 mcgr x Kgs e infusión a 0.15 mcg x Kg x minuto. De los 10 pacientes que recibieron terapia antiplaquetaria específica con inhibidores de los receptores IIb IIIa , 4 recibieron abciximab y 6 pacientes recibieron tirofiban. A la terapia antiplaquetaria de mantenimiento se agregaba ticlopidina o clopidogrel asociado a la aspirina.
La mayoría de los pacientes 12/16 eran del sexo masculino. La edad de los pacientes osciló entre 36 y 79 años con un promedio de 59 años. El resto de los datos demográficos de la población aparecen en el diagrama N° 0.
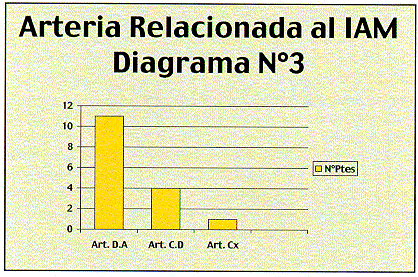
Al momento de realizar la angiografía, el flujo arterial coronario era TIMI 0 en 11/16 pacientes , TIMI 1 en 4/16 pacientes y TIMI 2 en 1/16 pacientes(diagrama N°1,2). La arteria involucrada en 11/16 pacientes era la descendente anterior ; en 4/16 pacientes la coronaria derecha y en 1/16 pacientes la arteria circunfleja (diagrama N°3).

En 10/16 pacientes la obstrucción arterial coronaria era proximal y en 6/10 pacientes la obstrucción estaba ubicada en el tercio medio (diagrama N° 4). En cuanto a la ubicación del infarto en 11/16 pacientes era anterior, 4/16 pacientes el infarto era inferior y en 1/16 pacientes el infarto era lateral (diagrama N°5).
El diámetro de balón más utilizado fue de 3 mm en 11/16 pacientes; 3.5 mm en 2/16 pacientes y de 2.5 mm en 3/16 (diagrama N°6). Se utilizó Stent en 11/16 pacientes. En 9/16 paciente se utilizó NIR stent y en el resto (2/16 pacientes) Multilink y CrossFlex (diagrama N°7). En 5/16 pacientes se realizó angioplastía solo con balón (diagrama N°8).
Resultados
]]> De los 16 pacientes incluídos en el estudio de angioplastía primaria, 15 pacientes tuvieron una evolución excelente, sin evidencias de reinfarto, muerte o revascularización del vaso trombosado que motivó la angioplastía durante su estadía en el hospital. En los 15 pacientes se logró obtener un flujo TIMI 3 posterior al procedimiento (diagrama N°9).Hubo una sola defunción que correspondió a un infarto inferior en shock cardiogénico, el cual había presentado múltiples episodios de fibrilación ventricular y descargas eléctricas durante las maniobras de resucitación en el cuarto de urgencia. En ningún momento se logró estabilizar al paciente desde su llegada al hospital hasta su traslado a la sala de cateterismo. La coronariografía reveló severa afección del sistema coronario izquierdo con obstrucción crítica de la coronaria derecha, a la que se le colocó un stent (multi-link) sin éxito requiriendo cirugía de by-pass aortocoronario urgente falleciendo en el acto operatorio.
Discusión
Nosotros hemos presentado 16 casos de angioplastía directa como tratamiento primario del infarto agudo al miocardio con resultados similares a los reportados en la literatura. En 15 de los 16 pacientes se logró mediante la angioplastía recanalizar la arteria responsable del infarto. Durante la estadía en el hospital de estos 15 pacientes no se detectaron complicaciones tales como reoclusión arterial, reinfarto, muerte o recanalización de la arteria afectada. Hubo una sola defunción atribuída principalmente a las complicaciones del infarto. De los infartos tratados mediante recanalización mecánica por angioplastía, 12 pacientes sufrían infarto anterior; 3 pacientes infarto inferior y un paciente infarto lateral.
La experiencia presentada nos llevan a plantear la discusión tomando en cuenta los siguientes puntos como referencia:
a) Por qué se optó por la angioplastía primaria en vez del tratamiento convencional con drogas trombolíticas?
b) Cuál es el papel de los antiplaquetarios específicos bloqueadores de los receptores IIB-IIIA y la heparina como medicamentos complementarios en la recanalización mecánica mediante angioplastía?
c) Cuál es la contribución de los Stents en esta nueva modalidad de tratamiento?.
]]> A continuación discutiremos cada una de las interrogantes planteadas previamente.POR QUE SE OPTO POR LA ANGIOPLASTIA PRIMARIA O DIRECTA EN VEZ DEL TRATAMIENTO TROMBOLITICO CONVENCIONAL?
Actualmente existe mucha controversia de los beneficios de la angioplastía primaria sobre la trombolísis sistémica como formas de tratamiento del infarto agudo al miocardio. Es oportuno al respecto hacer referencia al más grande estudio aleatorizado en donde se comparan los dos tratamientos: la angioplastía primaria y la trombolísis. Nos referimos al estudio GUSTO II b (15) en el que la mortalidad de los pacientes a los 30 días y 6 meses no fue estadísticamente muy diferente entre las dos modalidades de tratamiento. Así los puntos finales tomados en cuenta tales como reinfarto, muerte y accidente vascular cerebral a los 30 días fue de 9.6% para los pacientes tratados con angioplastía primaria y de 13.7 % para los pacientes que recibieron terapia trombolítica con tPA a dosis de carga ("front-loaded"). A los 6 meses el beneficio antes descrito disminuyó a la mitad, obteniéndose una diferencia absoluta entre los dos tratamientos de solamente 2.4%, lo cual es estadísticamente poco significativo.
Existen otros estudios claramente a favor de la angioplastía primaria . Nos referimos a un reciente meta-análisis de 10 estudios aleatorizados que incluyeron 2,606 pacientes en donde se demostró una clara disminución en la mortalidad de los pacientes sometidos a angioplastía primaria (16). Existen también estudios de seguimiento hasta por 2 años de los pacientes sometidos angioplastía primaria con persistente beneficio y significativa reducción de la mortalidad (PAMI-I) (17), en comparación con el grupo de pacientes que recibio tPA por ejemplo: reinfarto y muerte 14.9% en el grupo tratado con angioplastía primaria y 23% el grupo que recibió terapia trombolítica; isquemia recurrente 36.4% vs 48% y reintervención 27.2% vs 46.5% respectivamente.
Otros dos importantes estudios NRMI-2 (18) y el estudio Alemán ALKK (19) no parecen puntualizar la ventaja de un tipo de tratamiento sobre el otro. Sin embargo, sí reafirman la posible superioridad de la angioplastía primaria en cierto grupo de pacientes que consideran de más alto riesgo tales como: pacientes con infartos anteriores extensos, pacientes ancianos, pacientes hemodinámicamente inestables y en shock cardiogénico y pacientes con infarto inferior y compromiso del ventrículo derecho.
En nuestros pacientes, optamos por la angioplastía primaria por la presencia de infarto anterior extenso en la mayoría de los casos; en otro de los pacientes el infarto anterior se presentó en un hombre mayor de 75 años. De los pocos casos de infarto inferior, en uno de ellos era evidente su inestabilidad hemodinámica y en el otro se constató el compromiso del ventrículo derecho por electro y ecocardiograma.
Es importante antes de pasar a discutir otro de los aspectos sobre angioplastía primaria, que reafirmemos las ventajas de la misma sobre la terapia trombolítica. La angioplastía primaria tiene riesgo más bajo de accidente vascular cerebral hemorrágico (20); permite una mejor estratificación del riesgo del paciente basado en la anatomía coronaria (21); determina una mejor calidad de flujo sanguíneo (TIMI 3) posterior a la angioplastía primaria (22). Además de las bondades del procedimiento es oportuno también mencionar las limitaciones de la misma, por ejemplo : recurrencia de isquemia miocárdica en el 10-15% de los pacientes (23,24); reinfarto 3-5% de los pacientes antes de su salida del hospital; reoclusión de la arteria relacionada al infarto en un 10% (25,26,27), re-estenosis angiográfica 37-47%; reoclusión tardía de la arteria relacionada al infarto 9-15% (28,29); el 20% del total de pacientes sometidos a este procedimiento requerirán una nueva angioplastía o cirugía de by-pass a los 6 meses.
El tiempo transcurrido desde la llegada del paciente al cuarto de urgencia hasta el momento en que se realiza la angioplastía, se conoce como "Tiempo de puerta al balón", ésto tiene importancia porque la mortalidad es directamente proporcional al incremento en la duración del "tiempo de puerta al balón"(30,31). Lo ideal es entre 60-90 minutos.
CUAL ES EL PAPEL DE LOS ANTIPLAQUETARIOS ESPECIFICOS BLOQUEADORES DE LOS RECEPTORES IIb-IIIa Y DE LA HEPARINA COMO MEDICAMENTOS COMPLEMENTARIOS DE LA RECANALIZACION MECANICA MEDIANTE ANGIOPLASTÍA?
]]> Con respecto al uso de los inhibidores de las glicoproteínas IIb-IIIa y angioplastía primaria, en nuestros pacientes se utilizaron dos de estos compuestos, el Abxicimab (Reo-Pro) y el Tirofiban (Aggrastat) como terapia antiplaquetaria específica coadyuvante. Solo 10/16 pacientes recibieron IIb-IIIa., 4 pacientes Abxicimab y 6 pacientes Tirofiban (diagrama N° 9). Sin embargo, en la literatura la experiencia favorable al respecto es con el Abxicimab. Este agente fue utilizado en 483 pacientes presentados en el estudio RAPPORT (Reo-Pro Primary PTCA Organization and Randdomization Trial) en donde la incidencia de reinfarto, muerte y revascularización de la arteria enferma ("target vessel revascularization") disminuyó a un 40% en 30 días (11.2% vs 5.8%) (32,33). El Tirofiban utilizado en el estudio RESTORE no demostró tal reducción en la incidencia de estos parámetros (34). Las razones esbozadas para ello pueden ser varias, tal vez tenga que ver la no especificidad del Abxicimab, el cual se fija a otros receptores (vitronectina, MAC-1 etc); su vida media más prolongada; su empleo antes de iniciar el procedimiento terapéutico y no inmediatamente después de cruzar la guía de alambre como fue utilizado el Tirofiban, etc... Es posible que a corto plazo ( a mediados del 2000) a través del estudio TARGET con un total de 4300 pacientes se establezca si realmente existe diferencia entre el Abxicimab y Tirofiban como tratamiento simultáneo asociado a la angioplastía primaria.Con respecto al uso de la heparina, particularmente heparina no fraccionada, este agente se emplea en forma rutinaria previa a la intervención coronaria percutánea. Datos y observaciones de estudios "no randomizados" sugieren alcanzar un tiempo activado de coagulación (ACT) mayor de 300 segundos (35). Sin embargo, no existe un consenso sobre el nivel óptimo del mismo. Es claro que a mayor ACT, menor incidencia de cierre abrupto de la arteria pero mayor posibilidad de sangrado (36,37). En algunos de nuestros pacientes utilizamos la heparina fraccionada o de bajo peso molecular como terapia alterna posterior a la angioplastía primaria basados en sus bondades conocidas: mayor biodisponibilidad (90% vs 40% heparina no fraccionada); mayor inhibición del factor Xa comparado al factor II a; ausencia de inhibición por el factor plaquetario-4 ; reducción del incremento durante la fase aguda del factor de von Willebrand, importante en el fenómeno inicial de la adhesión plaquetaria, etc (38). Dadas todas estas ventajas, la heparina de bajo peso molecular, enoxaparina a dosis de 1 mgr/Kg I.V.
( 0,75 mg/kg asociado a antiplaquetario ) en bolo antes de la angioplastía, ha sustituido a la heparina no fraccionada con buenos resultados y sin mayor incidencia de sangrados mayores, menores o necesidad de transfusiones que lo reportado en el estudio EPILOG con heparina no fraccionada a bajas dosis (NICE-4) (39).
CUAL ES LA CONTRIBUCION DE LOS STENT EN ESTA NUEVA MODALIDAD DE TRATAMIENTO?
De la totalidad de 16 pacientes tratados mediante angioplastía primaria, en 12 casos se utilizó Stent. Esto se decidió de acuerdo al resultado posterior a la angioplastía con balón. En general, si el resultado angiográfico post-dilatación con balón era considerado como óptimo, no se le colocaba Stent. Cuál es la tendencia actual con respecto a la angioplastía primaria con balón y la angioplastía primaria con Stent?. Las preferencias tienden a inclinarse hacia la angioplastía primaria con la colocación de Stent de acuerdo al estudio piloto PAMI(40), PASTA (41)en donde a 7 meses y 1 año respectivamente la incidencia de reinfarto, muerte cardíaca y revascularización del vaso afectado
("target vessel revascularization") disminuyó en ambos estudios a favor de la angioplastía primaria con Stent. Existen otros dos estudios CADILLAC (42) y ADMIRAL(43) que favorecen el uso de Stent en la angioplastía primaria. En estos dos estudios se utilizó el abciximab como antiplaquetario específico. Con respecto al estudio CADILLAC fueron evaluados 1961 pacientes con infarto agudo de menos de 12 horas de evolución, con la administración concomitante de abciximab. La isquemia miocárdica recurrente se redujo mayormente en la angioplastía primaria con Stent (de 3.9% a 1.2% ) en relación a la angioplastía primaria con balón (de 4.9% a 1.4%); según el estudio PAMI-Stent la mortalidad tampoco aumenta en forma significativa con el uso de stents (44). Así, por lo pronto todo parece indicar que la angioplastía primaria con el uso de Stent es superior a la angioplastía primaria con balón y con la utilización concomitante de los antiplaquetarios específicos como el abciximab, ésta constante se sigue manteniendo. Es importante mencionar que los resultados de la angioplastía primaria con balón asociado a antiplaquetarios específicos como el abciximab son superiores a los resultados de la angioplastía primaria con balón sin antiplaquetarios.
Conclusión
La angioplastía primaria como terapia inicial del infarto agudo al miocardio, es una alternativa terapéutica efectiva. Este novedoso y especializado tratamiento se encuentra al alcance de nuestra población y conlleva un alto porcentaje de éxito y baja tasa de complicaciones. Los datos presentados reproducen la experiencia de los grandes centros cardiológicos del mundo. ]]>
Referencias
1. Herrick JB: Clinical features of sudden obstruction of the coronary arteries. JAMA 59: 2015-2020, 1912. [ Links ]
2. Davies M, Woolf N, Robertson W: Pathology of acute myocardial infarction with particular reference to occlusive coronary thrombi. Br. Heart J. 38: 659-664, 1976. [ Links ]
3. Davies MJ, Thomas A: Thrombosis and acute coronary artery lesion in sudden cardiac ischaemic.
N. Engl. J Med. 310: 1137-1140, 1984.
4. Ellis SG, O´Neill WW, Bates et al: Implication for patient triage from patient survival and left ventricular functional recovery analysis in 500 patients treated with coronary angioplasty for acute myocardial infarction.
J Am Coll Cardiol 13: 1251-1259, 1989.
5. Robert WC,Buja LM: The frecuency and significance of coronary arterial and other observation in fatal acute myocardial infarction : A study of 107 necropsy patient. Am J Med 52: 425-443, 1972. [ Links ]
6. DeWood MA, Spores J,Nosske R et al: Prevalence of total coronary occlusion during the early hours of transmural myocardial infarction. N Engl J Med. 303: 897-902, 1980. [ Links ]
7. Rentrop P, Blanke H, Karsch KR et al: Selective intracoronary thrombolysis inacute myocardial infarction and unstable angina pectoris. Circulation 63: 307-317, 1981. [ Links ]
8. Weaver WD,Cerqueira M, Hallstrom AP,et al: Pre-hospital initiated vs hospital initiaded thrombolytic therapy : The Myocardial Infarction Triage and Intervention trial. JAMA 270: 1211-1216, 1993. [ Links ]
9. Granger CB, Califf RM, Topol EJ: Thrombolytic therapy for acute myocardial infarction . Drugs 44: 293-325,1992. [ Links ]
10. Lincoff AM,Topol EJ: The illusion of reperfusion: Does any one achieve optimal myocardial reperfusion? Circulation 87: 1792-1805 (erratum 88:1361-1375),1993. [ Links ]
11. Lincoff AM,Topol EJ: Trickle down thrombolysis . J Am Coll 21: 1396-1398,1993. [ Links ]
12. Fibrinolytic Therapy Trialists´(FTT) Collaborative Group: Indication for fibrinolytic therapy in suspected acute myocardial infarction: Collaborative overview of early mortality and major morbility results from all randomised trials of more than 1000 patient. Lancet 343: 311-322, 1994. [ Links ]
13. Meyer J, Merx W, Schmitz H, et al: Percutaneus transluminal coronary angioplasty inmediately after intracoronary streptolysis of transmural myocardial infarction. Circulation 66: 905-913, 1982. [ Links ]
14. Hartzler GO,Rutherford BD, McConahay DR et al: Percutaneus transluminal coronary angioplasty with and without thrombolytic therapy for treatment of acute myocardial infarction. Am Heart J 106: 965-973. 1983. [ Links ]
15. GUSTO IIb angioplasty substudy investigators: A clinical trial comparing primary coronary angioplasty with tissue plasminogen activator for acute myocardial infarction. N. Engl J. Med 1997: 336: 1621-1828. [ Links ]
16. Weaver WD, Simes J, Betriu A, Grines CL, Zijlstra F, Garcia E, et al : Comparison primary coronary angioplasty and intravenous thrombolytic therapy for acute myocardial infarction. JAMA 1997, 278: 2093-2098. [ Links ]
17. Nunn CM,O ´Neil ,Rothbaum D, Stone GW, O´Keefe J, Overlie P et al: Long term outcome after primary angioplasty: report from the Primary Angiplasty in Myocardial Infarction (PAMI-1) Trial. J. Am Coll Cardiol
1999, 33 : 640-646.
18. Tiefenbrunn AJ, Chandra NC,French WJ, Gore JM, Roger WJ: Clinical experience with primary percutaneous transluminal coronary angioplasty compared with alteplase (recombinant tissue type plasminogen activator) in patient with acute myocardial infarction. J Am Coll Cardiol 1998, 31: 1240-1245. [ Links ]
19. Vogt A, Niederer W, Pfafferott C, Engels HJ, Heinrich KW, Merx W et al: on behalf of the ALKK study group: Direct percutaneous trasluminal coronary angioplasty in acute myocardial infarction: predictor of short term outcome and impact of coronary stenting. Eur. Heart J 1998, 19: 917-921. [ Links ]
20. Gibbons RJ,Holmes DR,Reeder Gs,Bailey KR, Hopfenspirger MR, Gersh BJ, for the Mayo Coronary Care Unite and Catheterization Laboratory Groups: Immediate angioplasty compared with the administration of a thrombolytic agent followed by conservative treatment for myocardial infarction. N Engl J Med 1993, 328: 685-691. [ Links ]
21. Grines C, Marsalese D, Brodie B, Griffin J, Donohue B,Sampaolesi A,Constantini A, Stone G,Spain M, Jones D, Sachs D, Mason D, O´Neil W: Acute cath provides the best method of risk stratifying MI patients (Abstract). Circulation 1995, 92 (suppl I) : l-531. [ Links ]
22. de Boer MJ, Suryapranata H,Hoorntje JCA, Reiffers S,Liem AL, Miedema K Herrmens WT, van den Brand MJBM, Zijlstra F: Limitation of infarct size and preservation of left ventricular function after primary coronary angioplasty compared with intravenous streptokinasa in acute myocardial infarction. Circulation 1994, 90: 753-761. [ Links ]
23. Stone GW,Grines CL,Broene KF, Marco J,Rothbaum D, O´Keefe J, Hartzler GO Overlie P, Donohue B, Chelliah N, Timmis GC, Vlietstra R,Strzelecki M, Puchrowica-Ochocki,O´Neil WW: Predictor of in hospital and 6 month outcome after acute myocardial infarction in the reperfusion era: the Primary Angioplasty in Myocardial Infarction (PAMI) Trial . J Am Coll Cardiol 1995, 25: 370-377. [ Links ]
24. Michel KB, Yusuf S: Does PTCA in acute myocardial infarction affect mortality and reinfarction rate?: a quantitative (meta-analysis) of the randomized clinical trial. Circulation 1995, 91: 476-485. [ Links ]
25. Zijlstra F, DeBoer MJ, Hoorntje JCA et al: A comparison of immediate coronary angioplasty with intravenous streptokinase in acute myocardial infarction. N Engl J Med 1993, 328: 680-684. [ Links ]
26. Gibbons RJ, Holmes DR, Reeder GS, et al: for the Mayo Coronary Care Unite and Catheterization Laboratory Groups: Immediate angioplasty compared with the administration of a thrombolytic agent follewed by conservative treatment for myocardial infarction. N Engl J Med 1993, 328: 685-691. [ Links ]
27. Ohman EM, Califf RM, Topol EJ et al: Consequence of reoclusion after successful reperfusion therapy in acute myocardial infarction. Circulation 1990, 82: 781-791. [ Links ]
28. O´Neill WW, Weintraub R, Brines CL et al: A prospective placebo controlled randomized trial of intravenous streptokinase and angioplasty versus alone angioplasty therapy of acute myocardial infarction.Circulation 1992, 86:1710-1717. [ Links ]
29. Nakagawa Y, Iwasaki Y, Kimura R et al: Serial angiographic follow up after successful direct angioplasty for acute myocardial infarction. Am J. Cardiol 1996, 78: 980- 984. [ Links ]
30. Cannon CP,Lambrew CT, Tiefenbrunn AJ, French WJ, Gore JM, Weaver DW Roger WJ, for the NRMI-2 Investigator: Influence of door to ballon time on mortality in primary angioplasty results in 3,648 patient in the second National Registry of Myocardial Infarction (NRMI-2) (Abstract). J Am Coll Cardiol 1996,27 (suppl A): 61-A-62A. [ Links ]
31. The global use of Strategies to Open Occluded Coronary Arteries in Acute Coronary Syndrome (GUSTO IIb) Angioplasty substudy Investigators: A clinical Trial comparing primary coronary angioplasty with tissue plasminogen activator for acute myocardial infarction. N. Engl J. Med 1997, 336: 1621-1628. [ Links ]
32. Brener SJ,Barr LA,Burchenal JEB, et al: Randomized, placebo-controlled trial of platelet glycoprotein IIb-IIIa blockade with primary angioplasty for acute myocardial infarction. Circulation 1998; 98: 734-741. [ Links ]
33. Lefkovits J, Ivanhoe RJ, Califf RM,et al: and the EPIC Investigators. Effect of platelet glycoprotein IIb-IIIa receptor blockade by chimeric monoclonal antibody (Abciximab) on acute and six-month outcomes after percutaneous coronary angioplasty for acute myocardial infarction. Am J Cardiol 1996; 77:1045-1051. [ Links ]
34. RESTORE Investigators. Effects of platelet glycoprotein IIb-IIIa blockade with tirofiban on adverse cardiac events in patient with unstable angina or acute myocardial infarction undergoing coronary angioplasty. Circulation 1997; 96: 1445-1453. [ Links ]
35. Ryan TJ,Bauman WB, Kennedy JW, et al : ACC/AHA guidelines for percutaneous transluminal coronary angioplasty: A report of the American College of Cardiology American Heart Association Task Force on Assessment of Diagnostic and Therapeutic Cardiovascular Procedures (Committee on percutaneous transluminal coronary angioplasty). J Am Coll Cardiol 1993; 22: 2033-2054.36. [ Links ]Narins CR,Hillegas WB, Nelson CL et al: Relationship between activated clotting time during angioplasty and abrupt closure. Circulation 1996;93:667-671.
37. Hillegass WV,Narins CR,Brott BC et al: Activated clotting time predicts bleeding complication from angioplasty. J Am Coll Cardiol 1994; 23: 184 A. 38. [ Links ]Xiao Z, Theroux P, Platelet activation with unfractionated heparin at therapeutic concentration and comparison with a low molecular weight heparin with a direct thrombin inhibitor. Circulation 1998; 97: 251-256. [ Links ]
39.Kereiakes D,Fry E,Lengerich R et al: Abciximab associated thrombocytopenia is reduced by enoxaparin: Preliminary result of the NICE-4 (abstr) Am J Cardiol 1999; 84; 67P. [ Links ]
40. Stone GW, Brodie BR,Griffin JJ, et al. Clinical and angiographic follow up after primary stenting in acute myocardial infarction: The Primary Angioplasty in Myocardial Infarction (PAMI) stent pilot trial. Circulation
1999;99:1548-1554.
41.Saito S,Hosokawa G,Tanaka S,Nakamura S for the PASTA Trial Investigator. Primary stent implatation is superior to ballon angioplasty in acute myocardia infarction (PASTA) trial.Cathet Cardiovasc Intervent 1999; 48: 262-268. [ Links ]
42. Stone GW.Stenting in acute myocardial infarction: Observational studies and randomized trial. J Invas Cardiol 1998; 10: 17A-26A. [ Links ]
43. Montalescot G,Barragan P,WittenbergO et al: Abciximab associated with primary angioplasty and stenting in acute myocardial infarction: The ADMIRAL study 30-day final result (abstr). Circulation 1999; 100: 1-87. [ Links ]
44.Stone GW,Controlled Abciximab and Device Investigation to Lower Late Angioplasty Complication (CADILLAC) trial: presented at 72nd Scientific Session of the American Heart Association, Plenary Session XII : Late Breaking Clinical Trial. November 1999. Data retrieved from American Heart Association web site www.americanheart.org [ Links ]
*Cardiólogos Asociados de Panamá, Centro Médico Paitilla,
Hospital Nacional, Ciudad de Panamá, Panamá
E-mail:dpichel@pananet.com.