Evaluación de la infiltración local de bupivacaina en el manejo del dolor post salpingectomía parcial bilateral
(Evaluation of Local Infiltration with Bupivacaine for Pain Management after Partial Bilateral Salpingectomy)
Mariella Fajardo-Arcia1, Leonardo Orozco-Saborío2, Gerardo Montiel-Larios3
]]>
*Correspondencia
Resumen
Objetivo: Se valoró la eficacia de la infiltración local de bupivacaína en la disminución del dolor postoperatorio en las pacientes sometidas a salpingectomía parcial bilateral por mini laparotomía.
Métodos: Un total de 100 participantes programadas para esterilización quirúrgica fueron aleatorizadas a un grupo intervención donde se aplicó 2.5mg de bupivacaína en el mesosalpinx y 2.5mg en el muñón de cada trompa de Falopio y a un grupo control sin intervención alguna. El dolor postoperatorio fue medido después de una y cuatro horas usando la escala visual análoga (EVA, 0-10 cm),y se determinó la necesidad y cantidad de analgesia postoperatoria. Para la comparación de medias se utilizó la prueba t-Student, y todos los análisis fueron realizados por medio del software estadístico Stata 10.0 definiendo como estadísticamente significativo un punto crítico de 0.05 (p≤0.05).
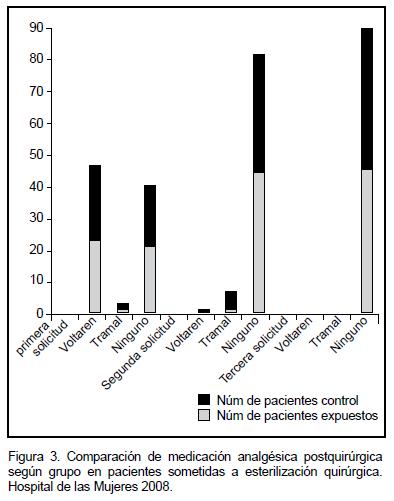
Resultados: La puntuación en la escala visual análoga (EVA), en el grupo de bupivacaína fue 4.7 y 2.6 comparado con 5.3 y 2.6 en el grupo control, a la hora y a las cuatro horas respectivamente (todas las p> 0.05).La aplicación de bupivacaína redujo la solicitud por parte de la participante de una segunda dosis de analgesia después de la primera hora de la cirugía de forma significativa (p<0.03).En el grupo control se evidenció un mayor uso de opiodes (n=8) en comparación con el grupo en el que se aplicó bupivacaína (n=1). La aplicación de bupivacaína en los muñones de las trompas uterinas y en el mesosalpinx al realizar la esterilización quirúrgica por mini laparotomía, no produjo diferencias en la medición del dolor post operatorio en la escala visual análoga a la hora y a las cuatro horas.
Conclusión: La aplicación de bupivacaína es efectiva en la reducción de la necesidad de analgesia después de una hora de la cirugía y en la reducción de la aplicación de fármacos opiodes.
]]> Descriptores: bupivacaína, esterilización quirúrgica, dolor postoperatorio.
Abstract
Aim: To evaluate the efficacy of locally applied bupivacaine in decreasing postoperative pain in patients undergoing minilaparotomybilateral partial salpingectomy.
Methods: A total of 100 women scheduled for surgical sterilization were randomized to either an intervention group that received 2.5mg of bupivacaine in the mesosalpinx and 2.5 mg in the stump of each fallopian tube or a control group that received no intervention. Postoperative pain was measured at one and four hours using the visual analogue scale (VAS, 0-10 cm). In addition, these scores determined the necessity and quantity of postoperative analgesia.To compare means we used Student t-test and all tests were performed using Stata Statistical Software 10.0.A critical point of 0.05 (p≤ 0.05) was defined as statistically significant.
Results: Scores on the visual analogue scale (VAS cm) were 4.7 at one hour and 2.6 at four hours in the intervention group, compared to 5.3 at one hour and 2.6 at four hours in the control group (p>0.05). The application of bupivacaine significantly reduced requests by participants for a second dose of analgesics after the first hour of surgery (p<0.03). The control group showed an increased use of opiates (n=8) in comparison to the bupivacaine intervention group (n=1).The application of bupivacaine to the fallopian tube stumps and mesosalpinx at the time of minilaparotomy surgical sterilization does not produce differences in the postoperative pain management as measured by the visual analogue scale at one and four hours post-surgery.
Conclusion: The application of bupivacaine is effective in reducing the need for analgesics one hour post-surgery and reduces the use of opioids.
Keywords: Bupivacaine, surgical sterilization, post operative pain.
]]>
La esterilización femenina, la cual es también llamada ligadura u oclusión de las trompas uterinas, ha sido uno de los métodos contraceptivos más utilizado alrededor del mundo.1,2 Más de un millón de mujeres en edad reproductiva han sido esterilizadas y se estimó que desde 1982, más de 100 millones de mujeres, solo en el mundo en desarrollo, buscarán esterilizarse.3
La esterilización ha tenido una evolución similar a muchos otros procedimientos quirúrgicos, en un esfuerzo para simplificar el procedimiento muchas técnicas han sido desarrolladas, desde la realización de la esterilización a través de una minilaparotomía, hasta las técnicas de esterilización laparoscópica.4-6
En países desarrollados se utiliza la vía laparoscópica, basados en la seguridad y efectividad de la misma. Sin embargo, en países en vías de desarrollo se utiliza la mini laparotomía debido a los escasos recursos disponibles, realizándose por ejemplo, 696 procedimientos en el año 2006 en el Servicio de Ginecología del Hospital de las Mujeres en San José, Costa Rica.7
Se han realizado diversos estudios para valorar la mejoría del dolor postoperatorio utilizando anestésicos locales en la salpingectomía parcial bilateral. Demostrándose en la mayoría, que el uso de dichos anestésicos disminuyen el puntaje en las escalas del dolor, además de una disminución de la necesidad de analgesia post operatoria.8-27 Sin embargo, la mayoría de los estudios realizados utiliza la vía laparoscópica como abordaje, por lo que el objetivo del presente estudio fue evaluar la eficacia de lainfiltración local de bupivacaína para reducir el dolor postoperatorio en las pacientes sometidas a salpingectomía parcial bilateral por la vía de mini laparotomía.
Materiales y métodos
El diseño del estudio fue aleatorizado, doble ciego. Previa aprobación del Comité de Ética Institucional y obtención del Consentimiento Informado, 100 pacientes programadas para esterilización quirúrgica en el programa de cirugía ambulatoria del Servicio de Ginecología del Hospital de las Mujeres, fueron enroladas en el estudio. Los criterios de inclusión fueron, mujeres mayores de 18 años y que cumplieran con los trámites pertinentes para la esterilización quirúrgica. Toda mujer con antecedentes de cirugía tubaria, portadora de síndrome adherencial, dolor pélvico crónico, patologías psiquiátricas o retardo mental y con antecedentes de reacción alérgica a cualquier tipo de anestésicos locales, fueron excluidas. La población muestra de este ensayo se tomó en base a un estudio,28 en donde se determinó que 57 mujeres fueron necesarias para detectar, con un 95% de probabilidad y un 90% de poder, una reducción de un 25% en el puntaje de la escala visual análoga a las 2 horas.
]]> Al conocer que con 57 mujeres se obtienen los indicadores arriba mencionados y tomando en cuenta el número de grupos a comparar que tiene este estudio, se obtuvo una muestra de 100 mujeres aleatorizadas equitativamente a cada grupo de tratamiento.Todos los procedimientos fueron realizados bajo un régimen estandarizado de anestesia general. Previo a la inducción anestésica las participantes fueron premedicadas con 10 mg de metoclopramida, 1 mg de midazolam y 0.75 microgramos/kg de fentanyl, este último fue utilizado como analgesia.
La inducción anestésica se realizó de forma estándar con propofol a dosis de 2 mg/kg, se aplicó 5 mg de itracurio y 100mg de succinilcolina para facilitar la entubación endotraqueal. Todas las participantes se sometieron a ventilación mecánica y el mantenimiento anestésico se realizó con sevoflorane y oxígeno. La monitorización transoperatoria se llevó a cabo bajo los estándares clínicos. Al final de la cirugía la anestesia se discontinuó y el bloqueo no se revirtió. La técnica utilizada para realizar la esterilización quirúrgica fue la salpingectomía parcial bilateral con la técnica de Pomeroy modificada. Al grupo de intervención se le aplicaron 5cc de bupivacaína al 0.5% (presentación frasco de 5mg/ml) en cada trompa de Falopio de la siguiente manera, 2.5cc en el mesosalpinx y 2.5 cc en el muñón quirúrgico. Al grupo control no se le aplicó ningún medicamento en las trompas de Falopio.
En el salón de internamiento se inició la evaluación de la escala visual análoga (EVA 0-10 cm) a 1hora y a las 4 horas después de la intervención quirúrgica.
]]> El régimen utilizado en caso de que la participante solicitara analgesia en el salón de internamiento fue, una dosis de 75mg de diclofenaco IM. Ante una segunda solicitud se aplicó 50mg de tramadol subcutáneo y en caso de una tercera solicitud, morfina 15mg subcutáneo. El uso de analgesia postoperatoria se aplicó por el personal de enfermería según los requerimientos expresados por cada paciente previa indicación médica, quedando registrado en el expediente. La hora de aplicación y el tipo de analgesia fueron registrados.Para el análisis de los datos se realizó la caracterización de las pacientes por medio de la estimación de frecuencias y proporciones para las variables cualitativas y la estimación de medias y desviación estándar como medidas descriptivas para las variables cuantitativas para cada uno de los grupos. Se realizó la comparación de las características por medio de la estimación de la prueba de t-Student para las variables cuantitativas y de chi cuadrado de homogeneidad para la distribución de las variables cualitativas entre grupos.
Se realizó la comparación de la escala visual análoga entre los grupos en el tiempo 1 hora y 4 horas por medio de la comparación de medias utilizando la prueba t-Student. Todos los análisis fueron realizados por medio del software estadístico Stata 10.0 definiendo como estadísticamente significativo un punto crítico de 0.05 (p≤0.05).
Resultados
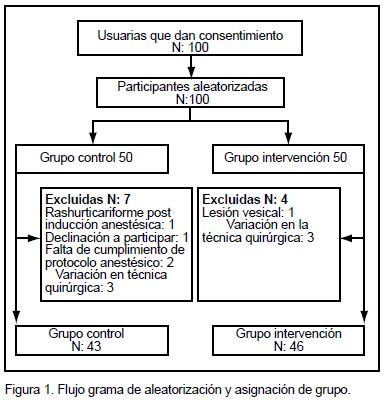
Del primero de abril al nueve de septiembre del 2008, un total de 100 participantes firmaron el Consentimiento Informado.
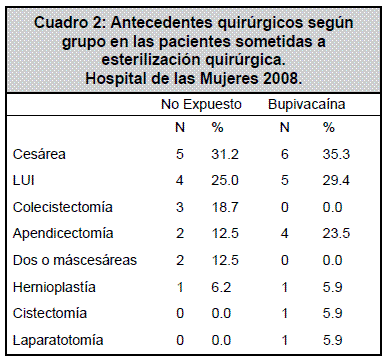
Se excluyeron en total once participantes, de las cuales siete pertenecían al grupo control, una erupción urticariforme post inducción anestésica, una por declinación a participar, dos por falta de cumplimiento de protocolo anestésico, y tres por variación en la técnica quirúrgica. En el grupo de intervención se excluyeron cuatro pacientes, una por lesión vesical y tres por variación en la técnica quirúrgica. Esto resultó en 43 participantes analizados en el grupo control y 46 en el grupo de intervención.
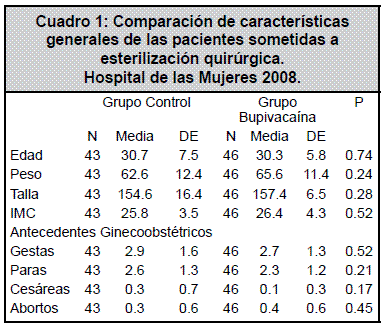
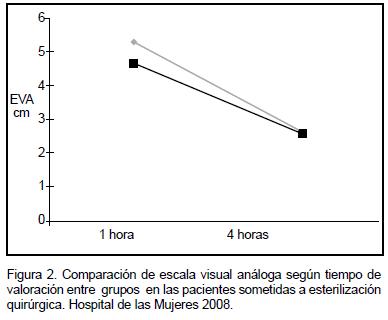
La puntuación del EVA a la hora después de la cirugía en el grupo al que se le aplicó bupivacaína fue de 4.7 ± 2.7 y en el grupo control fue de 5.3 ± 3.2 (p=0.30). A las cuatro horas después de la cirugía fue de 2.6 ± 2.2 en el grupo al que se le aplicó bupivacaína y de 2.6 ± 2.3 en el grupo control (Figura 2).
Se realizó un análisis exploratorio comparando el EVA del grupo de intervención y el grupo control a la hora y cuatro horas postquirúrgicas en las pacientes que no solicitaron analgesia después de la cirugía, no encontrándose diferencias significativas: 35.7 ± 24.8 para el grupo de intervención y 38.0 ± 29.8 para el grupo control a la hora (p=0.79); 23.9 ± 5.3 y 17.2 ± 2.8, a las cuatro horas respectivamente (p=0.29). Al comparar la magnitud en la reducción del puntaje del EVA en las pacientes que no solicitaron analgesia, se observó que en el grupo control la diferencia fue significativa cuando se comparó a la hora y a las cuatro horas, 38.0 ± 29.8 y 17.2 ± 2.8 respectivamente (p=0.01), no así en el grupo de bupivacaína, 35.7 ± 24.8, a la hora y 23.9 ± 5.3 a las cuatro horas (p=0.13).
Discusión
A diferencia de los estudios realizados anteriormente que mostraron una mejoría en las puntuaciones de las escalas del dolor posterior a la salpingectomía parcial bilateral,10, 28, 30 nuestro estudio evidenció que la aplicación de bupivacaína en los muñones de las trompas uterinas y en el mesosalpinx al realizar la esterilización quirúrgica por mini laparotomía, no produjo diferencias significativas en la puntuación del dolor post operatorio usando la escala visual análoga a la hora y a las cuatro hora después de la cirugía.
Cabe destacar que toda la evidencia en donde la aplicación de algún anestésico local fue efectiva, el abordaje quirúrgico fue a través de la paroscopía, esto puede sugerir que la mayor sección de tejidos de la pared abdominal en el acceso a la cavidad pélvica con el abordaje por mini laparotomía, influye de forma importante en el dolor postoperatorio.
Sin embargo, la aplicación de bupivacaína fue efectiva en la reducción de la necesidad de analgesia posquirúrgica y uso de opioides después de una hora de la cirugía, esto concuerda con un gran número de estudios en donde se ha evidenciado una reducción variable en el consumo de analgesia y uso de opiodes en los grupos donde se utilizó algún analgésico local.l7-10,16,17,20 Este hecho evidencia que la aplicación de bupivacaína puede tener un efecto beneficioso a corto plazo después de la cirugía, aunque no se refleje en la puntuación de la EVA, ya que en el grupo control se observó una reducción del puntaje de la EVA similar al grupo de la intervención (Figura 2). Este hecho se podría explicar si diferenciamos la magnitud del dolor de la percepción o tolerancia al mismo.
El dolor es una experiencia emotiva personal, cuya magnitud solo puede ser descrita subjetivamente por la persona afectada. Se sabe que la percepción del dolor en un determinado sujeto varía considerablemente en relación con factores emocionales y anímicos,28,31 es en este contexto que la importancia de los factores psicológicos, cognoscitivos y conductuales se han convertido en factores determinantes en el abordaje del dolor.32-37 Ya antes se ha descrito esta misma situación, en donde se reportó menos uso de morfina a la hora después de la cirugía en el grupo de intervención, aunque la puntuación de la EVA durante el periodo del estudio fue similar en los grupos.38
Hay algunas limitaciones en nuestro ensayo. Primero, aunque la dosis que se utilizó ya se ha usado en otros estudios,7,10 en nuestro medio se hace difícil medir las concentraciones sanguíneas de la droga, y lograr la homogeneidad de la dosis aplicada dependía exclusivamente de cada cirujano. Segundo, no se documentó la cantidad de medicamentos analgésicos tomados por las participantes después del egreso, debido al aumento de trabajo que para la paciente representaría este auto reporte. Podría ser imaginable que hubo una diferencia en la cantidad de analgesia tomada entre los grupos. Sin embargo, debido a que las pacientes que tienen más dolor tomarían más analgesia, la diferencia en los niveles de dolor más bien disminuiría en lugar de enfatizarse y no sería ético negarle analgesia a una persona que tiene dolor.
En conclusión, el hecho de que la salpingectomía parcial bilateral por mini laparotomía sea un procedimiento ambulatorio, y que en algunos casos las pacientes no se egresan por referir mucho dolor, enfatiza la importancia de una mejoría en el alivio del dolor postoperatorio. La utilización de bupivacaína por esta vía de abordaje quirúrgica no parece beneficiar el cumplimiento de este objetivo. Sin embargo, parece ser efectiva en la disminución de la necesidad de analgesia post operatoria y en el uso de opioides.
La corta duración del efecto de este tratamiento podría posponer, y no eliminar la necesidad de otras drogas analgésicas; a si que el uso de bupivacaína, debería verse solo como un posible agregado, y no como un reemplazo de la terapia de analgesia tradicional.
]]> Agradecimientos y colaboradoresSe agradece al servicio de anestesia del HOMACE en especial al Dr. Leonardo Barquero, la Dra. Doris Sánchez y la Lic. Sara Campos por su colaboración a este ensayo.
Referencias
1. Limpaphayom K. Sterilization. Curr Opin Obstet Gynecol 1991; 3: 501-509. [ Links ]
2. World Health Organization. Contraceptive use and commodity cost of female sterilization. What health workers need to know. WHO/ FHE/ FPP 1994;94.2. [ Links ]
]]>
3. World Health Organization, Task Force on Female Sterilization, Special programmed of Research, Development and Research Training in Human Reproduction. Minilaparotomy or laparoscopy for sterilization. Am J Obstet Gynecol 1982;143:645-652. [ Links ]
4. Wheeless CR. Outpatient laparoscope sterilization under local anesthesia. Obstet Gynecol 1972; 39:767-770. [ Links ]
5. Osathanondh V. Suprapubic mini-laparotomy, uterine elevation technique: simple, inexpensive and out-patient procedure for interval female sterilization. Contraception 1974;10:251-262. [ Links ]
6. Uchida H. Uchidatubalsterilization. Am J ObstetGynecol 1975; 121:153-158. [ Links ]
7. Centro de estadística del Hospital de la Mujer Adolfo Carit Eva, San José Costa Rica. [ Links ]
8. Van Ee R, Hemrika DJ, de Blok S. Effects of ketoprofen and mesosalpinx infiltration on postoperative pain afeter laparoscopic sterilization. Obstet Gynecol 1996; 88: 568-72. [ Links ]
9. Alexander CD, Wetchler BV, Thompson RE. Bupivacaína infiltration of the mesosalpinx in ambulatory surgical laparoscopic tubal sterilization. Can J Anaesth 1987; 34: 362-5 [ Links ]
10. Kaplan P, Freund R, Squires J, Herz M. Control of immediate postoperative pain with topical bupivacaine hydrochloride for laparoscopic Falope ring tubal ligation. Obstet Gynecol 1990: 798-802 [ Links ]
11. Smith BE, MAcPherson GH, de Jorge M, Griffith JM. Rectus sheath and mesosalpinx block for laparoscopic sterilization. Anaesthesia 1991; 46:875-7 [ Links ]
12. Wheatley SA, Millar JM, Jadad AR. Reduction of pain afeter laparoscopic sterilization with local bupivacaine: a randomized, parallel, double- blind trial. Br J Obstet Gynaecol 1994; 101: 443-6 [ Links ]
]]>
13. Tool Al, Kammerer-Doak DN, Nguyen CM. Posoperative pain relief following laparscopic tubal sterilization with silastic bands. Obstet Gynecol 1997; 90: 731-4 [ Links ]
14. Koetsawang S, Srisupandit S, Apimas SJ, Champion CB. A comparative study of topical anesthesia for laparoscopic sterilization with the use of tubal ring. Am J Obstet Gynecol 1984; 150: 931- 3. [ Links ]
15. Barclay K, Calvert JP, Catling. Analgesia after laparocopic sterilization. Effect of 2% lignocaine gel applied to Filshie clips. Anaesthesia 1994; 49: 68-70. [ Links ]
16. Ezed UO, Shoulder VS, Martin JF. Local anaesthetic on doubled- blind controlled trial. Lancet 1995; 346:82-5 [ Links ]
17. Fiddes TM, Williams HW. Herbison GP. Evaluation of postoperative analgesia following laparoscopic application of Filshie clips.Br J Obstet Gynecol 1996; 103:1143-7. [ Links ]
18. McKenzie R, Phitayokorn P, Uy NTL. Topical etidocaine during laparoscopic tubal occlusion for postoperative pain relief. Obstet Gynecol 1986; 67:447-9 [ Links ]
19. Baram D, Smith C, Stinson S. Intraoperative topical etiodocaine for reducing postoperative pain after laparoscopic tubal ligation. J Reprod Med 1990; 35:407-10 [ Links ]
20. Loughney AD, Sarma V, Ryall EA. Intraperitoneal bupivacaine for the relief of pain following day case laparoscopy. Br J Obstet Gynaecol 1994; 101: 449-51. [ Links ]
21. Benhamou D, Narchi P, Mazoit JX, Fernandez H. Postoperative pain after local anesthesics for laparoscopic sterilization. Obstet Gynecol 1994; 84:877-80. [ Links ]
22. Callesen T, Hijort D, Mogensen T. Combined field block and i.p. instillation for pain management after laparoscopic sterilization. Br J Anaesth 1999; 82: 586-90. [ Links ]
]]>
23. Mohammed E, Lahsae M, Alborzi S, Vafaei H, Heinrich E. Comparative, double- blind, randomized, placebo-controlled trail of intraperitoneal of bupivacaine and lidocaine for pain control after diagnostic laparoscopy. J Am AssocGynecollaparosc 2003; 10:311-315 [ Links ]
24. Hunter A, Fogarty P. Transcervical analgesia for laparoscopic sterilization. Br J Obst Gynecol. 1996, 103: 378-380 [ Links ]
25. Luscombe FE, Puonder D, Geraghty AV, Bevan JR. Percevicalintrafallopian bupivacaine instillation to reduce postoperative pain after laparoscopic tubal sterilization. Journal of Obstetrics and Gynaecology. 1989, 10: 145-148 [ Links ]
26. Wheatley SA, Millar JM, Jadad AR. Reduction of pain after laparoscopic sterilization with local bupivacaine: randomized, parallel, double-blind trial. British Journal of obstetrics and gynecology 1994; vol 101, 5:443-446 [ Links ]
27. Visalyaputra S, Lertakyamanee J, Pethpaisit N, SomprakitP, Parakkamodom S, Suwanapeum P. Intraperitoneallidocaine decreases intraoperative pain during postpartum tubal ligation. AnesthAnalg 1999; 88:1077-80. [ Links ]
28. Kelly MC. An assessment of the value of intraperitoneal bupivacaine for analgesia after laparoscopic sterilization. BJOG 1996, 103: 837-839. [ Links ]
29. Dionne RA, Khan AA, Gordon SM. Analgesia and COX-2 inhibition. Clin Exp Rheumatol 2001; 19(6 Suppl 25):S63-70. [ Links ]
]]>
30. Knight YE, Goadsby PJ. The periaqueductal grey matter modulates trigeminovascular input: a role in migraine? Neuroscience 2001; 106:793-800. [ Links ]
31. Ashpal K, Fisher K, Chabot J, Coderre TJ. Differential effects of NMDA and group I mGluR antagonists on both nociception and spinal cord protein kinase C traslocation in the formalin test and a model of neuropathic pain in rats. Clin J Pain 2001; 17:178-86. [ Links ]
32. Eastwood JD. The folly of effort: ironic effects in the mental control of pain. Int J ClinExpHypn 1998; 46 :19. [ Links ]
33. Fillingim RB, Maixner W, Kincaid S, Sigurdsson A, Harris MB. Pain sensitivity in patients with temporomandibular disorders: relationship to clinical and psychosocial factors. Clin J Pain 1996; 12:260-9. [ Links ]
34. Field HC. Brainsterm control of spinal pain trasmissor neurons. Ann Rev Physiol 1978;40:217-48. [ Links ]
35. Fillingim RB. Sex differences in temporal summation but not sensory-discriminative processing of thermal pain. Pain 1998; 75:121-7. [ Links ]
36. Foster NE, Baxter F, Walsh D, Baxter GD, Allen JM. Manipulation of transcutaneous electrical nerve stimulation variables has no effect on two models of experimental pain in humans. Clin J Pain 1996; 12:301-10. [ Links ]
37. Stanik-Hutt JA, Soeken KL, Belcher AE, Fontaine DK, Gift AG. Pain experiences of traumatically injured patients in a critical care setting. Am J Crit Care 2001;10 :252-9. [ Links ]
38. Fredman B, Jedeikin R, Olsfanger D, Flor P, Gruzman A. Residual pneumoperitoneum: a cause of postoperative pain after laparoscopic cholecystectomy. Anesth Analg 1994;79: 152–4. [ Links ]