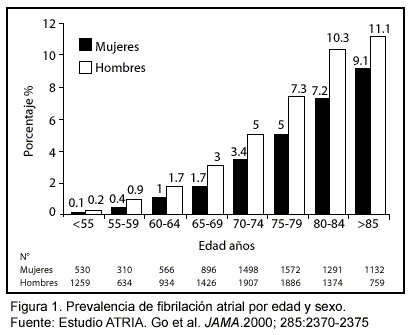
 ]]>
]]>
Fibrilación atrial en los adultos mayores
(Atrial Fibrillation in the Elderly)
Jorge Brizuela-Torres,
Fernando Morales-Martínez
Unidad de Postgrado. Hospital Nacional Geriatría y Gerontología Dr. Raúl Blanco Cervantes. UCR-CENDEISSSCCSS.
Correspondencia: Jorge Brizuela Torres E-mail: jbrizuela5@hotmail.com
Resumen
La fibrilación atrial es la taquiarritmia más prevalente en los adultos mayores. La frecuencia de dicha arritmia aumenta con la edad, presentándose en un 1.5% de los 50 a 59 años a 10% de los 80 a 89 años. La fibrilación atrial no valvular incrementa el riesgo de sufrir un evento cerebrovascular isquémico cardioembólico en 5 veces y causa el 15% de todos los accidentes cerebrovasculares isquémicos en Estados Unidos de América. El manejo de la fibrilación atrial se enfoca, principalmente, en la prevención de los fenómenos tromboembólicos y en el control de la frecuencia y ritmo cardiaco. La anticoagulación, cuando está indicada, ha demostrado ser la principal herramienta en la prevención de dichos eventos. Sin embargo, aunque las complicaciones hemorrágicas son más frecuentes, en esta población, y aumentan con la edad, sobrepasa por mucho, el beneficio al riesgo. El control de la frecuencia cardiaca ha demostrado ser igual o mejor que el control del ritmo en cuanto a prevención de eventos cerebrovasculares y mortalidad en estos pacientes. La edad cronológica por sí sola, no es contraindicación alguna para ofrecer una terapia óptima. Debe tomarse en cuenta el estado funcional, cognitivo y social, así como aspectos fisiológicos del envejecimiento con respecto a la prescripción de medicamentos. Cuando, a pesar del tratamiento adecuado, la sintomatología persiste, las estrategias invasivas han demostrado ser beneficiosas, pero faltan estudios que involucren a individuos mayores.
Descriptores: fibrilación atrial, adulto mayor, anticoagulación, prevención, antiplaquetarios, accidente cerebrovascular.
]]> AbstractAtrial fibrillation is the most prevalent arrhythmia in the elderly. Its frequency increases with age, being 1.5% from 50 to 59 years old and 10% from 80 to 89 years old. Non valvular atrial fibrillation increases 5 fold the risk of suffering an stroke and causes 15% of strokes in the USA. Atrial fibrillation management focuses in the prevention of thromboembolic phenomena and heart rate and rhythm control. Anticoagulation, when indicated, has demonstrated to be the main tool in the prevention of these events.
Nevertheless, although bleeding complications are more frequent in this population and increase with age, anticoagulation benefits are greater than the risks. Heart rate control is better than rhythm control regarding cerebrovascular accidents and mortality. Age by itself is not a contraindication to offer optimal therapy. Functional, mental and social status, must be taken into account as well as physiological aspects of aging when it comes to prescribing medications. If symptoms persist in spite of adequate treatment, invasive strategies have demonstrated to be of benefit, however studies in elderly population are lacking.
Key words: atrial fibrillation, elderly, anticoagulation, prevention, antiplatelet agents, stroke.
Recibido: 8 de agosto de 2008 Aceptado: 3 de febrero de 2009
La fibrilación atrial es, sin duda alguna, la arritmia cardiaca de mayor prevalencia en los adultos mayores, estimándose que el 5% de las personas de 65 años y más, la presentan y un 10% en aquellos mayores de 80 años. (Figura 1).1,2
La prevalencia de la fibrilación atrial está en incremento; en gran parte, por el aumento de la población de 60 años y más en todo el mundo. Como ya es sabido, Costa Rica no se excluye de este fenómeno demográfico. Para el año 2050, se estima que habrá 5.6 millones de personas con fibrilación atrial en los Estados Unidos de América (E.U.A.), de esos, el 50% tendrá 80 o más años.1
La fibrilación atrial no valvular incrementa el riesgo de sufrir un evento cerebrovascular isquémico en 5 veces y causa el 15% de todos los accidentes vasculares cerebrales (AVC) isquémicos en E.U.A. En personas de 80 a 89 años, esto se incrementa aproximadamente, a un 24%.3 Los eventos cerebrovasculares cardioembólicos asociados a la fibrilación atrial tienen una mortalidad del 25% en 30 días, y resultan en mayor discapacidad que los no cardioembólicos.4, 5
Es por eso, que la prevención de los eventos cerebrovasculares en los pacientes portadores de una fibrilación atrial es pilar en el tratamiento de dicha afección, resultando en un impacto importante, en la reducción de costos, en la rehabilitación y ulterior manejo del paciente con secuelas, desde el punto de vista médico, social y mental.4
Los anticoagulantes orales, cuando están indicados, han demostrado ser altamente efectivos en la prevención de dicha catástrofe. Sin embargo, por diversas razones, algunas de estas más mitos que realidades, son poco prescritos en los adultos mayores.6, 7
Uso de la warfarina para prevenir AVC en acianos con fibrilación atrial
En el Hospital Nacional de Geriatría y Gerontología "Dr. Raúl Blanco Cervantes", los pacientes en que se determinó que habían sufrido un AVC isquémico cardioembólico secundario a fibrilación atrial del 2005 al 2006, sólo el 10%, estaban recibiendo un anticoagulante oral y menos de la mitad estaban con niveles óptimos de INR (International Normalized Ratio) en el momento del evento. Por otra parte, de 1998 a 1999 en E.U.A, un estudio de Medicare reportó que solo el 42% de los pacientes portadores de fibrilación atrial, estaban recibiendo warfarina a la hora de darles de alta en distintos hospitales.8 Existe amplia evidencia del beneficio y el uso seguro de la warfarina en los ancianos.9
La warfarina reduce el riesgo relativo de un AVC isquémico en un 62-68% en pacientes con fibrilación atrial y en un 33% la mortalidad por dicha causa.6, 9
La dosis de warfarina, en esta población, ha sido discutida ampliamente y en diversos estudios se ha documentado que los ancianos, por los cambios normales del envejecimiento en cuanto a la farmacocinética y farmacodinamia, requieren menor dosis de inicio y mantenimiento. Un estudio mostró que se debe reducir la dosis de warfarina en 0.4mg/día por cada año después de los 70 años, particularmente, en las mujeres, la dosis debe ser de 3 a 5 mg.10
]]> Independientemente de la dosis de inicio y de mantenimiento, lo crucial es mantener un INR de 2.0 a 3.0. Prescribir dosis menores logrando un INR < 2.0 no brinda protección de sufrir un AVC y no disminuye el riesgo de hemorragia intracraneal.11,12 También, el riesgo de sangrado es mayor proporcionalmente, al aumento de los niveles de INR sobre 4.0.6,14Los estudios no proveen evidencia clara sobre la frecuencia en que se debe controlar el INR en estos pacientes. La Sociedad Americana de Geriatría recomienda control diario hasta que se estabilicen los niveles de 2.0 a 3.0 en al menos dos ocasiones consecutivas, luego 2 a 3 veces por semana durante 2 semanas luego, semanalmente, por un mes y por último, mensualmente. Quizá uno de los más grandes retos es el lograr un apego a los controles debido al poco acceso de laboratorios disponibles, en el primer y segundo nivel de atención en el país, así como el estado físico, funcional, mental y social de los pacientes y la disponibilidad de los cuidadores. La educación, en este sentido, es fundamental.13
El riesgo de hemorragia asociado a la warfarina se incrementa con la edad. La tasa anual de sangrado en diversos estudios varía desde un 0.3% a 10%.15, 16
En un gran estudio de cohorte en pacientes con fibrilación atrial, que estaban anticoagulados, se demostró que la tasa de hemorragia intracraneana fue de 0.47% y de hemorragia extracraneana del 0.64% anual lo que significa decir que por 1 año de terapia con warfarina, se estima 1 a 2 hemorragias intracraneanas por cada 1000 pacientes. (Figura 2).17
Se han identificado diversos factores de riesgo asociados a sangrado mayor que deben tomarse en cuenta en el adulto mayor: AVC previo, sangrado digestivo previo, hipertensión arterial, uso concomitante de aspirina, anemia, insuficiencia renal crónica, enfermedades neuropsiquiátricas, polifarmacia (> de 5 medicamentos), falta de educación y cáncer, todas muy frecuentes en esta población.18,19
Antiplaquetarios en la prevención de AVC en ancianos con fibrilación atrial
Si la warfarina está contraindicada o el paciente es de bajo riesgo, los antiplaquetarios también han demostrado ser beneficiosos en prevenir los eventos isquémicos cerebrovasculares cardioembólicos.20
La aspirina reduce el riesgo de AVC en un 21% y tiene menos complicaciones hemorrágicas que la warfarina. Algunas ventajas de esta sobre la warfarina es su costo, amplia disponibilidad, posee una vasta ventana terapéutica, menos interacciones droga-droga, dieta-droga y no necesita monitoreo. Debe tomarse en cuenta los sangrados digestivos y los efectos secundarios gastrointestinales en los adultos mayores. Un reciente estudio demostró que los pacientes entre 80 y 90 años abandonan, con mayor frecuencia, la aspirina que la warfarina precisamente, por los efectos secundarios reportados.20, 21
El uso de la warfarina es superior al de aspirina combinada con clopidogrel, en la prevención de eventos cerebrovasculares en pacientes con FA, con similares tasas de eventos hemorrágicos en ambos grupos, demostrado en el estudio ACTIVE-W (Atrial fibrillation clopidogrel trial with Irbesartan for prevention of Vascular Events). El uso de clopidogrel solo, no es superior que la aspirina o la warfarina.21, 22
Otros antitrombóticos han sido estudiados, como el inhibidor directo de trombina, el ximelagatran, demostró ser, al menos, igual de eficaz que la warfarina en la prevención de AVC, pero nunca fue lanzado al mercado por su toxicidad hepática. El idraparinux, un inhibidor directo del factor Xa así como el apixaban y rivoroxaban se encuentran en estudios, así que por el momento no existe otro antitrombótico que sea superior a la warfarina en la prevención de eventos cerebrovasculares en ancianos con FA. 22,23
Anticoagulación basada en la evidencia y en la estratificación del riesgo
Los ancianos reciben menos prescripción de anticoagulantes y cuando se les anticoagula, se hace de manera subterapéutica, a pesar de que tengan criterios para recibir dicha terapia. Algunos de los factores que influyen en esta omisión terapéutica, inciden en el temor de algunos médicos de recetar warfarina por creencias infundadas, como lo es el riesgo de un anciano a caerse y desarrollar grandes hematomas o trauma craneoencefálico, el antecedente de sangrado previo, demencia y la poca adherencia al tratamiento. Como se apreció, en el Hospital Nacional de Geriatría y Gerontología y en otras partes del mundo, existe una tendencia de no ofrecer el beneficio de la anticoagulación plena cuando esta se encuentra indicada y menos de la mitad de estos pacientes están anticoagulados de manera óptima. 24-27
Pocos estudios han logrado cuantificar el riesgo absoluto asociado a las caídas y la warfarina, en parte porque la mayoría de estos, excluyen a pacientes con riesgo de caerse. Uno de los estudios más influyentes en la decisión de anticoagular a estos pacientes, demostró que es necesario caerse 300 veces al año para que la warfarina no se indique como tratamiento de elección cuando así se requiera.28 Por otra parte, un estudio documentó que los pacientes con alto riesgo de caídas, pero bajo riesgo de presentar un evento cerebrovascular isquémico tromboembólico, no se ven beneficiados con el uso de warfarina.29
]]> La warfarina incrementa el riesgo en un 25% de sufrir fracturas patológicas ya que disminuye la densidad mineral ósea. En este estudio se demostró que el deterioro cognitivo y las enfermedades neuropsiquiátricas también son factores de riesgo para fracturas, por lo que se hace énfasis en la importancia de analizar el estado cognitivo y funcional de los pacientes a los que se les prescribe warfarina.29, 38Existen algunos índices de evaluación de riesgo para sufrir un evento cerebrovascular isquémico en los ancianos con FA. El más validado por la mayoría de autores es el índice de CHADS2 (Congestive heart failure, Hipertensión, Age > 75 años, Diabetes Mellitus, prior Stroke/transient ischemic attack).30-32 Este índice muestra el riesgo anual de presentar un AVC en pacientes portadores de FA que no reciben anticoagulación, el cual varía de < 1% con solo un punto a 20% en aquellos que tienen al menos un puntaje de 6. 32 (Cuadro 1 y Figura 3)
Control farmacológico de la frecuencia y el ritmo cardiaco en los ancianos
Algunos estudios recientes han demostrado que el control del ritmo cardiaco no es superior al control de la frecuencia en el manejo de la FA en cuanto a mortalidad o aparición de AVC. Además los fármacos antiarrítmicos no previenen los eventos cerebrovasculares ni evitan la indicación de anticoagulación. De hecho, el control del ritmo cardiaco se ha asociado a un aumento, en la mortalidad, en el adulto mayor.34-37
Un reciente metaanálisis evidenció que la incidencia de AVC isquémico entre los pacientes en que se controló el ritmo con los que se controló la frecuencia cardiaca fue similar (3.35% vs 3.9% respectivamente, OR=0.50, IC=95%).41 (Figura 4)
Los betabloqueadores, los calcioantagonistas no dihidropiridínicos y la digoxina, son los fármacos mayormente recomendados y utilizados para controlar la frecuencia cardiaca en la fibrilación auricular, pero todos ellos pueden inducir bradicardia o bloqueos de la conducción atrioventricular en los ancianos.37 (Cuadro 5 y 6)
La amiodarona, un antiarrítmico de clase III de Vaugham Williams, ha demostrado ser la droga más efectiva para mantener el ritmo sinusal. El 30% de los pacientes, con la dosis de carga, lo logran, a pesar de ser recomendación Iia por la Asociación Americana del Corazón.50 Su metabolito activo, la desetilamiodarona metabolizada en el hígado, bloquea los canales de sodio, potasio y calcio, así como un relativo alfa y betabloqueo a nivel de los miocitos cardiacos. El más significativo es el bloqueo de los canales de potasio que enlentece la repolarización, prolongando el QT y previene el remodelado eléctrico del miocardio.
Su gran volumen de distribución, por ser lipofílica, es de aproximadamente 66 litros por kilogramo de peso corporal, aspecto a tomar en cuenta ya que en el anciano aumenta en un 20% a 40% la grasa corporal total y disminuye en un 10%-15% el agua corporal total.43 Su inicio de acción es de 2-3 días y tiene una eliminación media de hasta 6 meses. No se ve alterada por la función renal y es especialmente útil en pacientes con alteración estructural del corazón o en aquellos que tienen insuficiencia cardiaca.44
La dosis inicial es de 400 mg dos veces al día durante 2 semanas hasta acumular una dosis de 10 gr, seguida de 400 mg por día por 2 semanas más para luego continuar con 200 mg vía oral por día de mantenimiento. (Cuadros 2, 3, 4).
En el anciano no deben variar las dosis de carga por el aumento en la grasa corporal descrito anteriormente sin embargo, aunque no hay estudios al respecto, se recomienda que la dosis de mantenimiento en algunos ancianos, sobre todo aquellos que tienen un IMC < 18 Kg/m2, sea de 100 mg por día, aunado a la disminución del metabolismo hepático de fase I y por la relativa disminución de la albúmina sérica en estos pacientes, haciéndolos más susceptibles a bradicardias, por lo que si el QT se prolonga por más de 550 mseg, debe reducirse la dosis.43
El efecto indeseado más común en los ancianos es la bradicardia, el hipotiroidismo se presenta en un 20%, no debe suspenderse el fármaco y puede agregarse levotiroxina si se requiere.45 El Hipertiroidismo varía de un 3% a un 20%, se debe descontinuar la amiodarona si este se presenta. Los niveles de T4 libre y TSH deben medirse al inicio y cada 6 meses.
]]> La toxicidad pulmonar es la complicación más seria y se presenta en un 3%, es dosis dependiente y su aparición requiere retirar el medicamento. Pruebas de función pulmonar y la radiografía de tórax deben realizarse al inicio de la terapia y anualmente.45,46 La toxicidad hepática, una esteatohepatitis no alcohólica, es asintomática y se manifiesta por elevación de dos veces los valores de las transaminasas, que puede resultar en cirrosis hepática si no se descontinúa la ingesta de amiodarona, aparece en un 15%. Deben solicitarse las pruebas de función hepática al menos cada seis meses. Los efectos dermatológicos aparecen en un 25%- 75% con fotosensibilidad por lo que debe evitarse la exposición al sol. Los pacientes expuestos a la amiodarona por largos períodos de tiempo pueden aquejar una coloración grisácea difusa y alopecia.47 Microdepósitos cornéales aparecen en todos los pacientes sin tener repercusiones clínicas; la neuropatía óptica aparece en menos del 1% y es razón para suspender la amiodarona.44,46Ataxia, tremor, polineuropatía, insomnio y deterioro en la memoria, son efectos neurológicos que se presentan hasta en un 30% y es dosis dependiente. En general, los efectos adversos pueden persistir hasta en un 13%-18% un año después de descontinuar la amiodarona.48Otras contraindicaciones para el uso de dicho fármaco son: disfunción del nodo y bloqueos atrioventriculares de alto grado (excepto los que tienen marcapaso artificial funcionante). La dosis de warfarina debe reducirse en un 25% con el uso concomitante de la amiodarona debido a la interacción de ambos, en el metabolismo hepático en el citocromo P450-2C9.49
La dronedarona, un derivado benzofurano recientemente desarrollado, con propiedades electroestructurales similares a la amiodarona pero con un radical iodínico menos, que busca reducir o eliminar la pneumo y tirotoxicidad, actua bloqueando canales de sodio, calcio, potasio y también tiene efectos antiadrenérgicos, con una vida media de 1 a 2 días comparado con la amiodarona que es de 30 a 55 días.
Algunos estudios recientes sugieren que la dronedarona tiene un impacto en la morbimortalidad relacionada con la fibrilación atrial, como lo demostraron los meta-análisis EURIDIS (European Trial in Atrial Fibrillation Patients Receiving Dronedarone for the Maintenance of Sinus Rythm), y el estudio ADONIS (American-Australian Trial With Dronedarone in Atrial Fibrillation Patients for the Maintenance of Sinus Rythm); ambos mostraron una reducción de la tasa de recurrencia de episodios de fibrilación atrial a 12 meses de seguimiento de 67.1% y 61.1% con dronedarona versus 77.5% y 72.8% con placebo respectivamente.50,51
Estos beneficios se confirmaron más recientemente, con el estudio doble ciego controlado con placebo: ATHENA; realizado en 551 centros de 37 países alrededor del mundo, en donde se randomizaron sujetos mayores de 70 años, portadores de fibrilación atrial paroxística o persistente asociado a un moderado/alto riesgo cardiovascular el cual mostró una reducción del 24% en el riesgo de hospitalización o muerte cardiovascular en los sujetos que recibieron dronedarona 400 mg BID, así como una reducción del 45% en la mortalidad asociada a arritmias y sin efectos secundarios superiores al placebo, por lo que parece ser una buena opción para evitar los efectos adversos de la amiodarona y se perfila a jugar un rol protagónico en el manejo de pacientes portadores de fibrilación atrial en el corto plazo.52
La digoxina debe usarse con precaución por su toxicidad, estrecha ventana terapéutica y múltiples interacciones con otros medicamentos, sobre todo en los pacientes con falla renal. Su principal indicación es en el control de la frecuencia en los pacientes con insuficiencia cardiaca o disfunción del ventrículo izquierdo. La digoxina reduce la frecuencia cardiaca en reposo pero no así en la actividad física.49 La dosis habitual es de 0.125mg a 0.5 mg por día vía oral. (Cuadros 5 y 6) Un estudio reciente sugiere que mantener niveles séricos de 0.09 ng/ml es efectivo para reducir la tasa de eventos vasculares.53 No existen recomendaciones avaladas por las diferentes autoridades mundiales para que se dosifique de lunes a viernes y no se administren las dosis correspondientes a los fines de semana en los ancianos, práctica muy común en nuestro medio.49 Lo más importante es cuantificar los niveles de manera periódica para mantenerlos dentro del rango terapéutico (0.2-2 ng/ml).53Las diferentes presentaciones de digoxina en la CCSS son: tabletas de 0.25 mg, frasco al 0.075% o 0.75mg/ml o sea cada gota contiene 16.6 mcgr y ampollas de 1 ml con 0.25 mg/ml.54
Las Guías de Práctica Clínica Americanas recomiendan que el objetivo en el control de la frecuencia cardiaca en estos pacientes debe ser de 60-80 latidos por minuto en reposo y de 90 a 115 latidos durante la actividad física moderada.49
Tratamiento invasivo en ancianos con fibrilación atrial
Los pocos estudios que involucran el manejo invasivo para controlar la frecuencia y el ritmo cardiaco, en el adulto mayor, incluyen algunas estrategias como la ablación del nodo atrioventricular con implantación de marcapaso, ablación focal de las venas pulmonares con catéter de radiofrecuencia y el procedimiento de Cox-Maze III.
Cuando están indicados, estos procedimientos han demostrado ser más efectivos que los agentes farmacológicos, sobre todo en pacientes que persisten sintomáticos a pesar del tratamiento médico óptimo.55, 57
La ablación del nodo atrioventricular se realiza mediante ablación transvenosa con radiofrecuencia del nodo AV y colocación de marcapaso atrial o bicameral, resultando en un bloqueo completo y control de la frecuencia. En un estudio de 350 pacientes (edad promedio 68±11 años), la supervivencia no fue inferior a la de aquellos pacientes controlados con tratamiento óptimo. La anticoagulación debe persistir a pesar de dicha estrategia.55 La ablación percutánea con catéter de radiofrecuencia permite realizar la ablación transvenosa en los focos de ectopia, los cuales se considera que se encuentran ubicados en un 80% al 90% en las venas pulmonares, seguidos de las venas cavas, los atrios y el seno coronario.56-58
Las tasas de éxito son del 78% al 85% con un rango de complicaciones entre el 1% y el 5% en centros experimentados.59 Aún no está claro si la anticoagulación debe continuarse luego de este procedimiento sin embargo, la mayoría de los estudios se han efectuado en pacientes menores de 65 años sin patología estructural cardiaca y sin comorbilidades.60 La cirugía de Cox-Maze III consiste en realizar incisiones en el atrio, eliminando los apéndices auriculares, aislando las venas pulmonares y posterior reconstrucción del atrio. Tiene una tasa de curación en un 90% a 10 años plazo, con una mortalidad del 2% al 3% perioperatoria.61
Conclusión
]]> La fibrilación atrial es la arritmia más frecuente en el adulto mayor y es un importante factor de riesgo para desencadenar una catástrofe tromboembólica, resultando en un accidente cerebrovascular isquémico. Los que sobreviven a dicho evento, arrastrarán las secuelas físicas, mentales, funcionales y sociales, así como sus familias y cuidadores. Actualmente, existe evidencia clara sobre las pautas que se deben asumir en el manejo óptimo y oportuno de la fibrilación atrial, enfocado principalmente, en la prevención del fenómeno tromboembólico y en el control de la frecuencia cardiaca. Aunque son relativamente pocos los estudios en los ancianos, no existe contraindicación absoluta para privar a estos pacientes, solo por la edad cronológica, de ofrecer el beneficio de la terapia recomendada siempre y cuando se individualice, integralmente, cada paciente.Abreviaturas: AAS, ácido acetil salicílico; CCSS, Caja Costarricense del Seguro Social; AIT, accidente isquémico transitorio; AVC, accidente vascular cerebral; FC, frecuencia cardiaca; FE, fracción de eyección del ventrículo izquierdo; HTA, hipertensión arterial; ICC, insuficiencia cardiaca congestiva; INR, international normalized ratio.
Referencias
1. Go AS, Hylek EM, Phillips KA. Prevalence of diagnosed atrial fibrillation in adults: national implications for rhythm management and stroke prevention: The Anticoagulation and Risk factors in Atrial Fibrillation (ATRIA) Study. JAMA. 2000; 285:2370-2375. [ Links ]
2. Wolf PA, Abbott RD, Kannel WB. Atrial fibrillation as an independent risk factor for stroke: The Framingham Study. Stroke1991;22:983-988. [ Links ]
3. Lakshminarayan K, Solid CA, Collins AJ. Atrial fibrillation and stroke in general medicare population: a 10 year perspective (1992-2002). Stroke.2006;37:1969-1974. [ Links ]
4. Lin HJ, Wolf PA, Kelly Hayes M. Stroke severity in atrial fibrillation. The Framinghan Study. Stroke 1996;27:1760-4. [ Links ]
5. Hylek EM, Go AS, Chang Y. Effect of intensity of oral anticoagulation on stroke severity and mortality in atrial fibrillation. N Engl J Med 2003;349:1019-26. [ Links ]
6. Hart R, Benavente O, McBride R. Antithrombotic therapy to prevent stroke in patients with atrial fibrillation: a meta-analysis. Ann Intern Med 1999;131:492-501. [ Links ]
7. Mccrory DC, Matchar DB, Samsa G. Physician attitudes about anticoagulation for nonvalvular atrial fibrillation in the elderly. Arch Intern Med 1995; 155:277-81. [ Links ]
8. Jencks SF, Cuerdon T, Burwen DR. Quality of medical care delivered to Medicare beneficiaries: a profile at state and national levels. JAMA 2000;284:1670-6. [ Links ]
9. David A. Garcia MD, Elaine Hylek. Reducing the risk for stroke in patients who have atrial fibrillation. Cardiol Clin 2008:267-275. [ Links ]
10. Garcia D, Regan S, Crowther M. Warfarin maintenance dosing patterns in clinical practice: implications for safer anticoagulation in the elderly population. Chest 2005;127:2049-2056. [ Links ]
11. Hylek EM, Skates S, Sheehan M. An analysis of the lowest effective intensity of prophylactic anticoagulation for patients with nonrheumatic atrial fibrillation. N Engl J Med.1996:335:540-546. [ Links ]
12. Fang MC, Chang Y, Hylek EM. Advanced age, anticoagulation intensity and risk for intracranial hemorrhage among patients taking warfarin for atrial fibrillation. Ann Intern Med. 2004;141:745-752. [ Links ]
13. American Geriatrics Society Clinical Practice Committee. The use of oral anticoagulants (warfarina) in older people. American Geriatrics Society Guideline. J AM Geritr Soc. 2002;50:1439-1445. [ Links ]
14. Palareti G, Leali N, Coccheri S. Bleeding complications of oral anticoagulant treatment: an inception cohort, prospective collaborative study (ISCOAT). Italian Study on Complications of Oral Anticoagulant Therapy. Lancet 1996;348:423-8. [ Links ]
15. Fanikos J, Grasso-Correnti N, Shah R. Major Bleeding complications in a specialized anticoagulation service. Am J Cardiol.2005;96:595-598 [ Links ]
16. Landefeld CS, Goldman L. Major bleeding in outpatients treated with warfarin: incidence and prediction by factors known at the start of outpatient therapy. Am J Med. 1989;87:144-152. [ Links ]
17. Fang MC, Go AS, Hylek EM. Age and the risk of warfarin associated hemorrhage: the Anticoagulation and Risk Factors In Atrial Fibrillation (ATRIA) Study. J Am Geritr Soc. 2006;54:1231-1236. [ Links ]
18. Levine MN, Raskob G, Beyth RJ. Hemorrhagic complications of anticoagulant treatment: the Seventh ACCP Conference on Antithrombotic and Thrombolitic Therapy. Chest. 2004; 126:287S- 310S [ Links ]
19. Kagansky N, Knobler H, Rimon E. Safety of anticoagulation therapy in well informed old patients. Arch Intern Med. 2004;164:2044- 2050. [ Links ]
20. vanWalraven C, Hart RG, Singer DE. Oral anticoagulants vs aspirin in nonvalvular atrial fibrillation: an individual patient metanalysis. JAMA. 2002;288:2441-2448. [ Links ]
21. Rash A, Downes T, Portner R. A randomized controlled trial of warfarin vs aspirin for stroke prevention in octogenarians with atrial fibrillation (WASPO). Age and Ageing.2006;afl 129. [ Links ]
22. Olsson S, Executive Steering Committee on behalf of the SPORTIF III Investigators. Stroke prevention with the oral direct thrombin inhibitor ximelagatran compared with warfarin in patients with nonvalvular atrial fibrillation (SPORTIF III): randomized controlled trial. Lancet 2003;362:1691-1698. [ Links ]
23. SPORTIF executive Steering Committee for the SUPORTIF V Investigators. Ximelagatran vs warfarin for stroke prevention in patients with nonvalvular atrial fibrillation: a randomized trial. JAMA. 2005;293:690-698. [ Links ]
24. McCrory DC, Matchar DB, Samsa G. Physician attitudes about anticoagulation for novalvular atrial fibrillation in the elderly. Arch Intern Med. 1995;155:27-281. [ Links ]
25. Quilliam BJ, Lapane KL. Clinical correlates and drug treatment of residents with stroke in long term care. Stroke. 2001;32:1385-1393 [ Links ]
26. McCormick D, Gurwitz JH, Goldberg RJ. Prevalence and quality of warfarin use for patients with atrial fibrillation in long term care setting. Arch Intern Med.2001;161:2458-2463. [ Links ]
27. Fang MC, Stafford RS, Ruskin JN. National trends in antiarrhythmic and antithrombotic medication use in atrial fibrillation. Arch Intern Med.2004;164:55-60. [ Links ]
28. Man-Son-Hing M, Nichol G, Lau A, Laupacis A. Choosing antithrombotic therapy for elderly patients with atrial fibrillation who are at risk for falls. Arch Intern Med.1999;159:677-685. [ Links ]
29. Gage BF, Birman-Deych E, Kerzner R. Incidence of intracranial hemorrhage in patients with atrial fibrillation who are prone to fall. Am J Med.2005;118:612-617 [ Links ]
30. Hart R, Pearce L, MacBride R. Factors associated with ischemic stroke during aspirin therapy in atrial fibrillation: analysis of 2012 participants in the SPAF I-III clinical trials. Stroke. 1999;30:1223-1229. [ Links ]
31. Fang MC, Singer DE, Chang Y. Gender differences in the risk of ischemic stroke and peripheral embolism in atrial fibrillation (ATRIA) study. Circulation. 2005;112:1687-1691. [ Links ]
32. Gage BF, Waterman AD, Shannon W. Validation of clinical classification schemes for predicting stroke: results from the National Registry of Atrial Fibrillation. JAMA. 2001;285:2864-2870. [ Links ]
33. Go AS, Hylek EM, Chang Y. Anticoagulation therapy for stroke prevention in atrial fibrillation: how well do randomized trials translate into clinical practice?. JAMA. 2003; 290: 2685-2692. [ Links ]
34. AFFIRM Investigators: A comparison of rate control and rhythm control in patients with atrial fibrillation. N Engl J Med. 2002; 347:1825-1833. [ Links ]
35. Van Gelder I.C., Hagens V.E., Bosker H.A. A comparison of rate control and rhythm control in patients with recurrent persistent atrial fibrillation. N Engl J Med .2002; 347:1834-1840. [ Links ]
36. Alpert MA. Medical cardioversion of atrial fibrillation. Chest 2000;117:1530-31. [ Links ]
37. Hohnloser SH, Kuck K, Lilienthal J. Rhythm or rate control in atrial fibrillation-pharmacological intervention in atrial fibrillation (PIAF): a randomized trial. Lancet 2000; 356:1789-94. [ Links ]
38. Tsivgoulis G, Spengos K, Zacopoulos N. Efficacy of anticoagulation for secondary stroke prevention in older with non-valvular atrial fibrillation: a prospective case series study. Age and Ageing 2005; 34: 35-40. [ Links ]
39. Hart RG, Pearce LA, Rothbart RM. Stroke with intermittent atrial fibrillation: incidence and predictors during aspirin therapy. J Am Coll Cardiol 2000; 35; 183-7. [ Links ]
40. de Denus S., Sanoski C.A., Carlsson J. Rate vs rhythm control in patients with atrial fibrillation: a meta-analysis. Arch Intern Med 2005; 165: 258-262. [ Links ]
41. Echt DS, Liebson PR, Mitchell LB. Mortality and morbidity in patients receiving encinide, flecainide or placebo. The cardiac arrhythmia suppression Trial. N Engl J Med. 1991; 324: 781-88. [ Links ]
42. Allan J, McLean G, McLean D. Aging Biology and Geriatric Clinical Pharmacology. Pharmacol Rev 2004; 56: 163-184. [ Links ]
43. Zimetbaum P. Amiodarone for Atrial Fibrillation. N Engl J Med 2007; 356: 935-941. [ Links ]
44. Goldschlager N, Epstein AE, Naccarelli G. Practical Guidelines for clinicians who treat patients with amiodarone. Arch Inter Med 2000; 160: 1741-8. [ Links ]
45. Olshansky B, Sami M, Rubin A. Use of amiodarone for atrial fibrillation In patients with preexisting pulmonary disease in the AFFIRM study. Am J Cardiol 2005; 95: 404-5. [ Links ]
46. Ahmad S. Amiodarone and reversible alopesia. Arch Intern Med 1995; 155: 1106. [ Links ]
47. Singh BN, Singh SN, Reda DJ. Amiodarone vs Sotalol for atrial fibrillation. N Engl J Med 2005; 352:1861-72. [ Links ]
48. Jacobs LG. Warfarin Pharmacology, Clinical management and evaluation of hemorrhagic risk for the elderly. Cardiol Clin 2008; 26:157-167. [ Links ]
49. Fuster V., Ryden L.E., Cannom D.S. ACC/AHA/ESC 2006 Guidelines for the Management of Patients with Atrial Fibrillation: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the European Society of Cardiology Committee for Practice Guidelines (Writing Committee to Revise the 2001 Guidelines for the Management of Patients With Atrial Fibrillation): developed in collaboration with the European Heart Rhythm Association and the Heart Rhythm Society. Circulation 2006; 114:257-354. [ Links ]
50. Singh B, Connolly SJ. Dronedarone for maintenance of sinus rhythm in atrial fibrillation or flutter. N Engl J Med. 2007; 357:987-999. [ Links ]
51. Hohnloser S. EURIDIS and ADONIS: Maintenace of sinus rhythm with dronedarone in patients with atrial fibrillation or flutter. Program and abstracts from European Society of Cardiology Congress 2004; August 28-September 1,2004 [ Links ]
52. Hohnloser S, Crijns HJ, van Eickels M. The ATHENA trial: Effects of dronedarone on cardiovascular hospitalization and death in patients with atrial fibrillation or flutter. Program and abstracts from Heart Rhythm 2008: The Heart Rhythm Society (HRS) Annual Scientific Sessions, May 14-17,2008, San Francisco, California [ Links ]
53. Adams KF, Gheroghiade M, Uretzky BF. Clinical benefits of low serum digoxin concentrations in heart failure. J Am Coll Cardiol 2002; 39: 946-53. [ Links ]
54. Comité de Farmacoterapia. Lista Oficial de Medicamentos (LOM). Costa Rica. Caja Costarricense del Seguro Social (CCSS), 2006: 86. [ Links ]
55. Ozcan C., Jahangir A., Friedman P.A. Long-term survival after ablation of the atrioventricular node and implantation of a permanent pacemaker in patients with atrial fibrillation. N Engl J Med 2001; 344:1043-1051. [ Links ]
56. Haissaguerre M., Jais P., Shah D.C. Spontaneous initiation of atrial fibrillation by ectopic beats originating in the pulmonary veins. N Engl J Med .1998; 339: 659-666. [ Links ]
57. Wazni O.M., Marrouche N.F., Martin D.O. Radiofrequency ablation vs antiarrhythmic drugs as first-line treatment of symptomatic atrial fibrillation: a randomized trial. JAMA 2005; 293: 2634-2640. [ Links ]
58. Peters NC, Schilling RJ, Karagaratman PV. Atrial fibrillation: strategies to control, combat and cure. Lancet 2002; 359: 593-603. [ Links ]
59. Pappone C., Oral H., Santinelli V. Atrio-esophageal fistula as a complication of percutaneous transcatheter ablation of atrial fibrillation. Circulation 2004; 109: 2724-2726. [ Links ]
60. Oral H., Pappone C., Chugh A. Circumferential pulmonary-vein ablation for chronic atrial fibrillation. N Engl J Med 2006; 354: 934-941. [ Links ]
61. Ad N., Cox J.L. Stroke prevention as an indication for the Maze procedure in the treatment of atrial fibrillation. Semin Thorac Cardiovasc Surg 2000; 12: 56-62. [ Links ] ]]>