Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Acta Médica Costarricense
On-line version ISSN 0001-6002Print version ISSN 0001-6012
Acta méd. costarric vol.54 n.1 San José Jan./Mar. 2012
Clinical Case
Acute Lyme Disease in Costa Rica. Description of the first autochthonous case.
Enfermedad de Lyme aguda en Costa Rica. Descripción del primer caso autóctono
1 Infectology Service
2 Microbiology Division, Clinical Laboratory, Hospital México, CCSS.
Abbreviations: LD, Lyme Disease; USA, United States of America
Correspondence:
Abstract
This is the case of a 44-year-old patient, who lives in Santa Teresa, Puntarenas; with acute onset of fever, chills, severe arthralgias and malaise, 15 days after a tick bite. The indirect fluorescent antibody test for Lyme was positive and the patient improved with doxycicline for 14 days. Other infectious and noninfectious diseases were ruled out; we consider this case as the first autochtonous case of Lyme disease in Costa Rica.
Keywords: Lyme Disease, Costa Rica
LD in humans is associated with acute and chronic manifestations with a variable degree, affecting the osteomuscular, cardiac and nervous systems.
In Costa Rica there are no known autochthonous cases of LD, and the previously seen cases in the country were "imported" cases from the US. We present the first case of autochthonous LD described in Costa Rica.
Case report
A 40 year-old male patient, born in Italy but living in Santa Teresa of Puntarenas for the last 16 years, business man without any past history of illness. The patient's work activities required him to go horseback-riding very often, thus, exposing himself permanently to insect bites, like mosquito and tick bites.
The patient left Costa Rica for the last time 14 months prior to the symptom onset, visiting the US east coast and Milan (Italy) for a 30 day period, not leaving the Santa Teresa and Cóbano regions afterwards.
On early September 2009, he found a tick sticked to his leg's skin for an unknown period of time. He did not remember having any other cutaneous lesions. Fifteen days later he started with chills, fever of up to 39-40 degrees Celsius, malaise, intense joint pain and cramps. After 7 days of persisting symptoms he consulted at the local clinic where he was prescribed with doxycycline 100 mg twice a day, without a precise diagnosis. Two days after, because of the symptom persistence, he arrived at México Hospital. There, an acutely ill, feverish, without tachycardia, mildly dehydrated patient was found, without pathologic findings at the physical examination.
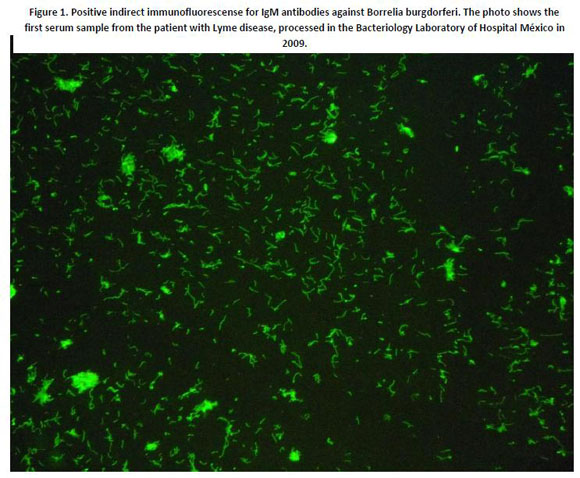
The peripheral blood smears and serology (IgG and IgM) were negative for ehrlichiosis, serology (IgM) for Rickettsia rickettsii and leptospirosis were negative, as so were the VDRL, HIV ELISA and the Epstein Barr virus monotest. Indirect immunofluorescence (Scimedex®) for Borrelia burgdorferi was performed and tested positive for both IgM and IgG. It was controlled three times with a 15 to 22 day interval, showing a progressive decrease in the IgM titer with increase in IgG (figure 1). The patient presented full recovery of clinical signs and symptoms within 5 days of initiating doxycycline, which was prescribed for 14 days. With this information the diagnosis of Lyme Disease or acute borreliosis was made, being this the first autochthonous case in Costa Rica. There were no cardiovascular acute complications, ruled out with a normal electrocardiogram.
Discussion
LD was initially described in Europe, but it was not until the late 70's early 80's (in the city of Old Lyme, Connecticut, USA), that the etiologic agent was discovered to be the Borrelia burgdorferi spirochete.
For the USA, the hard tick Ixodes scapularis is the vector, Ixodes ricinus in Europe and Ixodes persulcatus for Asia, which has a 2 year life cycle with four evolutive stages: egg, larva, nymph and adult. Larva feed of blood of small vertebrates like rodents and birds (considered reservoirs for the spirochete), and in superior stages, they feed from superior mammals like deers and men, with the possibility of transmitting Borrelia. For transmission to be effective the tick has to be adhered to its host at least 36 hours.
There are 12 species of this Gram negative spirochete, forming the Borrelia burgdorferi sensu lato (s.l.) complex, of which Borrelia burgdorferi sensu stricto (s.s.), Borrelia garinii and Borrelia afzelii are the pathogenic species for men. When this microorganism is inoculated, it has a very fast hematogenous dissemination, with predilection for nervous, cardiac, skins and joint tissues. This apparent tissue tropism depends on the infective species, which explains the wide spectrum of manifestations attributed to the disease and the relative geographical predominance of some of them. The disease has three presentations: early localized, early disseminated and late persistent. The most common early form of presentation is the disseminated form that produces signs and symptoms of systemic affection, such as fever, headache, myalgias, arthralgias and malaise, which in 80% of the cases is accompanied by a red papule or spot where the tick bit the patient, which then expands leaving a pale central circle, also known as erythema migrans. These initial symptoms appear after a variable incubation period of some days up to 8 weeks. If the acute presentation lacks systemic symptoms and has only cutaneous manifestations, it is known as early localized.
Early disseminated LD can affect the heart, leading to carditis, which manifests itself most frequently with an atrioventricular block, although other conduction anomalies may occur, like myocarditis, pericarditis and even miocardiopathy in the late persistent form.
Persistent late LD is the chronic form and also shows cutaneous manifestations such as chronic erythema migrans, lymphocytoma cutis and acrodermatitis chronica atroficans. Other chronic manifestations of interest are joint manifestations, presenting generally as big joint mono arthritis, affecting mostly the knee joint, and in some cases even temporomandibular affection has been reported.
In Europe, neurologic pathology is the most seen, and it can lead to an acute meningoradiculoneuritis, with involvement of cranial nerves, lymphocytic meningitis and intense radicular pain; also known as Garin-Boujadoux-Bannwarth syndrome. In the chronic phase, it produces meningoencephalitis, cranial nerve involvement, peripheral neuropathy and variable cognitive impairment. It is important to mention that neurologic manifestations are the least frequent amongst the mentioned. Recently, LD has been associated with depression, anxiety, chronic fatigue syndrome and fibromyalgia; all of them predominantly affecting women.
The diagnosis of the early form requires an elevated clinical suspicion, plus a compatible epidemiological history and a suggestive clinical scenario; and in the chronic form the suspicion index is lower, especially in low-incidence countries like Costa Rica. In high-incidence countries the diagnosis can be made only with clinical data, but in our environment, the infection has to be documented with complementary laboratory tests. The spirochete can be isolated from cutaneous lesions and rarely from cerebrospinal or joint fluids with the Barbour-Stoenner-Kelly media culture; but it is a complex process that could last up to 12 weeks. Diagnosis can also be made by detecting nucleic acids with the Polymerase Chain Reaction, although the test is expensive and of variable sensitivity. This explains why the indirect confirmation method of antibody detection is the gold standard, also being less expensive, less complex and with higher sensibility than the other tests mentioned. For this purpose, IgG and IgM antibodies against highly immunogenic bacterial proteins are detected with indirect immunofluorescence or ELISA tests, and then confirmed with a Western Blot, according to international recommendations. In the early phase of LD there could be no IgM antibodies, leading to a false negative, nevertheless, other pathologies like mononucleosis, syphilis, leptospirosis and autoimmune diseases can lead to false positive results because of crossed reactivity of the antigens.
The antibiotic treatment of LD is indicated in every clinical stage of the disease, although it is more effective during the early stages, preferring doxycicline 100 mg twice a day oraly during 14 days. Alternative regimens include amoxicillin for 14 days and azithromycin for 5 days, both in the usual doses. In every case, it is enough to extend the oral regimen for 14 days, except for when there is central nervous system or cardiovascular compromise, in which case the recommendation is to extend the oral administration for 14 to 22 days. In case intravenous therapy is required, sodium penicillin, ceftriaxone or cefotaxime are recommended.
In the case previously presented, the differential diagnoses includes acute febrile pathologies that can lead to joint compromise, but the history of the tick bite guides us into a group of zoonoses that include ehrlichiosis and rickettsiosis, both ruled out.
Other spirochete-borne diseases could generate false positive results because of cross reactivity with the immunofluorescence for LD, like syphilis and leptospirosis, both were ruled out; also, autoimmune pathologies are less likely because of the clinical findings and the patient's evolution. Although the traditional geographic distribution of LD makes it less probable in our country, both the clinical findings and the laboratory data confirm the diagnosis of the first autochthonous case of LD in Costa Rica. This case must widen the diagnostic horizon of local infectology, in one hand with acute febrile pathologies with an epidemiologic antecedent suggestive of zoonoses, and in the other hand with chronic cardiovascular, neurologic and joint pathologies that lack of a better explanation. The emergence of this type of new diseases must accompany itself with a wide research work that justifies it. Field research must be made to find the vector and the reservoir implied, completing the cycle. It is of our interest to motivate research in this field.
Translated by: Javier Estrada ZeledónReferences
1. Burgdorfer W, Barbour AG, Hayes SF, Benach JL, Grunwaldt E y Davis JP. Lyme disease-a tick-borne spirochetosis? Science 1982; 216:1317-1379. [ Links ]
2. Kurtenbach K, Hanincová K, Tsao J, Margos G, Fish D y Ogden N H. Fundamental processes in the evolutionary ecology of Lyme borreliosis. Nature 2006; 4: 660–669. [ Links ]
3. Wormser G, et al. The clinical assessment, treatment, and prevention of Lyme disease, human granulocytic anaplasmosis, and babesiosis: clinical practice guidelines by the Infectious Diseases Society of America. ClinInfDis 2006; 43: 1089-1134. [ Links ]
4. Hengge U, Tannapfel A, Tyring S, Erbel R, Arendt G y Ruzicka T. Lyme borreliosis. THE LANCET Infectious Diseases 2003; 3:489–500. [ Links ]
5. Lelovas P, Dontas I, Bassiakou E y Xanthos T. Cardiac implications of Lyme disease, diagnosis and therapeutic approach. International Journal of Cardiology 2008; 129:15–21. [ Links ]
6. Aguero-Rosenfeld M, Wang G, Schwartz I y Wormser G P. Diagnosis of Lyme Borreliosis. ClinMicrob Rev 2005; 18:484-509. [ Links ]
7. Franz J. Lymedisease. Best Pract Res Clin Rheum 2003; 17: 241-264. [ Links ]
8. Aguero-Rosenfeld M. E. Lyme disease: Laboratory issues. Infect DisClin N Am 2008; 22:301-313. [ Links ]
9. Bratton RL, Whiteside JW, Hovan MJ, Engle R y Edwards FD. Diagnosis and treatment of Lyme disease. Mayo ClinProc 2008; 83:566–571. [ Links ]
10. Boza C Ricardo. Enfermedad de Lyme (Borreliosis de Lyme) en Costa Rica. Actamédicacostarric 2011; 53:34-36. [ Links ]
Received: April
5th, 2011 Accepted: November 17th , 2011











 text in
text in